Introduction
In the dynamic realm of healthcare, the effectiveness of Electronic Medical Record (EMR) software is crucial for ensuring optimal patient care. By optimizing core functionalities, implementing comprehensive training, and leveraging advanced AI tools, healthcare providers can significantly enhance their operational effectiveness.
Many healthcare organizations struggle to adapt their EMR systems to meet evolving user expectations and technological innovations. Addressing these challenges is essential for healthcare organizations to maintain high standards of patient care in an ever-changing environment.
Understand Core Functionalities of EMR Software
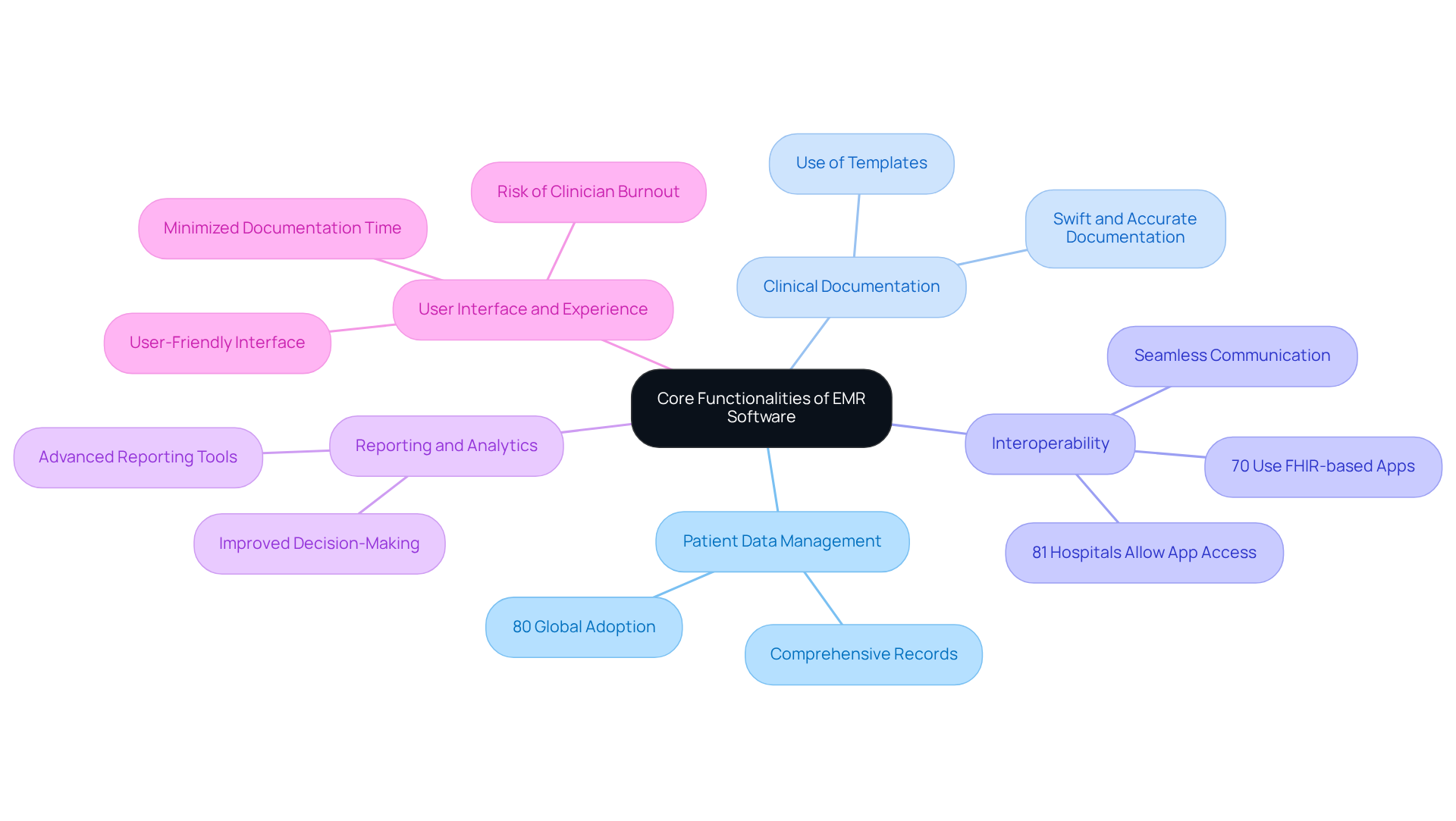
To enhance the efficiency of physician EMR software, it is essential to have a thorough understanding of its core functionalities. Key features include:
- Patient Data Management: EMRs must effectively manage patient demographics, medical histories, medications, and treatment plans, ensuring comprehensive and accurate records. Nearly 80% of healthcare providers globally have embraced digital records, highlighting the significance of efficient client information management.
- Clinical Documentation: The ability to document individual encounters swiftly and accurately is vital. Utilizing templates and structured data entry streamlines this process, enhancing productivity.
- Interoperability: EMRs should seamlessly communicate with other medical systems, facilitating coordinated care and reducing the risk of fragmented information. Significantly, 81% of hospitals allowed access through apps, with 70% utilizing FHIR-based applications, emphasizing the importance of interoperability in contemporary medical services.
- Reporting and Analytics: Advanced reporting tools allow medical providers to assess individual information, aiding improved decision-making and adherence to regulatory standards.
- User Interface and Experience: A user-friendly interface is essential for enhancing usability, minimizing documentation time, and increasing clinician satisfaction. Yet, poorly designed interfaces can really disrupt workflows and lead to clinician burnout.
This understanding enables providers to tailor their systems effectively, leading to improved patient outcomes and operational efficiency. As the healthcare landscape continues to evolve, the importance of effective patient data management using physician EMR software will only intensify, making these features crucial for success in the coming years.
Implement Comprehensive User Training Programs
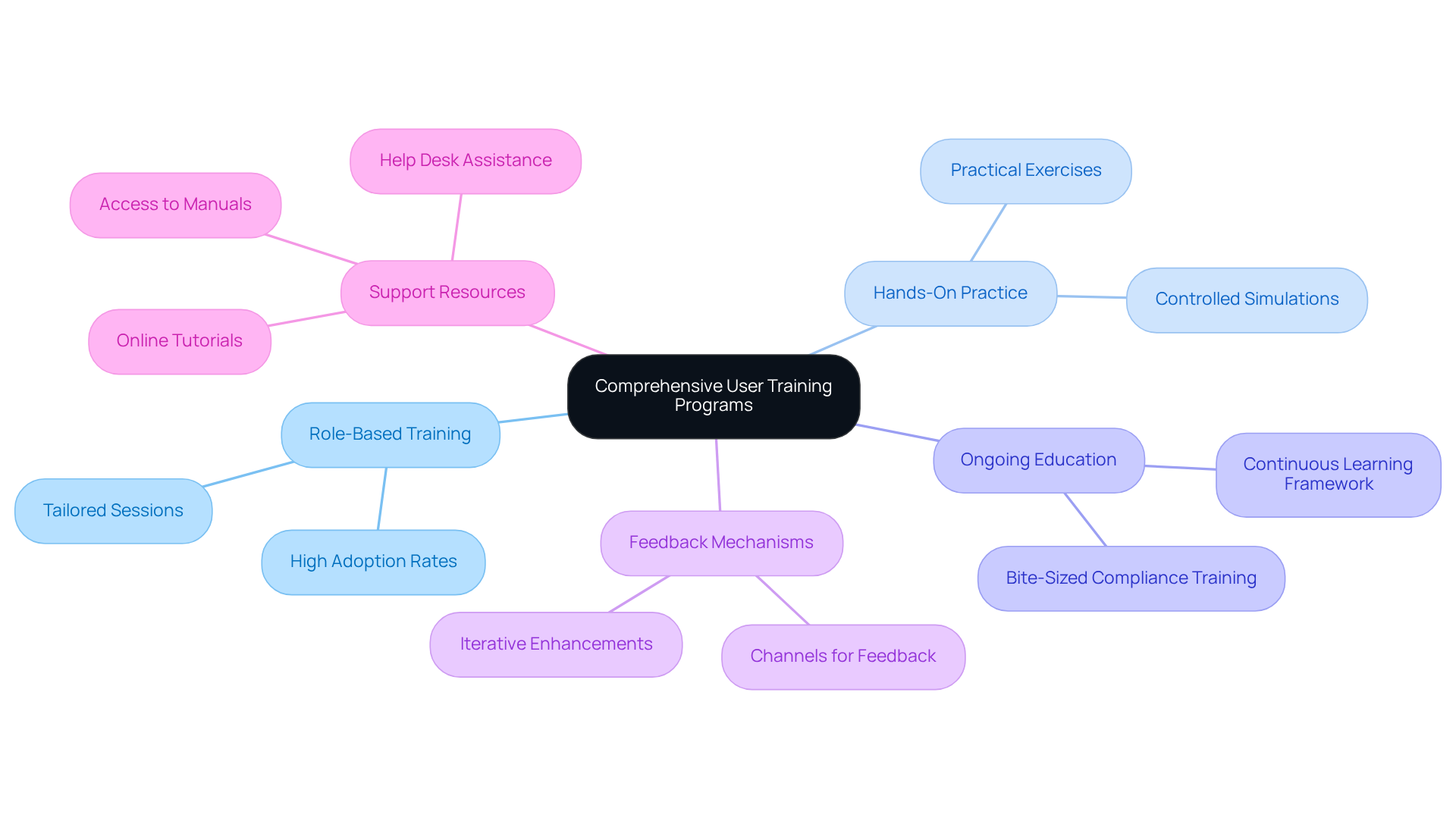
To maximize the effectiveness of EMR software, healthcare professionals must engage in thorough training programs that address specific user needs. Key components to consider include:
- Role-Based Training: Tailor training sessions to the specific roles of users, such as physicians, nurses, and administrative staff, to enhance relevance and effectiveness. High levels of participant adoption have been achieved within the first month of a comprehensive, role-based training program, demonstrating its effectiveness.
- Hands-On Practice: It’s important to include practical exercises and simulations, giving individuals a chance to practice in a controlled setting, which helps them feel more comfortable and proficient with the software.
- Ongoing Education: Establish a continuous learning framework that includes regular refresher courses and updates on new features or changes in the software. This ensures individuals remain informed and skilled. Compliance training is vital and is most effective when delivered in bite-sized formats via mobile platforms.
- Feedback Mechanisms: Establish channels for individuals to offer feedback on training effectiveness and software usability, promoting iterative enhancements in training programs. Rushed training can create obstacles that hinder effective software use.
- Support Resources: Provide access to manuals, online tutorials, and a help desk to assist individuals as they navigate the EMR system.
Investing in comprehensive training on physician EMR software significantly improves user proficiency, leading to enhanced efficiency and improved care for individuals. This investment not only enhances user proficiency but also directly contributes to improved patient care outcomes. As the healthcare landscape evolves, the importance of well-trained professionals cannot be overstated in ensuring quality patient care.
Leverage AI Tools for Enhanced EMR Functionality
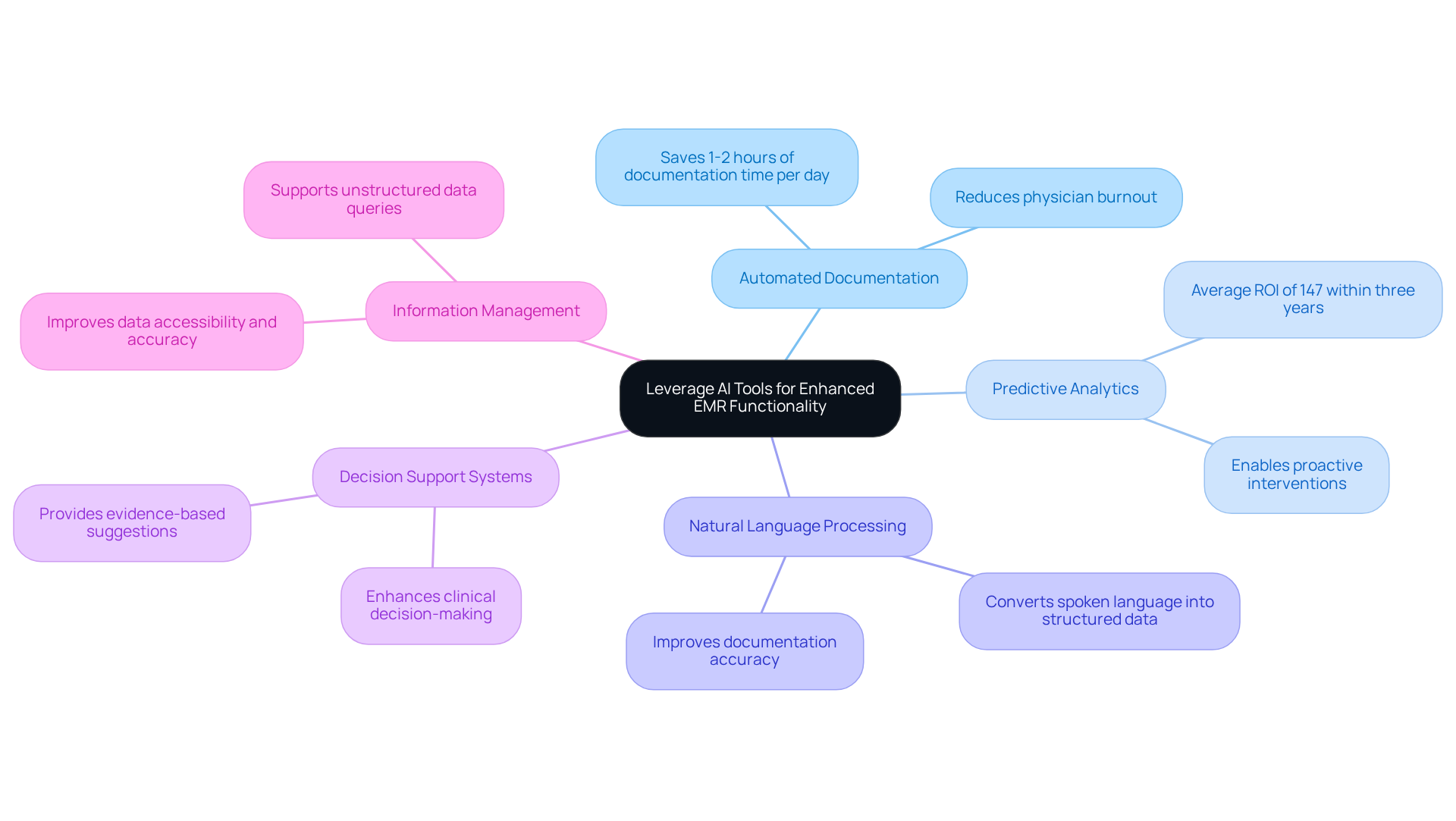
Integrating AI tools into EMR systems presents a pivotal opportunity to enhance functionality and efficiency in healthcare. Here are several ways to leverage AI:
- Automated Documentation: Healthcare providers often struggle with excessive documentation, which detracts from patient care; studies indicate that AI scribes can save them 1-2 hours of documentation time per day. This leads to increased efficiency and reduced burnout among physicians.
- Predictive Analytics: Implementing AI algorithms that analyze individual information can predict outcomes, enabling proactive interventions and customized care plans. This financial return underscores the value of investing in AI technologies, as healthcare organizations that integrate advanced analytics see an average ROI of 147% within three years.
- Natural Language Processing (NLP): Utilizing NLP to convert spoken language into structured data streamlines the documentation process and improves accuracy. This technology aids in capturing essential individual information that might otherwise be overlooked, ensuring thorough records.
- Decision Support Systems: Integrating AI-driven decision support tools offers clinicians evidence-based suggestions during client encounters. This capability enhances clinical decision-making and improves healthcare outcomes by providing clinicians with the latest information.
- Information Management: Utilizing AI improves information management capabilities, ensuring that records are precise, current, and easily accessible. With over 80% of medical data in EHRs being unstructured, AI tools that support native NoSQL and unstructured data queries can significantly enhance data utilization.
Healthcare organizations can enhance their operational efficiency and patient outcomes by optimizing their physician EMR software through the strategic use of AI tools. Ultimately, the strategic integration of AI tools can redefine operational paradigms in healthcare, paving the way for enhanced patient care.
Establish Continuous Evaluation and Feedback Loops
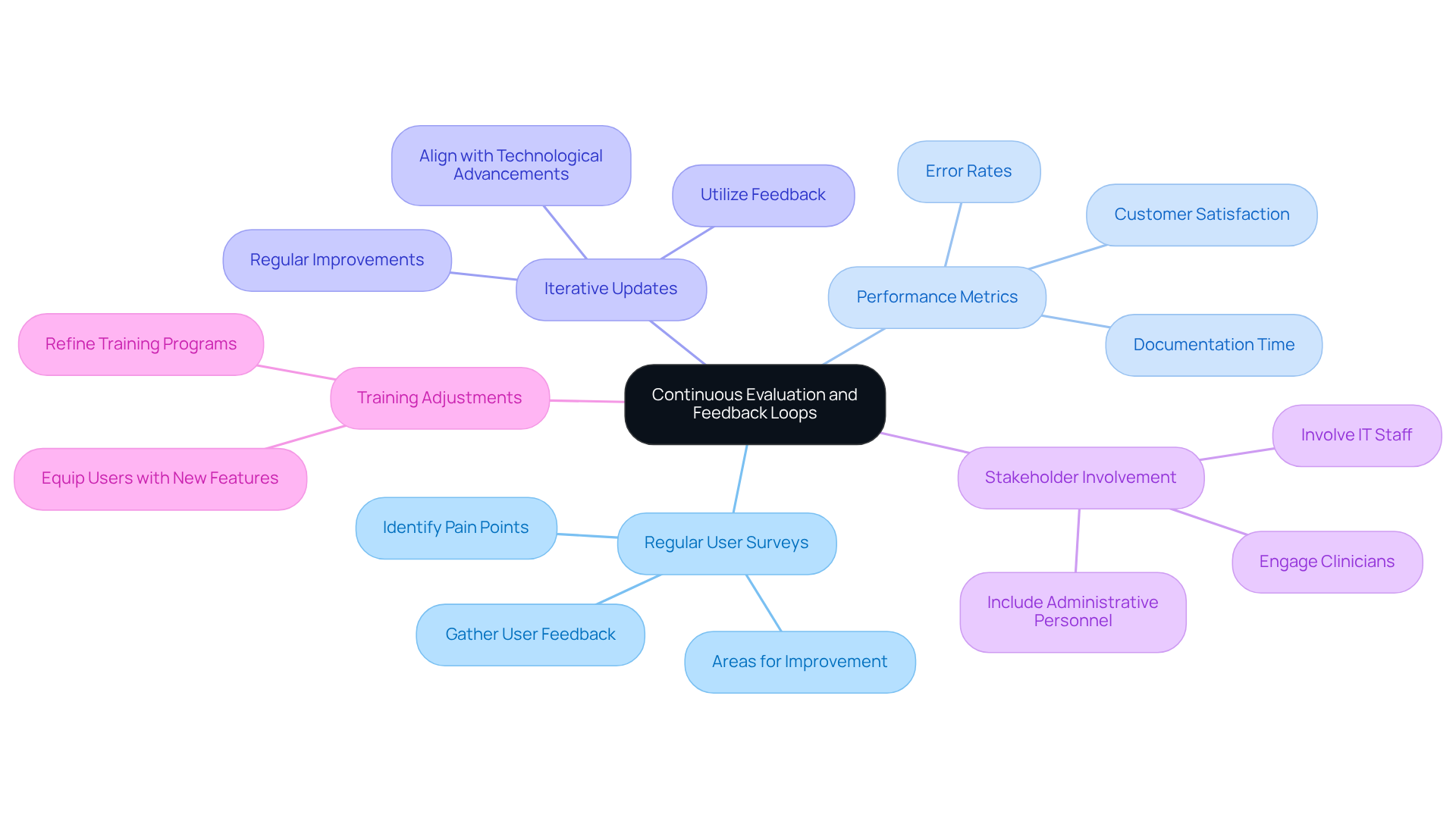
Many healthcare organizations struggle to keep their EMR systems aligned with user expectations and technological advancements. To maintain and enhance the efficiency of EMR software, it is essential to establish continuous evaluation and feedback loops. The following strategies are essential:
- Regular User Surveys: Conduct surveys to gather feedback from users about their experiences with the EMR system, identifying pain points and areas for improvement.
- Performance Metrics: Develop key performance indicators (KPIs) to assess the effectiveness of the EMR system, such as customer satisfaction, documentation time, and error rates.
- Iterative Updates: Utilize feedback and performance data to guide regular updates and improvements to the EMR system, ensuring it stays in line with the needs of those utilizing it and technological advancements.
- Stakeholder Involvement: Involve a diverse group of stakeholders, including clinicians, IT staff, and administrative personnel, in the evaluation process to gain a comprehensive understanding of system performance.
- Training Adjustments: Use evaluation results to refine training programs, ensuring that users are equipped to utilize new features and improvements effectively.
Ultimately, neglecting these evaluation strategies can compromise the quality of patient care delivered through EMR systems.
Conclusion
Enhancing the efficiency of physician EMR software is vital for improving healthcare delivery and patient outcomes. Healthcare organizations can enhance operational effectiveness and care quality by understanding EMR functionalities, implementing tailored user training, leveraging AI tools, and establishing continuous evaluation processes.
Key insights include:
- The necessity for tailored training programs that address specific user needs.
- The integration of AI technologies to streamline documentation and enhance decision-making.
- The importance of ongoing feedback mechanisms to ensure systems remain aligned with user expectations.
Each of these practices contributes to creating a more efficient, user-friendly environment that empowers healthcare professionals to focus on patient care rather than administrative burdens.
As the healthcare landscape evolves, adopting best practices for optimizing EMR software is essential for success. By prioritizing efficiency and user satisfaction, healthcare organizations can foster a culture of continuous improvement that ultimately leads to better patient experiences and outcomes. Committing to these strategies today ensures a more effective and responsive healthcare system in the future.
Frequently Asked Questions
What are the core functionalities of EMR software?
The core functionalities of EMR software include patient data management, clinical documentation, interoperability, reporting and analytics, and user interface and experience.
How does EMR software manage patient data?
EMR software effectively manages patient demographics, medical histories, medications, and treatment plans, ensuring comprehensive and accurate records.
Why is clinical documentation important in EMR software?
Clinical documentation is vital because it allows for the swift and accurate recording of individual encounters, enhancing productivity through the use of templates and structured data entry.
What is interoperability in the context of EMR software?
Interoperability refers to the ability of EMR systems to seamlessly communicate with other medical systems, facilitating coordinated care and reducing the risk of fragmented information.
How prevalent is the use of interoperability in hospitals?
Approximately 81% of hospitals allow access through applications, and 70% utilize FHIR-based applications, highlighting the significance of interoperability in modern medical services.
What role do reporting and analytics play in EMR software?
Advanced reporting tools in EMR software enable medical providers to assess individual information, which aids in improved decision-making and adherence to regulatory standards.
Why is user interface and experience important in EMR software?
A user-friendly interface enhances usability, minimizes documentation time, and increases clinician satisfaction, while poorly designed interfaces can disrupt workflows and lead to clinician burnout.
How does understanding EMR functionalities benefit healthcare providers?
A thorough understanding of EMR functionalities allows providers to tailor their systems effectively, leading to improved patient outcomes and operational efficiency.
List of Sources
- Understand Core Functionalities of EMR Software
- EMR Software Development in 2026: How It’s Transforming Healthcare Delivery (https://assuresoft.com/blog/tech-trends/emr-software-development-2026-how-its-transforming-healthcare-delivery)
- The Future of Electronic Medical Records: 2026 Trends Every Healthcare Professional Should Know (https://ccitraining.edu/blog/up-and-coming-changes-in-electronic-medical-records)
- Key Trends in EHR in 2026 Shaping Global Healthcare (https://riomed.com/key-trends-in-ehr-in-2026-shaping-global-healthcare)
- 30+ US Electronic Health Records (EHR) Adoption Statistics for 2026 (https://aptarro.com/insights/us-ehr-adoption-statistics)
- Implement Comprehensive User Training Programs
- Best Practices for Training Healthcare Staff During EMR System Transitions – MedSys Group (https://medsysgroup.com/best-practices-for-training-healthcare-staff-during-emr-system-transitions)
- Healthcare Training Programs Transforming Workforce Readiness In 2025 (https://elearningindustry.com/healthcare-training-programs-transforming-workforce-readiness)
- From EMR Training to Workforce Readiness: The New Standard for Digital Healthcare Adoption in 2026 (https://linkedin.com/pulse/from-emr-training-workforce-readiness-new-standard-c8qze)
- Tips for EMR Software Implementation in 2026 | EMRSystems Blog (https://emrsystems.net/blog/tips-for-emr-software-implementation-in-2026)
- Leverage AI Tools for Enhanced EMR Functionality
- Impact of artificial intelligence-based clinical documentation tools on clinical workflow – Mayo Clinic (https://mayoclinic.org/medical-professionals/physical-medicine-rehabilitation/news/impact-of-artificial-intelligence-based-clinical-documentation-tools-on-clinical-workflow/mqc-20590250)
- Top AI Tools in EMR Software in 2026 | EMRFinder Blog (https://emrfinder.com/blog/top-ai-tools-in-emr-software-in-2026)
- Best AI SOAP Note Generator – Free Trial | SOAPNoteAI (https://soapnoteai.com/soap-note-guides-and-example/healthcare-ai-trends-2026)
- Healthcare Analytics Statistics 2026: Key Data and Trends (https://knowi.com/blog/healthcare-analytics-statistics-2026)
- Studies find AI technology for clinical documentation aids efficiency and reduces burnout – School of Medicine and Public Health (https://med.wisc.edu/news/ambient-ai-improves-practitioner-well-being)
- Establish Continuous Evaluation and Feedback Loops
- Closing the feedback loop to drive patient experience improvements (https://pharmaphorum.com/views-and-analysis/closing-the-feedback-loop-to-drive-patient-experience-improvements)
- Improving EHR Systems with User Experience and Interface Design to Reduce Clinician Burnout and Enhance Workflow Efficiency | Healthcare IT Today (https://healthcareittoday.com/2024/12/19/improving-ehr-systems-with-user-experience-and-interface-design-to-reduce-clinician-burnout-and-enhance-workflow-efficiency)
- Closing the Loop on Patient Feedback: Lessons from CVS Health | AHA (https://aha.org/aha-center-health-innovation-market-scan/2024-04-16-closing-loop-patient-feedback-lessons-cvs-health)
- The Role of Patient Feedback Software in Enhancing Care Quality (https://certifyhealth.com/blog/why-every-practice-needs-patient-feedback-software-for-better-experiences)
