Introduction
Clinical software solutions have fundamentally transformed the healthcare landscape by providing essential tools that enhance patient care and streamline operations. Technologies such as electronic health records and telemedicine platforms play a pivotal role in enabling healthcare providers to deliver timely and effective services.
However, as the integration of these systems becomes increasingly complex, organizations encounter significant challenges in maximizing their potential while navigating various obstacles.
To ensure that clinical software solutions not only address immediate needs but also foster long-term success, healthcare providers must adopt best practices that align with these evolving demands.
Define Clinical Software Solutions and Their Importance in Healthcare
Clinical software solutions are essential digital tools that empower medical providers to deliver efficient and effective care. Key components of clinical software solutions encompass:
- Electronic Health Records (EHRs)
- Practice management systems
- Telemedicine platforms
- Clinical decision support systems
Each plays a crucial role in healthcare delivery. EHRs, in particular, streamline workflows and enhance communication among healthcare professionals, significantly improving patient outcomes by ensuring timely access to critical information. For example, EHRs facilitate quick access to medical histories, which is vital for informed decision-making during consultations.
Recent advancements in EHR technology, such as AI integration for real-time clinical decision support and improved interoperability, have further augmented their effectiveness. A community hospital in Vermont reported a 60% reduction in near-miss medication events and a 25% decrease in the number of charts requiring retrieval for signing orders and dictated reports after implementing an EHR. This illustrates the tangible benefits these systems provide. Furthermore, statistics reveal that 63% of individuals experienced fewer medication errors with EHRs, while 75% of providers assert that their EHR enables them to deliver enhanced care, underscoring their role in improving safety.
As medical organizations navigate regulatory standards, EHRs ensure that individual data is managed securely and ethically. This reinforces the importance of adopting these technologies in contemporary medical practices.
Identify Essential Features of Effective Clinical Software Solutions
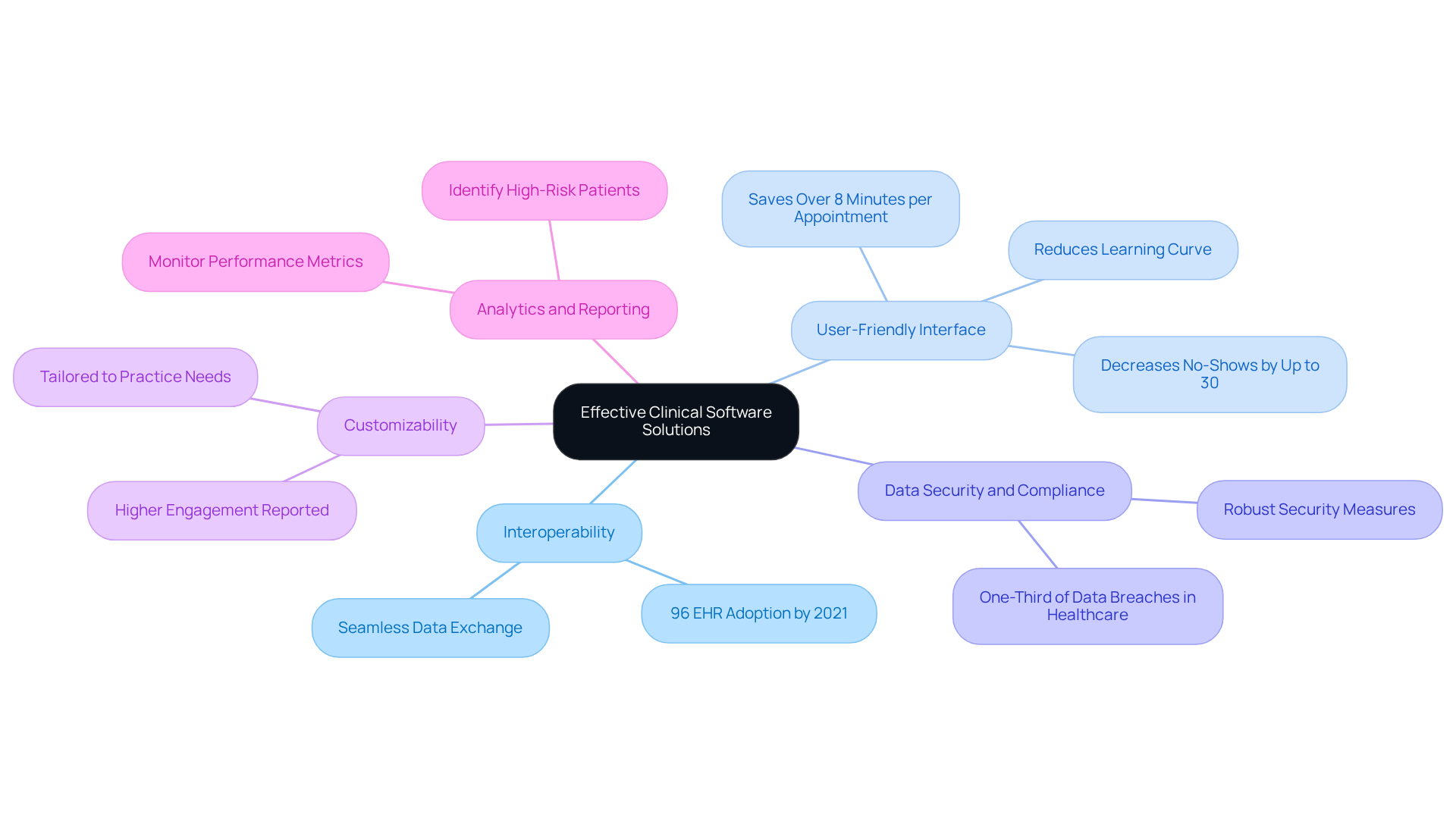
Effective clinical software solutions must incorporate several essential features to maximize their utility in healthcare settings:
- Interoperability: Seamless data exchange between systems is crucial for comprehensive health management. This capability ensures that medical providers can access complete individual histories, regardless of where treatment was received. Statistics indicate that 96 percent of non-federal acute treatment hospitals in the U.S. had implemented a certified EHR by 2021, underscoring the growing emphasis on interoperability in medical applications.
- User-Friendly Interface: A straightforward and intuitive interface significantly reduces the learning curve for medical personnel, allowing them to concentrate on patient care rather than navigating complex software. Case studies, particularly those involving small clinics, demonstrate that practices with user-friendly systems experience enhanced staff satisfaction and operational efficiency. Targeted automation can save over 8 minutes per appointment and decrease no-shows by up to 30%.
- Data Security and Compliance: Given the sensitive nature of medical data, robust security measures are imperative to protect patient information and comply with regulations such as HIPAA. Recent reports reveal that one-third of all reported data breaches occurred in the medical sector, highlighting the necessity for stringent security protocols.
- Customizability: Tailoring software to meet specific practice needs enhances its effectiveness and user satisfaction. Practices that adopt customizable solutions report higher engagement and improved alignment with operational workflows.
- Analytics and Reporting: Integrated analytics tools enable medical providers to monitor performance metrics, individual outcomes, and operational efficiency, fostering continuous improvement. Advanced analytics capabilities assist practices in identifying high-risk patients and reducing medical errors, ultimately leading to better health management.
By ensuring these attributes are present, medical organizations can select clinical software solutions that not only meet their immediate needs but also support long-term strategic objectives, particularly as the field of medical technology continues to evolve in 2026.
Implement Strategies for Successful Integration of Clinical Software Solutions
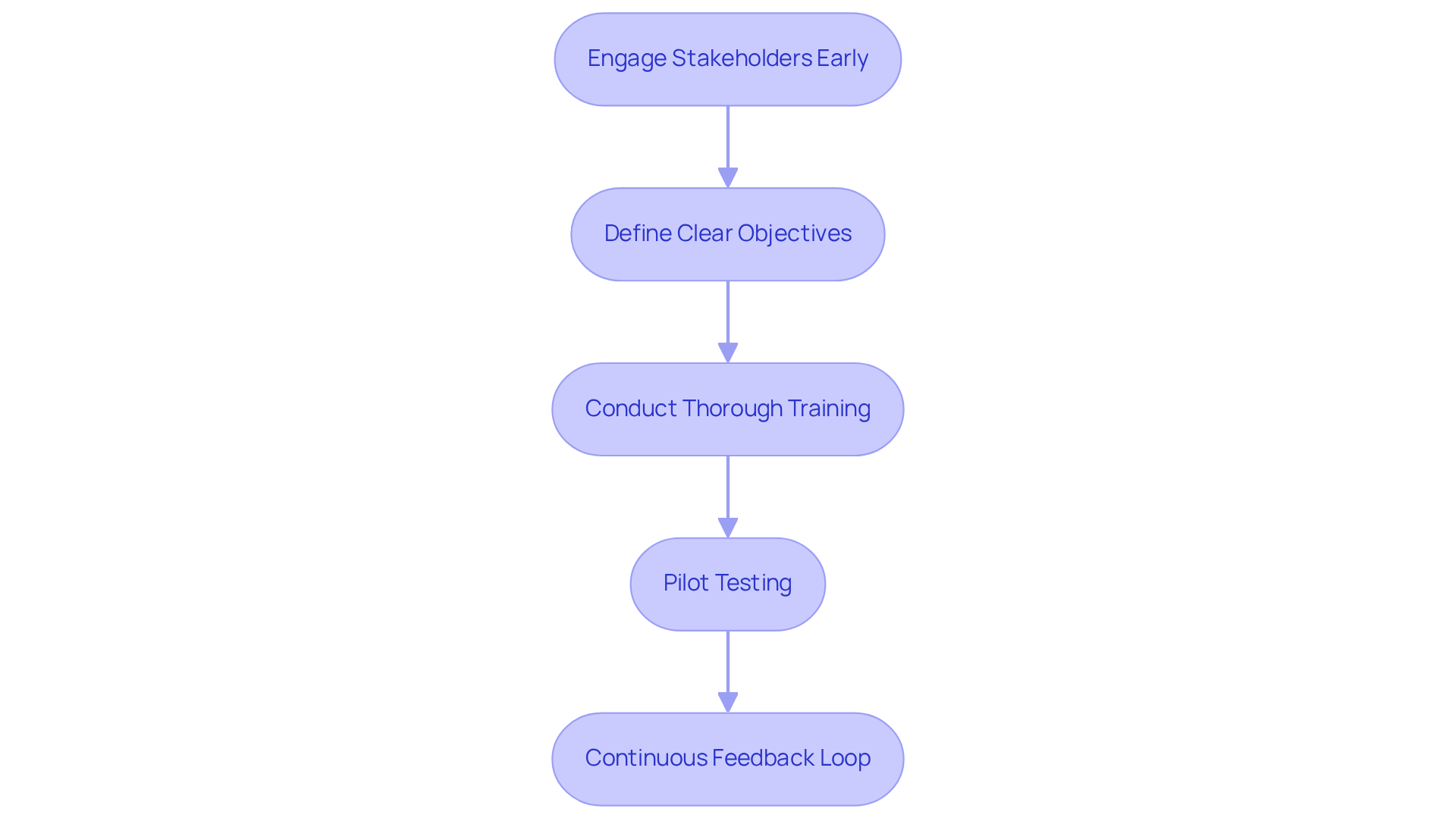
Successful integration of clinical software solutions relies on meticulous planning and execution. Key strategies to enhance this process include:
- Engage Stakeholders Early: Involving healthcare providers, IT staff, and administrative personnel from the outset ensures that the software aligns with the needs of all users. This early engagement is crucial; organizations that prioritize stakeholder involvement experience a significant improvement in integration success rates. For instance, streamlined charting in EHRs has been shown to increase efficiency by reducing administrative burdens on providers, underscoring the importance of user input in system design.
- Define Clear Objectives: Establishing specific goals for integration – such as improving health outcomes or minimizing administrative burdens – provides a focused direction for the project. Clear objectives facilitate success measurement and align efforts across teams. Organizations that treat interoperability as mere compliance risk falling behind competitors who leverage it for operational advantage by 2026.
- Conduct Thorough Training: Comprehensive training for all users is essential to foster comfort and proficiency with the new system. This may include hands-on workshops and ongoing support, which are vital for reducing resistance and enhancing user adoption. Case studies, such as those illustrating the role of digital intake and form management, demonstrate how effective training can streamline check-in processes and enhance overall satisfaction.
- Pilot Testing: Implementing the system in phases, starting with a pilot program, allows organizations to identify potential issues before a full rollout. This phased approach enables adjustments based on real-world feedback, significantly increasing the chances of a smooth transition. For example, the case study “From Data Exchange to Intelligent Workflows” illustrates how pilot testing can lead to improved operational efficiency.
- Continuous Feedback Loop: Establishing mechanisms for ongoing feedback from users is critical for identifying areas for improvement. This ensures that the program evolves to address the changing requirements of the organization and its clients. Organizations that integrate telehealth into their environments will enhance access without disrupting service experiences, demonstrating the value of ongoing engagement.
By following these strategies, medical organizations can significantly improve the likelihood of successful system integration, ultimately resulting in enhanced operational efficiency and better care outcomes through clinical software solutions.
Evaluate and Optimize Clinical Software Solutions for Long-Term Success
To ensure that clinical technology solutions remain effective over time, healthcare organizations must implement regular evaluation and optimization practices. This commitment is essential for maintaining the value of clinical software solutions while supporting high-quality patient care.
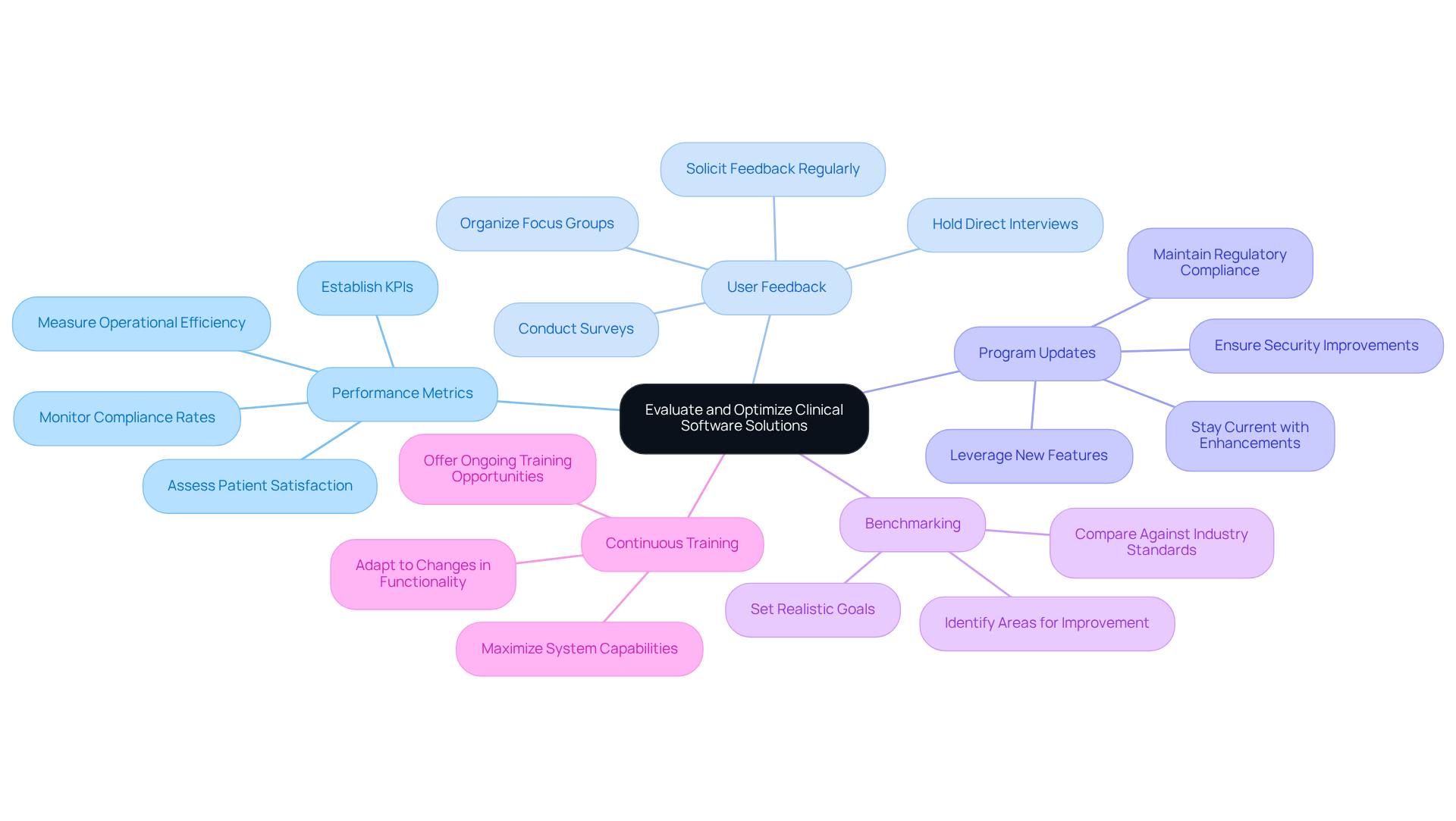
Performance Metrics: Establishing key performance indicators (KPIs) is crucial for assessing the effectiveness of applications in achieving desired outcomes. These outcomes may include patient satisfaction, operational efficiency, and compliance rates.
User Feedback: Regularly soliciting feedback from users helps identify pain points and areas for improvement. This can be accomplished through surveys, focus groups, or direct interviews, ensuring that user experiences inform ongoing enhancements.
Program Updates: Staying current with program updates and enhancements allows organizations to leverage new features and security improvements. Regular updates are also vital for maintaining compliance with evolving regulations, thereby safeguarding the integrity of clinical operations.
Benchmarking: Comparing performance against industry standards and best practices is essential for identifying areas for improvement. This benchmarking process aids in setting realistic goals for optimization and drives continuous enhancement efforts.
Continuous Training: Offering ongoing training opportunities for staff ensures they fully utilize the system’s capabilities and adapt to any changes in functionality. This investment in training is critical for maximizing the effectiveness of clinical software solutions.
Conclusion
Clinical software solutions play a crucial role in transforming healthcare delivery, enhancing efficiency, and improving patient outcomes. By integrating technologies such as Electronic Health Records (EHRs), telemedicine platforms, and clinical decision support systems, healthcare providers can streamline operations and ensure better access to critical patient information. The implementation of these solutions not only boosts operational efficiency but also fosters a safer environment for patient care.
Key aspects of effective clinical software solutions include essential features like:
- Interoperability
- User-friendly interfaces
- Data security
- Customizability
Successful integration strategies, such as:
- Engaging stakeholders
- Defining clear objectives
- Conducting thorough training
are vital for maximizing the benefits of these technologies. Continuous evaluation and optimization practices ensure that clinical software remains effective and aligned with evolving healthcare needs.
Embracing best practices in clinical software solutions represents more than just a technological upgrade; it signifies a commitment to enhancing healthcare delivery and patient safety. As the landscape of medical technology continues to evolve, healthcare organizations must prioritize these strategies to remain competitive and provide the highest quality of care. By investing in effective clinical software solutions, healthcare providers can significantly improve patient experiences and outcomes, ultimately contributing to a healthier society.
Frequently Asked Questions
What are clinical software solutions?
Clinical software solutions are digital tools that help medical providers deliver efficient and effective care. Key components include Electronic Health Records (EHRs), practice management systems, telemedicine platforms, and clinical decision support systems.
Why are clinical software solutions important in healthcare?
They are important because they streamline workflows, enhance communication among healthcare professionals, and improve patient outcomes by ensuring timely access to critical information.
How do Electronic Health Records (EHRs) improve healthcare delivery?
EHRs improve healthcare delivery by facilitating quick access to medical histories, which is vital for informed decision-making during consultations, and by enhancing communication among healthcare providers.
What recent advancements have been made in EHR technology?
Recent advancements include AI integration for real-time clinical decision support and improved interoperability, which enhance the effectiveness of EHRs.
Can you provide an example of the benefits of implementing EHRs?
A community hospital in Vermont reported a 60% reduction in near-miss medication events and a 25% decrease in charts requiring retrieval for signing orders and dictated reports after implementing an EHR.
What statistics support the effectiveness of EHRs in reducing medication errors?
Statistics show that 63% of individuals experienced fewer medication errors with EHRs, and 75% of providers believe their EHR enables them to deliver enhanced care.
How do EHRs contribute to data security and ethical management?
EHRs help medical organizations navigate regulatory standards, ensuring that individual data is managed securely and ethically, which is crucial in contemporary medical practices.
List of Sources
- Define Clinical Software Solutions and Their Importance in Healthcare
- Improved Diagnostics & Patient Outcomes (https://healthit.gov/health-it-basics/improved-diagnostics-patient-outcomes)
- Top Healthcare Software Solutions Every Clinic Needs in 2026 – eSEOspace (https://eseospace.com/blog/top-healthcare-software-solutions-every-clinic-needs-in-2026)
- The Future of Electronic Medical Records: 2026 Trends Every Healthcare Professional Should Know (https://ccitraining.edu/blog/up-and-coming-changes-in-electronic-medical-records)
- After three-year hiatus, VA to resume rollout of new electronic medical records system (https://militarytimes.com/news/pentagon-congress/2026/04/10/after-three-year-hiatus-va-to-resume-rollout-of-new-electronic-medical-records-system)
- Healthcare IT and EHR Trends to Watch in 2026: What Healthcare Leaders Need to Know (https://csicompanies.com/healthcare-it-and-ehr-trends-to-watch-in-2026-what-healthcare-leaders-need-to-know)
- Identify Essential Features of Effective Clinical Software Solutions
- 9 Essential Medical Software Features in 2026 (https://medesk.net/en/blog/medical-software-features)
- Top Healthcare Software Solutions Every Clinic Needs in 2026 – eSEOspace (https://eseospace.com/blog/top-healthcare-software-solutions-every-clinic-needs-in-2026)
- Key Features of Healthcare Practice Management Software (2026) (https://sprypt.com/blog/pms-features)
- Healthcare Software Development: A Practical Guide for 2026 (https://sotatek.com.au/blogs/healthcare-software-development)
- The Best EMR and EHR Software of 2026- businessnewsdaily.com (https://businessnewsdaily.com/10914-best-electronic-health-records-systems.html)
- Implement Strategies for Successful Integration of Clinical Software Solutions
- Healthcare IT and EHR Trends to Watch in 2026: What Healthcare Leaders Need to Know (https://csicompanies.com/healthcare-it-and-ehr-trends-to-watch-in-2026-what-healthcare-leaders-need-to-know)
- Top Healthcare Software Solutions Every Clinic Needs in 2026 – eSEOspace (https://eseospace.com/blog/top-healthcare-software-solutions-every-clinic-needs-in-2026)
- 2026 Healthcare Trends: Navigating Changes in a Shifting Landscape – Health IT Answers (https://healthitanswers.net/2026-healthcare-trends-navigating-changes-in-a-shifting-landscape)
- 10 Healthcare Technology Predictions Shaping 2026 | Carahsoft (https://carahsoft.com/blog/carahsoft-10-healthcare-technology-predictions-carahsoft-2026)
- Future of Healthcare Integration Technology in 2026 (https://emorphis.health/blogs/future-of-healthcare-integration-technology)
- Evaluate and Optimize Clinical Software Solutions for Long-Term Success
- 10 Healthcare Technology Predictions Shaping 2026 | Carahsoft (https://carahsoft.com/blog/carahsoft-10-healthcare-technology-predictions-carahsoft-2026)
- Healthcare IT and EHR Trends to Watch in 2026: What Healthcare Leaders Need to Know (https://csicompanies.com/healthcare-it-and-ehr-trends-to-watch-in-2026-what-healthcare-leaders-need-to-know)
- Top 5 Medical Software in 2026: Which Platforms Are Actually Changing the Game? – NewsBreak (https://local.newsbreak.com/finance-monthly-317425474/4513067833388-top-5-medical-software-in-2026-which-platforms-are-actually-changing-the-game)
- 2026 Medical Software Trends: How Providers Can Prepare for Rising Costs and AI Adoption (https://softwareadvice.com/resources/2026-medical-software-trends)
- Clinical Evaluation Requirements of Medical Device Software and Software As a Medical Device Including AI/ML-based Devices (ONLINE EVENT: Apr 28, 2026) (https://globenewswire.com/news-release/2026/04/13/3272645/28124/en/clinical-evaluation-requirements-of-medical-device-software-and-software-as-a-medical-device-including-ai-ml-based-devices-online-event-apr-28-2026.html)
