Introduction
As the healthcare industry increasingly relies on technology, the effective use of medical diagnostic software has become essential for improving patient outcomes. By understanding the core features and best practices for implementation, healthcare providers can fully leverage these tools, resulting in enhanced diagnostic accuracy and streamlined workflows. However, with the rapid evolution of technology and the complexities of integration, medical professionals must consider how to utilize these systems to their fullest advantage while ensuring the protection of sensitive patient information.
Understand Core Features of Medical Diagnostic Software
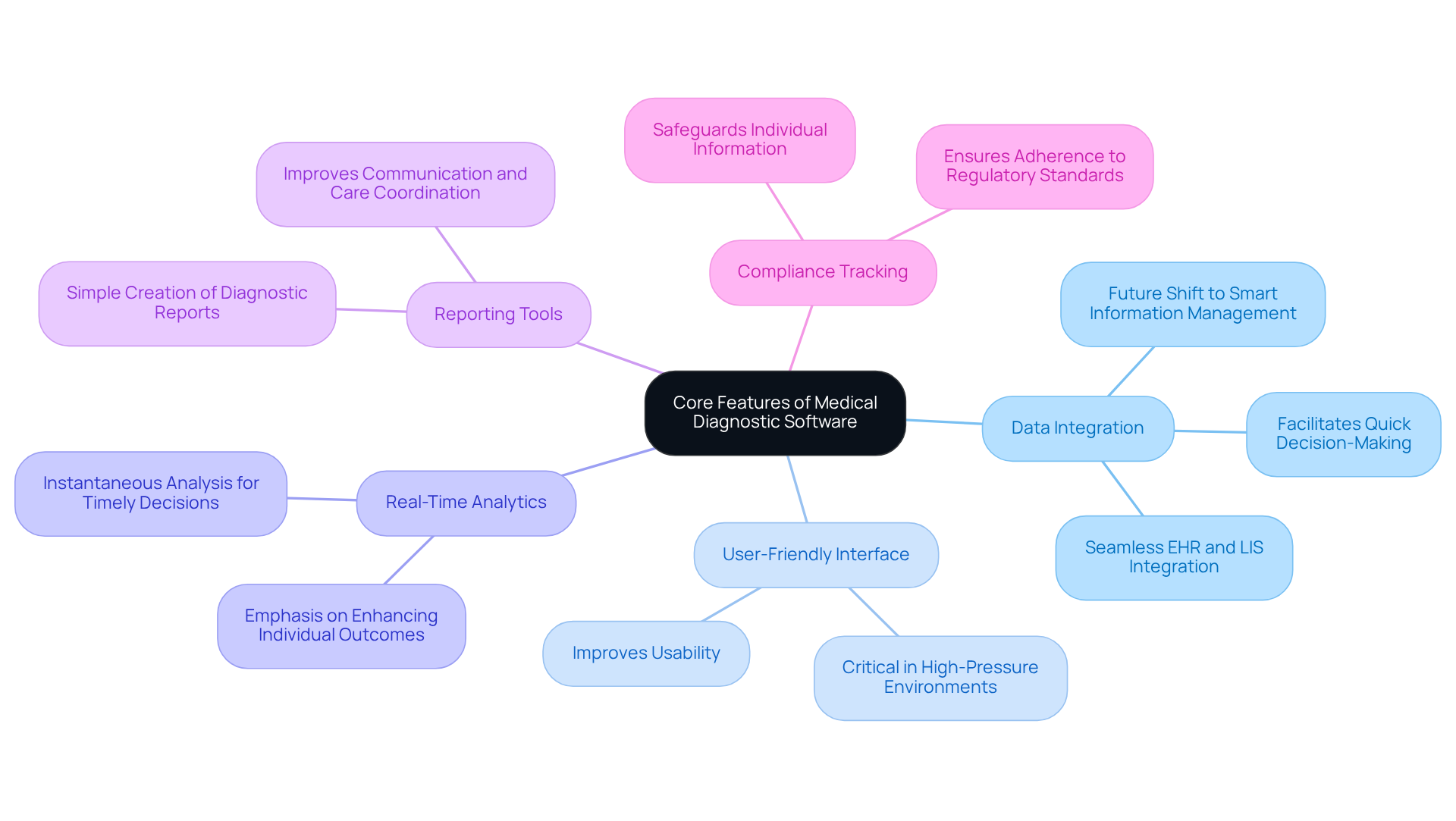
To maximize the effectiveness of medical diagnostic software, users must first understand the core features of the software. Key functionalities typically include:
- Data Integration: Seamless integration with existing electronic health records (EHR) and laboratory information systems (LIS) is crucial. This capability ensures that all patient information is accessible in one location, facilitating quicker decision-making and enhancing the overall quality of care. In 2026, the medical field will shift to smart information management with immediate validation and quality scoring, making information integration even more crucial.
- User-Friendly Interface: A well-crafted interface improves usability, enabling medical professionals to navigate the software effectively. This is particularly critical in high-pressure environments where time is of the essence.
- Real-Time Analytics: Features that offer instantaneous analysis enable clinicians to make timely decisions based on the most current information regarding individuals and diagnostic results. In 2026, medical organizations are anticipated to emphasize real-time analytics to enhance individual outcomes, reinforcing the need for effective data integration.
- Reporting Tools: Extensive reporting features allow simple creation of diagnostic reports, which can be shared with individuals and other healthcare providers. This functionality improves communication and care coordination, essential for effective treatment pathways.
- Compliance Tracking: Built-in compliance features are vital for ensuring that the application adheres to regulatory standards, such as HIPAA. This compliance is crucial for safeguarding individual information and preserving confidence in digital health solutions.
Grasping these features allows medical providers to utilize medical diagnostic software effectively, resulting in increased diagnostic accuracy and better patient care. As medical services progress towards smart information management, the incorporation of these functionalities will be crucial in addressing contemporary needs. Additionally, incorporating APIs and robust security measures will further enhance the effectiveness of data integration strategies.
Integrate with Existing Healthcare Systems for Seamless Workflow
To ensure that medical diagnostic software enhances clinical workflows, seamless integration with existing healthcare systems is essential. Achieving this integration involves several best practices:
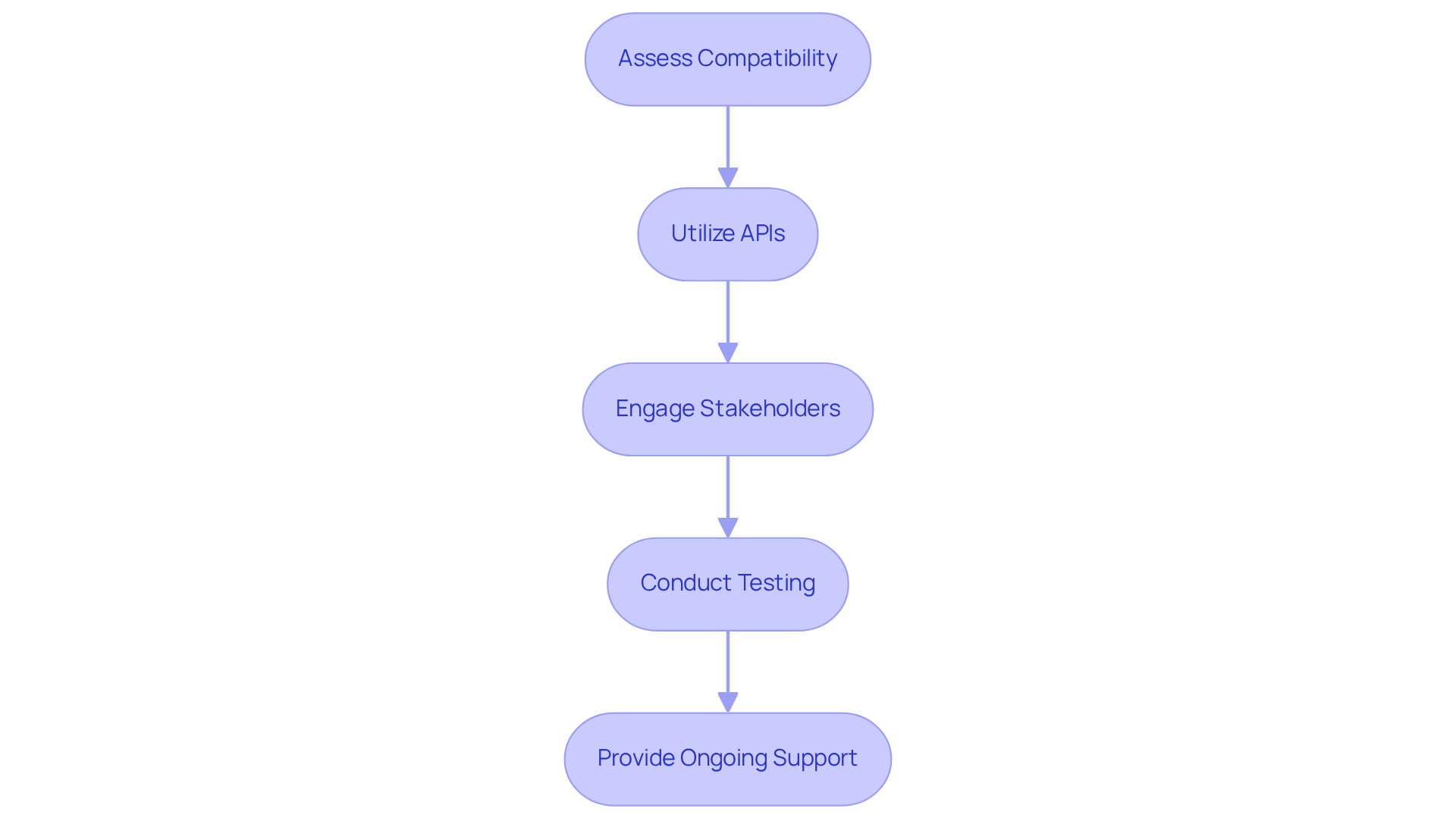
- Assess Compatibility: Evaluate the compatibility of diagnostic software with current Electronic Health Records (EHR) and Laboratory Information Systems (LIS) before implementation. This assessment helps identify potential integration challenges early, ensuring a smoother transition.
- Utilize APIs: Leverage application programming interfaces (APIs) to facilitate information exchange between systems. APIs simplify the integration process, allowing real-time information availability and improving operational efficiency. In 2022, 80% of non-federal acute care hospitals reported utilizing APIs to allow individuals access to health information through applications, and approximately 70% of hospitals facilitated access to user data through standards-based APIs, demonstrating their essential role in contemporary medical services.
- Engage Stakeholders: Involve key stakeholders, including IT staff, clinicians, and administrative personnel, in the integration process. Their insights are invaluable for tailoring the integration to meet the specific needs of the healthcare facility, fostering a collaborative environment that enhances healthcare delivery.
- Conduct Testing: Prior to full deployment, conduct thorough testing of the integrated systems to identify and resolve any issues. This step is essential for ensuring that the software operates as intended in a live environment, minimizing disruptions to care.
- Provide Ongoing Support: After integration, offer continuous support and training to users. This guarantees that staff can effectively utilize the integrated systems and address any challenges that arise, ultimately enhancing outcomes for individuals.
By adhering to these practices, healthcare organizations can attain a seamless workflow that enhances diagnostic capabilities through the use of medical diagnostic software and elevates care, paving the way for a more connected and efficient healthcare ecosystem.
Ensure Data Security and Compliance with Regulatory Standards
Essential elements of medical diagnostic software include data security and regulatory compliance. To safeguard sensitive patient information, consider the following best practices:
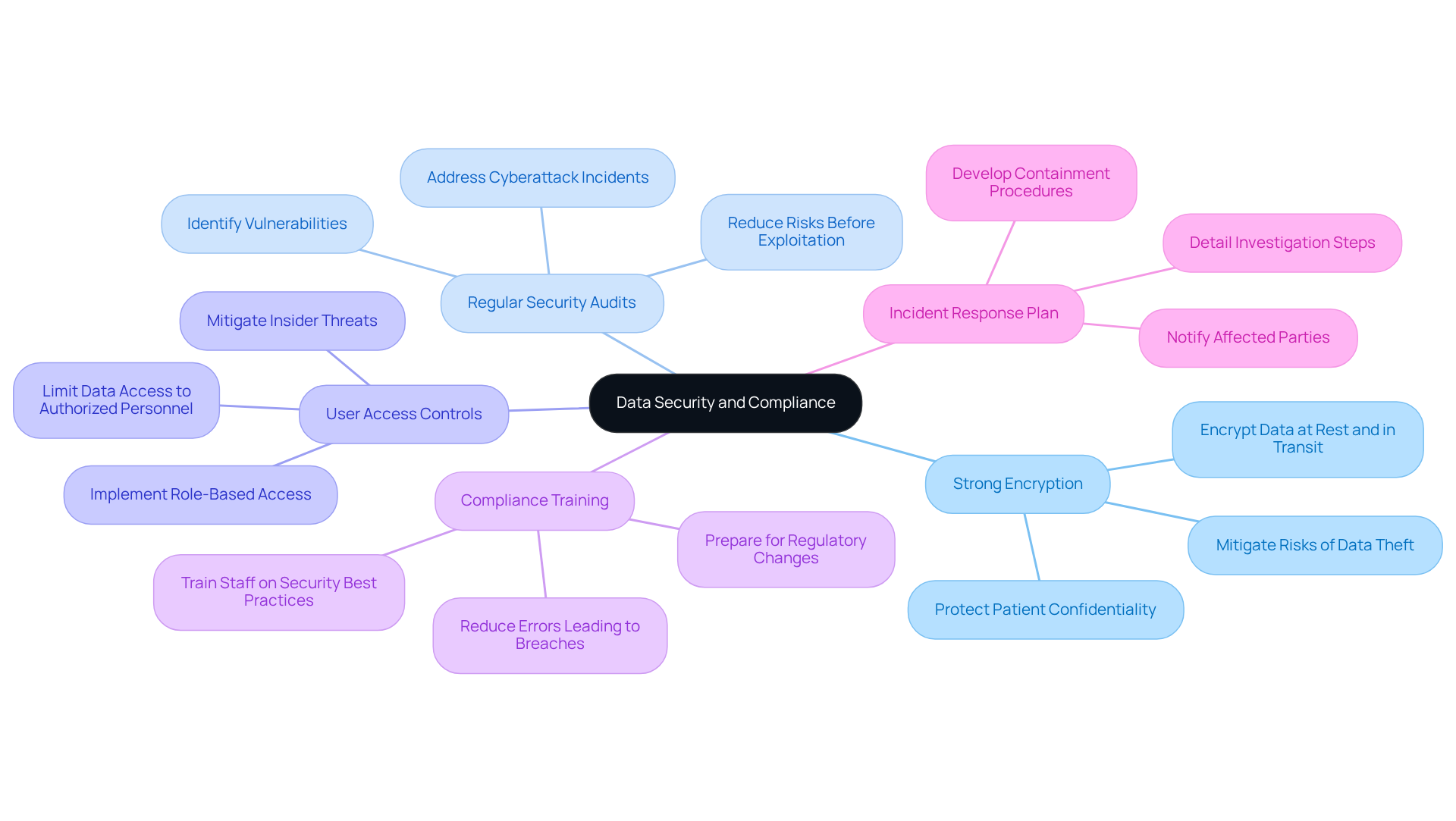
- Implement Strong Encryption: Employ encryption for data both at rest and in transit. This measure is crucial for protecting sensitive information from unauthorized access, thereby maintaining patient confidentiality. Given that patient records can fetch hundreds of dollars per file on illicit markets, robust encryption is non-negotiable.
- Regular Security Audits: Conducting regular security audits is vital for identifying vulnerabilities within the software. Addressing these vulnerabilities promptly can significantly reduce risks before they are exploited. Notably, nearly all medical organizations experienced at least one cyberattack in the past year, with an average of over 40 incidents per organization.
- User Access Controls: Establishing strict user access controls is imperative to limit who can view and modify sensitive information. Implementing role-based access ensures that only authorized personnel can access specific data, thereby mitigating the risk of insider threats and negligence-two leading causes of breaches in healthcare settings.
- Compliance Training: Providing continuous training for staff on information security best practices and regulatory requirements, such as HIPAA, is essential. With anticipated regulatory changes in May 2026, well-informed staff are less likely to make errors that could lead to information breaches, which have been linked to increased complications in medical procedures and longer hospital stays for patients.
- Incident Response Plan: Developing and maintaining an incident response plan is crucial for addressing potential breaches swiftly. This plan should detail the steps for containment, investigation, and notification to affected parties, ensuring that organizations can respond effectively to incidents that may disrupt patient care.
By prioritizing data security and compliance, medical organizations can protect their patients and ensure the integrity of their medical diagnostic software processes.
Provide Comprehensive Training and Support for Users
To ensure healthcare professionals effectively utilize medical diagnostic tools, comprehensive training and support are essential. Implementing effective training programs involves several best practices:
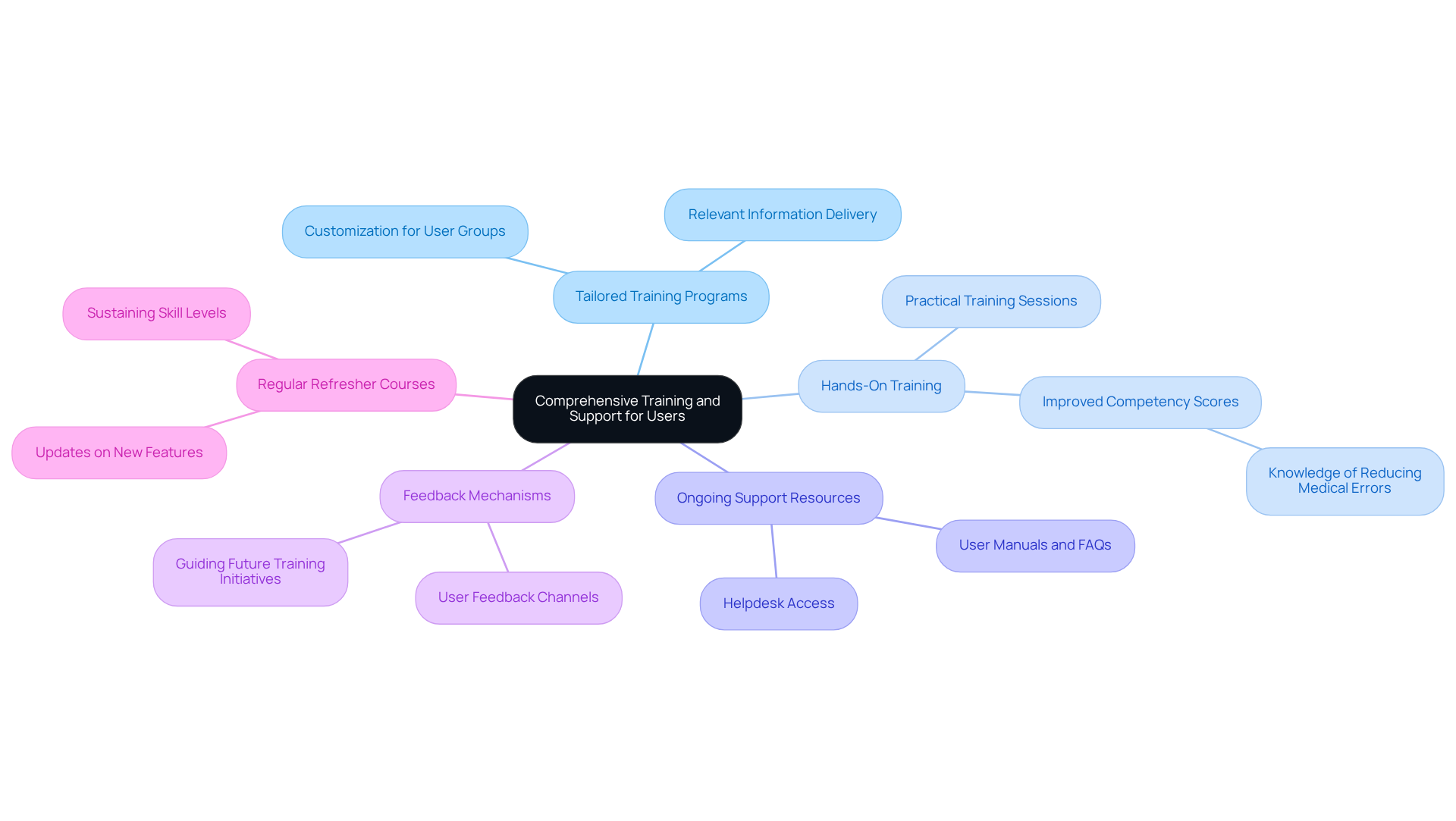
- Tailored Training Programs: It is crucial to develop training initiatives specifically designed for various user groups, including clinicians, administrative staff, and IT personnel. This customization ensures that each group receives relevant information, thereby enhancing their understanding and use of the system.
- Hands-On Training: Incorporating practical training sessions allows users to engage with the application in a controlled environment. Such experiential learning significantly boosts confidence and proficiency. A study demonstrated that hands-on training improved wellness staff’s knowledge and competencies related to electronic health records (EHR) usage, achieving 100% competency scores post-training. Notably, knowledge of reducing medical errors improved from 35.7% pre-intervention to 85.7% post-intervention (p = 0.02), underscoring the effectiveness of hands-on training.
- Ongoing Support Resources: Providing continuous support resources, including user manuals, FAQs, and helpdesk access, is vital for assisting users as they navigate the application. This support is crucial for quickly resolving issues and maintaining productivity, particularly in high-pressure healthcare settings.
- Feedback Mechanisms: Establishing channels for user feedback on both the application and training programs is essential. Collecting insights from users can guide future training initiatives and system updates, ensuring that the tools remain relevant and effective.
- Regular Refresher Courses: Offering periodic refresher courses keeps users informed about new features and best practices. Ongoing education is critical for sustaining high levels of skill and involvement, especially as technology evolves and medical practices transform.
As stated by the Wellness Center-Rawdat Al-Khail Health Center, “This tailored, hands-on training has been well received and effectively improved wellness staff knowledge, competencies, and satisfaction relative to EHR functionalities.” By investing in comprehensive training and support, healthcare organizations can empower their staff to effectively utilize medical diagnostic software, ultimately enhancing patient care and improving operational efficiency.
Conclusion
Maximizing the potential of medical diagnostic software relies on a comprehensive understanding of its core features and the implementation of effective practices. By emphasizing data integration, user-friendly interfaces, real-time analytics, compliance tracking, and robust security measures, healthcare professionals can significantly enhance diagnostic accuracy and patient care. The successful integration of these tools into existing healthcare systems is crucial for creating seamless workflows, ultimately improving the quality of care provided.
Key insights highlight the necessity of thorough integration processes, which include:
- Assessing compatibility
- Utilizing APIs
- Engaging stakeholders
- Offering ongoing support
Furthermore, prioritizing data security through strong encryption, regular audits, and user access controls is essential for maintaining patient confidentiality and adhering to regulatory standards. Comprehensive training and support are equally important, as tailored programs and hands-on training empower healthcare staff to effectively utilize these technologies, ensuring they remain competent and confident in their roles.
As the healthcare landscape continues to evolve, adopting these best practices in medical diagnostic software will not only enhance operational efficiency but also significantly influence patient outcomes. Healthcare organizations are encouraged to invest in these strategies, fostering a culture of continuous improvement and adaptation to meet the ever-changing demands of the medical field. By doing so, they can ensure that their diagnostic capabilities are both effective and reliable, ultimately leading to better health outcomes for individuals and communities alike.
Frequently Asked Questions
What are the core features of medical diagnostic software?
The core features typically include data integration, a user-friendly interface, real-time analytics, reporting tools, and compliance tracking.
Why is data integration important in medical diagnostic software?
Data integration is crucial as it allows seamless access to patient information from electronic health records (EHR) and laboratory information systems (LIS), facilitating quicker decision-making and enhancing the overall quality of care.
How does a user-friendly interface benefit medical professionals?
A well-crafted interface improves usability, enabling medical professionals to navigate the software effectively, which is particularly important in high-pressure environments where time is critical.
What role do real-time analytics play in medical diagnostic software?
Real-time analytics provide instantaneous analysis, allowing clinicians to make timely decisions based on the most current information about individuals and diagnostic results, thereby enhancing individual outcomes.
What are the benefits of reporting tools in medical diagnostic software?
Extensive reporting features enable the simple creation of diagnostic reports that can be shared with patients and other healthcare providers, improving communication and care coordination essential for effective treatment pathways.
Why is compliance tracking necessary in medical diagnostic software?
Built-in compliance features ensure adherence to regulatory standards, such as HIPAA, which is vital for safeguarding individual information and maintaining confidence in digital health solutions.
How will medical diagnostic software evolve by 2026?
By 2026, the medical field is expected to shift towards smart information management, emphasizing immediate validation, quality scoring, and real-time analytics to enhance individual outcomes, making data integration increasingly vital.
What additional features are important for enhancing data integration strategies?
Incorporating APIs and robust security measures will further enhance the effectiveness of data integration strategies in medical diagnostic software.
List of Sources
- Understand Core Features of Medical Diagnostic Software
- applause.com (https://applause.com/blog/4-digital-health-trends-that-will-define-healthcare-in-2026)
- In 2026, healthcare data will show a unified view of the patient (https://healthcareitnews.com/news/2026-healthcare-data-will-show-unified-view-patient)
- Top 5 Emerging Trends in Clinical Diagnostics for 2026 (https://blog.sekisuidiagnostics.com/dxdialogue/top-5-trends-clinical-diagnostics-2026)
- Healthcare Data Integration Trends: Top 2026 Insights for CIOs (https://vorro.net/top-healthcare-data-integration-trends-in-2026-every-cio-must-know)
- Integrate with Existing Healthcare Systems for Seamless Workflow
- White House, Tech Leaders Commit to Create Patient-Centric Healthcare Ecosystem | CMS (https://cms.gov/newsroom/press-releases/white-house-tech-leaders-commit-create-patient-centric-healthcare-ecosystem)
- API Integration: Connecting the Dots in Healthcare | Access (https://accesscorp.com/blog/api-integration-connecting-the-dots-in-healthcare)
- Hospital Use of APIs to Enable Data Sharing Between EHRs and Apps (https://healthit.gov/data/data-briefs/hospital-use-apis-enable-data-sharing-between-ehrs-and-apps)
- Healthcare Software Integration: Key Challenges & Benefits (https://talentica.com/blogs/healthcare-software-integration)
- EHR Integration in 2026: Challenges, Benefits, and Implementation (https://vcdoctor.com/blog/ehr-integration)
- Ensure Data Security and Compliance with Regulatory Standards
- 2026 HIPAA Security Rule Update: New Requirements to Prepare For | Medcurity (https://medcurity.com/hipaa-security-rule-2026-update)
- Cybersecurity in healthcare 2026: Protecting patients and preserving care amid rising threats | Insights | Elliott Davis (https://elliottdavis.com/insights/cybersecurity-in-healthcare-2026-protecting-patients-and-preserving-care-amid-rising-threats)
- January 2026 OCR Cybersecurity Newsletter (https://hhs.gov/hipaa/for-professionals/security/guidance/cybersecurity-newsletter-january-2026)
- Healthcare Compliance News (https://hipaajournal.com/category/healthcare-compliance)
- Provide Comprehensive Training and Support for Users
- Integrating Digital Health in Medical Education for Future Healthcare Training | Medical News Bulletin (https://medicalnewsbulletin.com/integrating-digital-health-in-medical-education-for-future-healthcare-training)
- 93 hospital and health system simulation and education programs to know | 2026 (https://beckershospitalreview.com/hospital-management-administration/93-hospital-and-health-system-simulation-and-education-programs-to-know-2026)
- Revolutionizing Medical Training with Technology – Infuse Med (https://infusemed.com/revolutionizing-medical-training-with-advanced-technology)
- The Impact of Training on Electronic Health Records Related Knowledge, Practical Competencies, and Staff Satisfaction: A Pre-Post Intervention Study Among Wellness Center Providers in a Primary Health-Care Facility – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC10243608)
- Scalable Training for Healthcare Teams in 2026 and Beyond – Lumeto (https://lumeto.com/blog/scalable-training-for-healthcare-teams)
