Introduction
Selecting the appropriate medical program software is a critical decision for healthcare organizations, as it profoundly impacts operational efficiency and patient care. Organizations can enhance their decision-making process by identifying essential selection criteria, including:
- Functionality
- User experience
- Compliance
- Vendor reputation
However, with the rapid advancement of technology and evolving regulatory standards, healthcare leaders must consider how to ensure that their chosen software not only addresses current needs but also adapts to future challenges. This article explores best practices for selecting and utilizing medical software, offering insights that empower healthcare providers to make informed decisions in a dynamic landscape.
Identify Key Selection Criteria for Medical Software
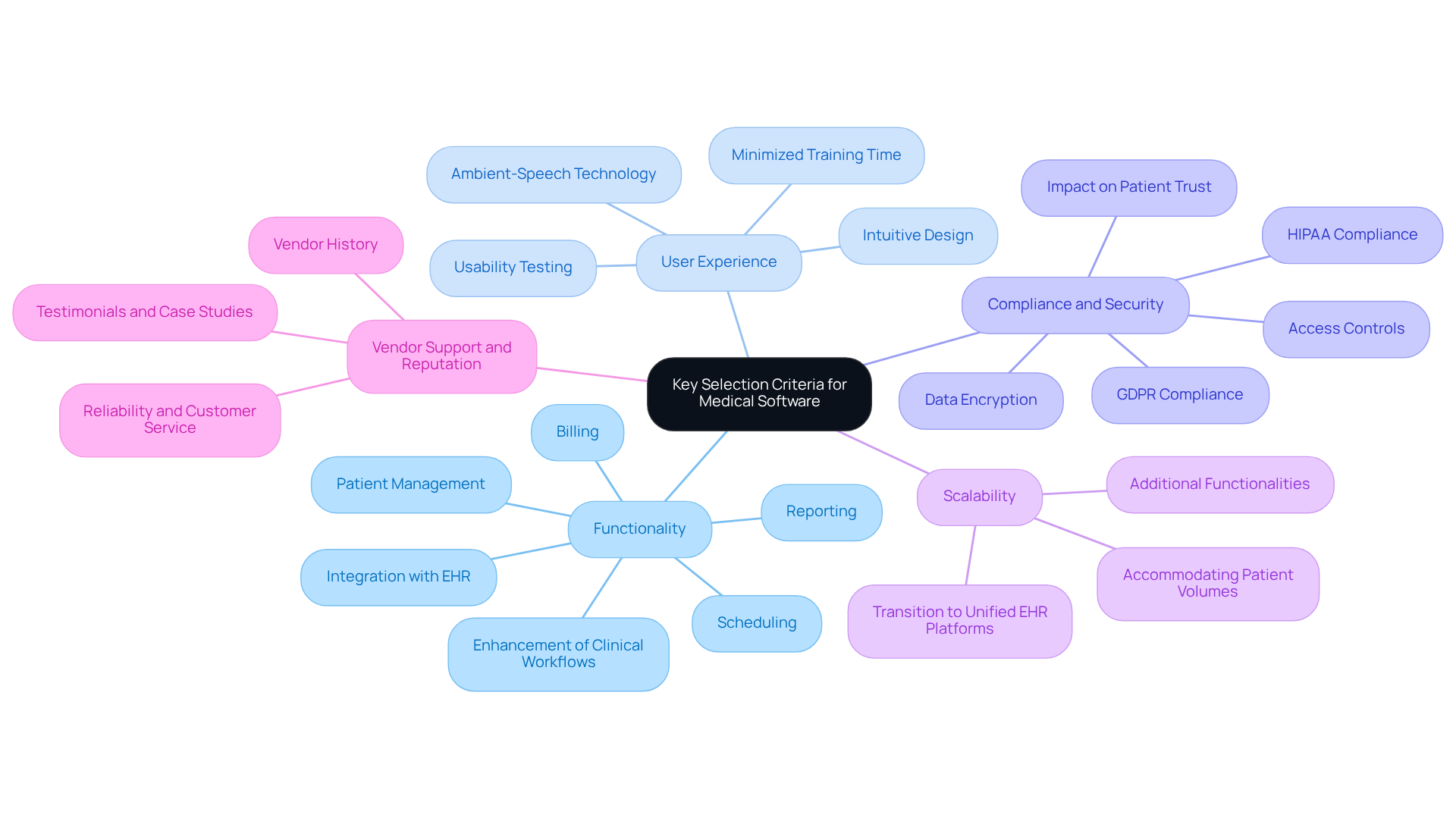
When selecting medical software, it is crucial to identify criteria that align with the specific needs of your organization. The following factors are essential to consider:
- Functionality: It is vital that the application supports essential functions such as patient management, billing, scheduling, and reporting. Evaluate its ability to integrate seamlessly with existing systems, including Electronic Health Records (EHR). According to the research, applications that enhance clinical workflows can significantly improve efficiency and provider wellness.
- User Experience: The application must be intuitive and user-friendly to minimize training time and enhance staff productivity. Conduct usability testing with potential users to gather valuable feedback. KLAS Research indicates that user experience impacts efficiency and provider wellness, underscoring the importance of user experience in system selection.
- Compliance: It is imperative to verify that the software meets regulatory standards. Assess its security features, including data encryption and access controls, to safeguard sensitive patient information. The importance of adherence cannot be overstated, as it directly impacts patient trust and organizational integrity. The 2026 General Wellness Guidance clarifies product classification and enforcement risk assessments, which are crucial for ensuring compliance.
- Scalability: Select software that can grow alongside your organization. It should accommodate increasing patient volumes and additional functionalities as your needs evolve. In 2026, many medical institutions are transitioning to unified EHR platforms, a significant trend that enhances scalability and operational performance.
- Vendor Support and Reputation: Investigate the vendor’s reputation within the medical sector. Look for testimonials and case studies that demonstrate their reliability and customer service. A vendor with a strong track record can provide the necessary support during implementation and beyond.
By establishing these criteria, medical organizations can streamline their selection process and ensure they choose software that enhances both efficiency and patient care.
Evaluate Regulatory Compliance and Standards
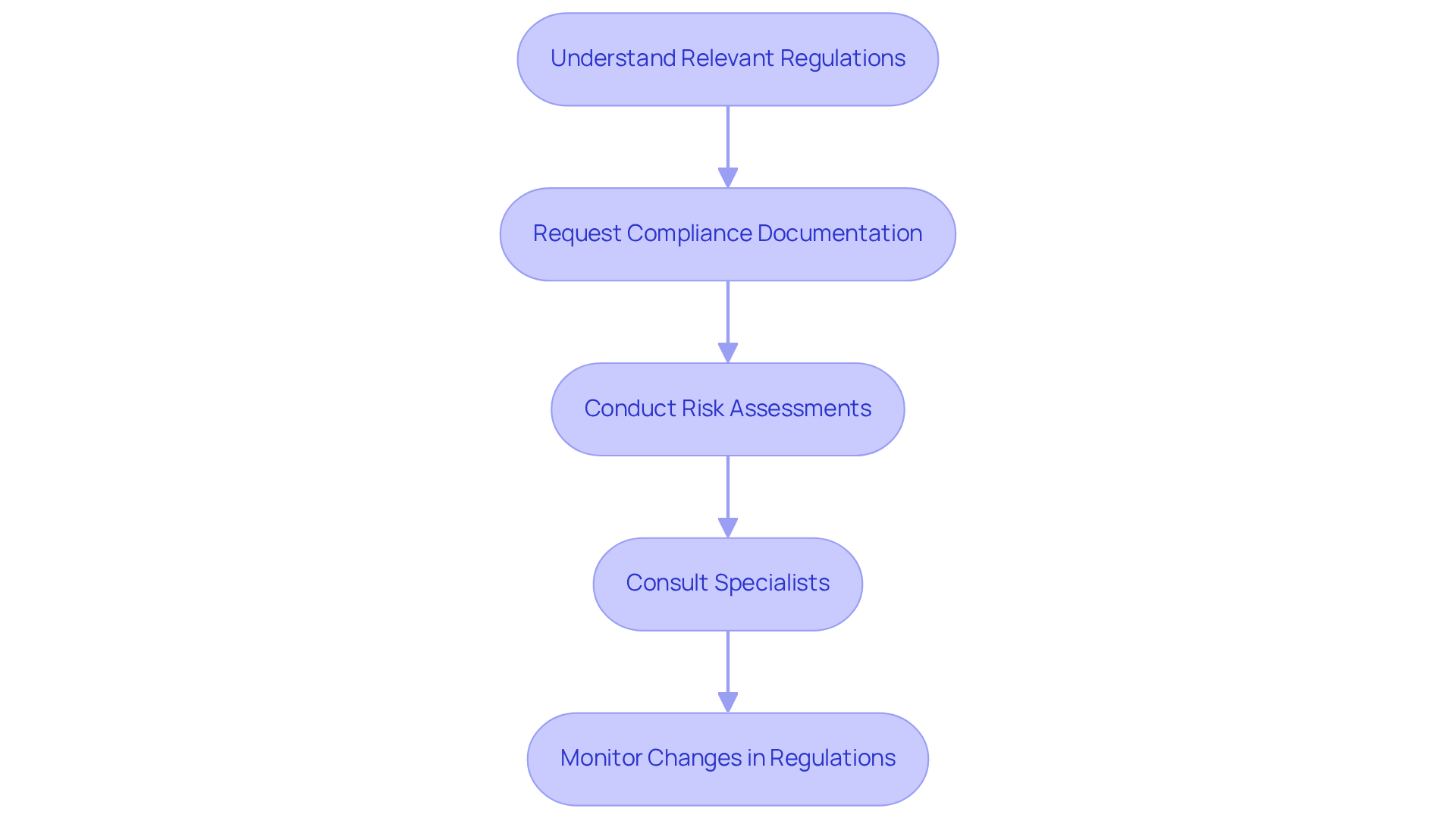
In the medical sector, compliance is essential. Understanding regulations is the first step. Familiarize yourself with guidelines such as HIPAA, HITECH, and FDA regulations that govern healthcare applications. It is crucial that the software adheres to these standards, as non-compliance can result in significant penalties, which may include fines and a loss of trust.
Next, request compliance documentation from vendors. This documentation should demonstrate the product’s compliance with industry standards. Certifications, audit reports, and assessments are vital for verifying adherence to HIPAA and GDPR standards.
Conducting regular audits is also necessary. Perform a thorough evaluation to identify potential vulnerabilities within the system. This assessment should include an analysis of data management practices and security protocols. Notably, 29% of medical providers cite regulatory pressures as a primary factor influencing their cybersecurity strategy.
Additionally, consider consulting specialists. Engaging experts or legal consultants who focus on compliance can ensure that all aspects of the application comply with regulatory standards. Their insights are invaluable, especially with the forthcoming 2026 regulations, for which the final rule publication is anticipated in early 2026, followed by a grace period of 180 days.
Finally, stay informed. Staying updated on alterations in medical regulations that may impact software adherence is crucial. Regularly assess and revise your adherence strategies, as healthcare entities must recover essential systems within 72 hours after an incident, a mandate shaped by HHS ransomware recommendations. This highlights the necessity for proactive adherence management.
By rigorously assessing compliance and standards, medical entities can protect patient data and uphold trust with stakeholders through the use of secure software.
Implement Best Practices for Software Utilization
To maximize the effectiveness of medical software, organizations should adopt several best practices:
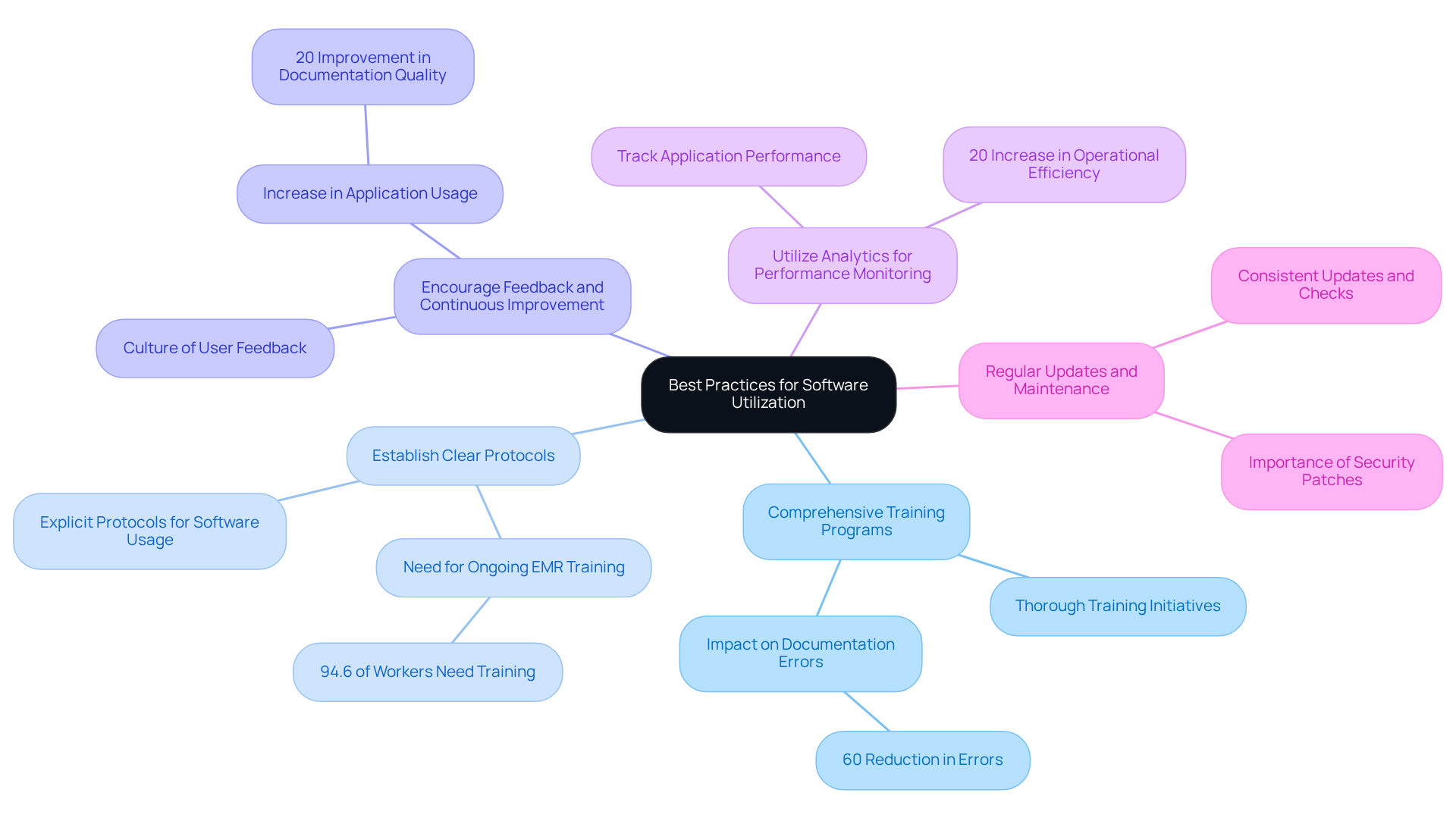
- Implement thorough training initiatives for all users, including administrative staff and healthcare providers. Training should encompass system functionalities, regulatory requirements, and best practices for data entry and management. Research indicates that well-trained staff can significantly reduce documentation errors; for instance, one clinic achieved a 60% reduction in errors through targeted training, underscoring the critical role of effective training in healthcare.
- Develop explicit protocols for software usage, detailing security measures, patient privacy practices, and reporting procedures. Ensuring that all personnel are familiar with these protocols is essential, as organizations with clear guidelines report enhanced compliance and fewer mistakes in data handling. Notably, 94.6% of healthcare workers express the need for ongoing EMR training, highlighting the necessity of clear protocols.
- Cultivate a culture that values feedback, allowing staff to report issues and suggest enhancements. Regularly reviewing this feedback can yield actionable insights, fostering an environment of continuous improvement. Research indicates that organizations actively seeking input experience a significant rise in application usage and satisfaction rates, with organized documentation techniques enhancing documentation quality by 20%.
- Utilize Analytics for Performance Monitoring: Leverage built-in analytics tools to track performance and user engagement. This data can assist in identifying areas requiring enhancement and ensuring that the system aligns with organizational objectives. Effective monitoring can lead to a 20% increase in productivity, as organizations can swiftly address any identified issues.
- Regular Updates and Maintenance: Schedule consistent updates and maintenance checks to keep the system compliant and functional. This includes applying security patches and upgrading features as necessary. Regular upkeep is crucial, as outdated systems can lead to vulnerabilities and compliance risks, which can significantly impact medical institutions in terms of finances and reputation.
By adopting these best practices, medical institutions can enhance the effectiveness of their clinical applications with improved training, ultimately resulting in improved patient care and outcomes.
Conduct Regular Reviews and Adaptations
To ensure that medical applications remain effective and compliant, organizations must conduct regular reviews. The following key steps outline this process:
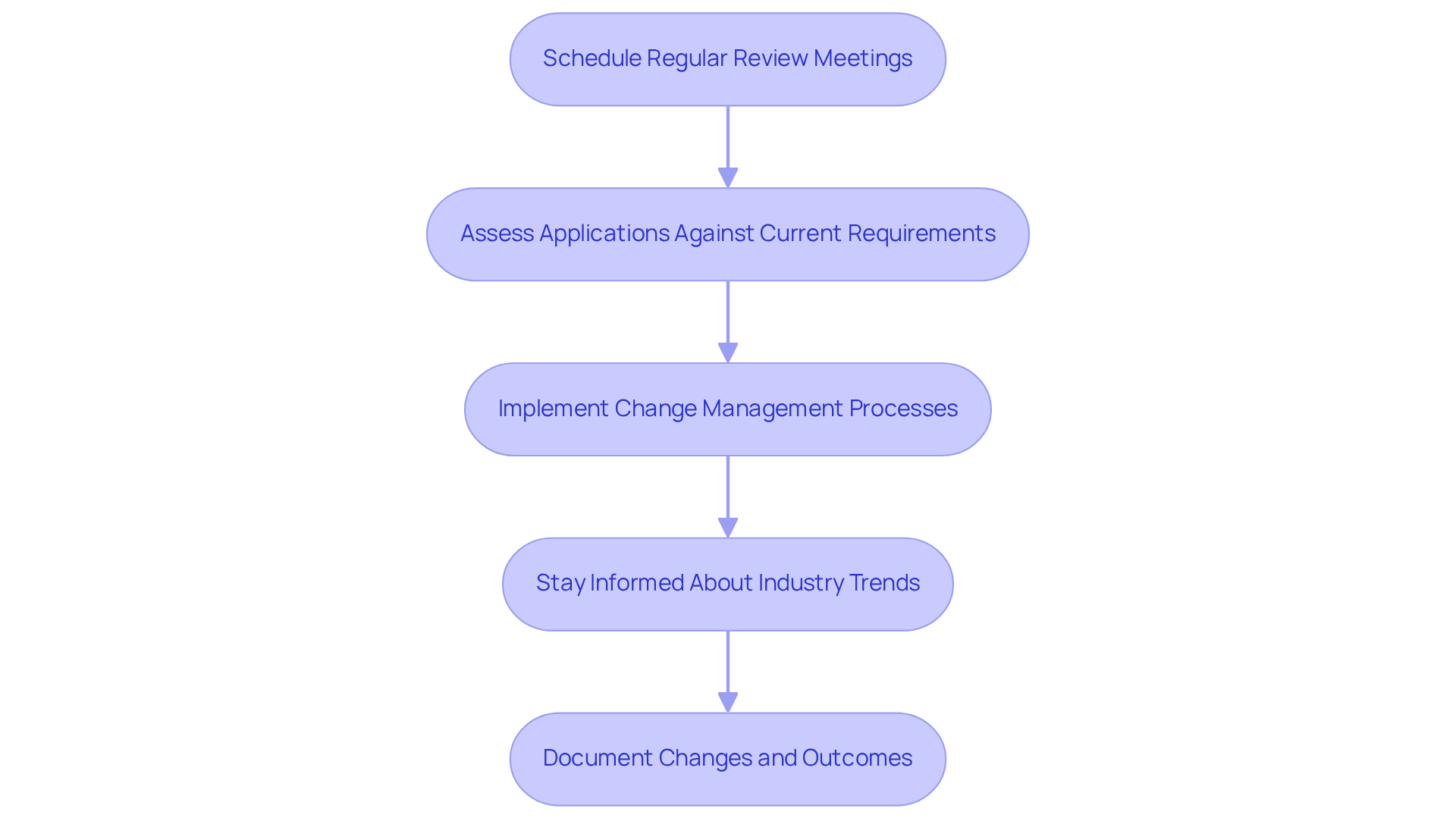
- Schedule Meetings: Establish a schedule for reviews with key stakeholders, including IT staff, compliance officers, and end-users. These meetings serve to evaluate program performance and gather feedback. As Jordan Brinkman notes, without a structured forum to review and discuss these metrics, the data loses its power.
- Assess Applications Against Current Requirements: Regularly evaluate whether the applications continue to meet the entity’s needs. This assessment should consider changes in patient volume, regulations, and technological advancements. Notably, 66% of life sciences executives plan to invest in generative AI by 2025, indicating a shift in focus that organizations must adapt to.
- Implement Change Management: Develop a structured change management process to guide adaptations to the system. This process should include assessing the impact of changes, communicating with stakeholders, and providing training on new features. Addressing challenges such as data quality, which 62% of AI professionals in the medical field cite as a top concern, is crucial for successful implementation.
- Monitor Industry Trends: Keep abreast of industry trends and developments that may affect technology utilization. This includes advancements in telehealth, data analytics, and patient engagement tools. With 57% of healthcare leaders identifying the reduction of administrative burdens through automation as a key opportunity for AI adoption, staying informed is essential.
- Maintain Documentation: Maintain thorough documentation of all modifications made to the system and the results of those modifications. This practice aids in future evaluations and ensures compliance with regulations. For instance, a multi-provider ophthalmology group identified unprofitable drugs through consistent KPI reviews, demonstrating the importance of thorough documentation.
By conducting regular reviews, medical providers can ensure that their applications remain effective and compliant with evolving standards. This proactive approach not only enhances operational efficiency but also positions organizations to capitalize on emerging opportunities in the healthcare landscape.
Conclusion
Selecting the appropriate medical program software is a pivotal decision for healthcare organizations, significantly impacting both operational efficiency and the quality of patient care. By concentrating on essential selection criteria – such as functionality, user experience, compliance, scalability, and vendor support – organizations can ensure they select a solution tailored to their unique needs, ultimately enhancing service delivery.
The article delineated critical aspects of software selection, underscoring the necessity of regulatory compliance and the implementation of best practices for effective use. Key points included:
- The importance of comprehensive training programs
- The establishment of clear protocols
- The encouragement of continuous feedback
- The execution of regular reviews to adapt to evolving requirements
These strategies are crucial for maximizing the software’s advantages and ensuring compliance with industry regulations.
In a rapidly evolving healthcare landscape, organizations must prioritize not only the initial selection of software but also its ongoing evaluation and adaptation. By embracing these best practices, healthcare providers can safeguard patient data, enhance operational efficiency, and position themselves to thrive amid emerging challenges and opportunities. Taking proactive measures now will lay the groundwork for a more effective and compliant healthcare environment in the future.
Frequently Asked Questions
What are the key selection criteria for medical software?
The key selection criteria for medical software include functionality, user experience, compliance and security, scalability, and vendor support and reputation.
Why is functionality important when selecting medical software?
Functionality is crucial because the application must support essential functions such as patient management, billing, scheduling, and reporting, and it should integrate seamlessly with existing systems like Electronic Health Records (EHR).
How does user experience affect the selection of medical software?
User experience is important as the application must be intuitive and user-friendly to minimize training time and enhance staff productivity. Usability testing with potential users can provide valuable feedback.
What compliance and security considerations should be taken into account?
It is essential to verify that the software complies with healthcare regulations such as HIPAA and GDPR, and to assess its security features, including data encryption and access controls, to protect sensitive patient information.
What does scalability mean in the context of medical software?
Scalability refers to the software’s ability to grow alongside the organization, accommodating increasing patient volumes and additional functionalities as needs evolve.
Why is vendor support and reputation important in selecting medical software?
Investigating the vendor’s history in the medical sector, along with testimonials and case studies, is important to ensure reliability and customer service during implementation and beyond.
How can establishing these selection criteria benefit medical organizations?
By establishing these criteria, medical organizations can streamline their selection process and ensure they choose software that enhances both operational efficiency and patient care.
List of Sources
- Identify Key Selection Criteria for Medical Software
- Healthcare IT Stats, Market Size and Trends Analysis Report (https://radixweb.com/blog/healthcare-it-statistics)
- Guide to Choosing the Best Healthcare Software in 2026 (https://safework.place/blog/best-healthcare-software)
- Healthcare IT and EHR Trends to Watch in 2026: What Healthcare Leaders Need to Know (https://csicompanies.com/healthcare-it-and-ehr-trends-to-watch-in-2026-what-healthcare-leaders-need-to-know)
- faegredrinker.com (https://faegredrinker.com/en/insights/publications/2026/1/key-updates-in-fdas-2026-general-wellness-and-clinical-decision-support-software-guidance)
- deliberatedirections.com (https://deliberatedirections.com/quotes-future-of-healthcare)
- Evaluate Regulatory Compliance and Standards
- Healthcare Regulations 2026: What’s Changing for Data Sharing and Privacy (https://xtalks.com/?p=196745)
- Saul Ewing 2026 Predictions and Prognostications for the Health Care Delivery System (https://saul.com/insights/alert/saul-ewing-2026-predictions-and-prognostications-health-care-delivery-system)
- 2026 HIPAA Changes: New Security Rule Requirements (https://hipaavault.com/resources/2026-hipaa-changes)
- Providers Evaluate Security as Updated HIPAA Compliance Looms (https://healthtechmagazine.net/article/2026/01/providers-evaluate-security-updated-hipaa-compliance-looms)
- HIPAA Updates and HIPAA Changes in 2026 (https://hipaajournal.com/hipaa-updates-hipaa-changes)
- Implement Best Practices for Software Utilization
- Tech Pros Predict Trends That Will Shape Healthcare In 2026 (https://forbes.com/councils/forbestechcouncil/2026/01/16/tech-pros-predict-trends-that-will-shape-healthcare-in-2026)
- medcitynews.com (https://medcitynews.com/2025/12/trends-in-health-it-what-should-organizations-prioritize-in-2026)
- Checking your browser – reCAPTCHA (https://pmc.ncbi.nlm.nih.gov/articles/PMC7813291)
- clinked.com (https://clinked.com/blog/ehr-best-practices)
- 5 Metrics to Measure EMR Training Success – GoLean Healthcare (https://golean.health/uncategorized/5-metrics-to-measure-emr-training-success)
- Conduct Regular Reviews and Adaptations
- Innovation and change management: 10 inspiring quotes (https://beeshake.com/en/innovation-et-conduite-du-changement)
- ventionteams.com (https://ventionteams.com/healthtech/ai/statistics)
- Change Management Quotes: Words of Wisdom (https://projectmanagertemplate.com/post/change-management-quotes-words-of-wisdom)
- Medical Practices Need Routine KPI & Financial Review Meetings and Why Review Alone Isn’t Enough (https://doctorsmanagement.com/blog/medical-practices-need-routine-kpi-financial-review-meetings-and-why-review-alone-isnt-enough)
