Introduction
Healthcare integration software is pivotal in modern medical technology, serving as a crucial link that connects diverse healthcare systems and enhances information flow. By facilitating streamlined data exchange across platforms, these tools not only improve care coordination but also enhance patient outcomes and ensure compliance with regulatory standards.
Nevertheless, the path to successful integration is laden with challenges, including interoperability issues and staff resistance. How can healthcare organizations effectively navigate these complexities and fully leverage integration software to transform patient care?
Define Healthcare Integration Software and Its Importance
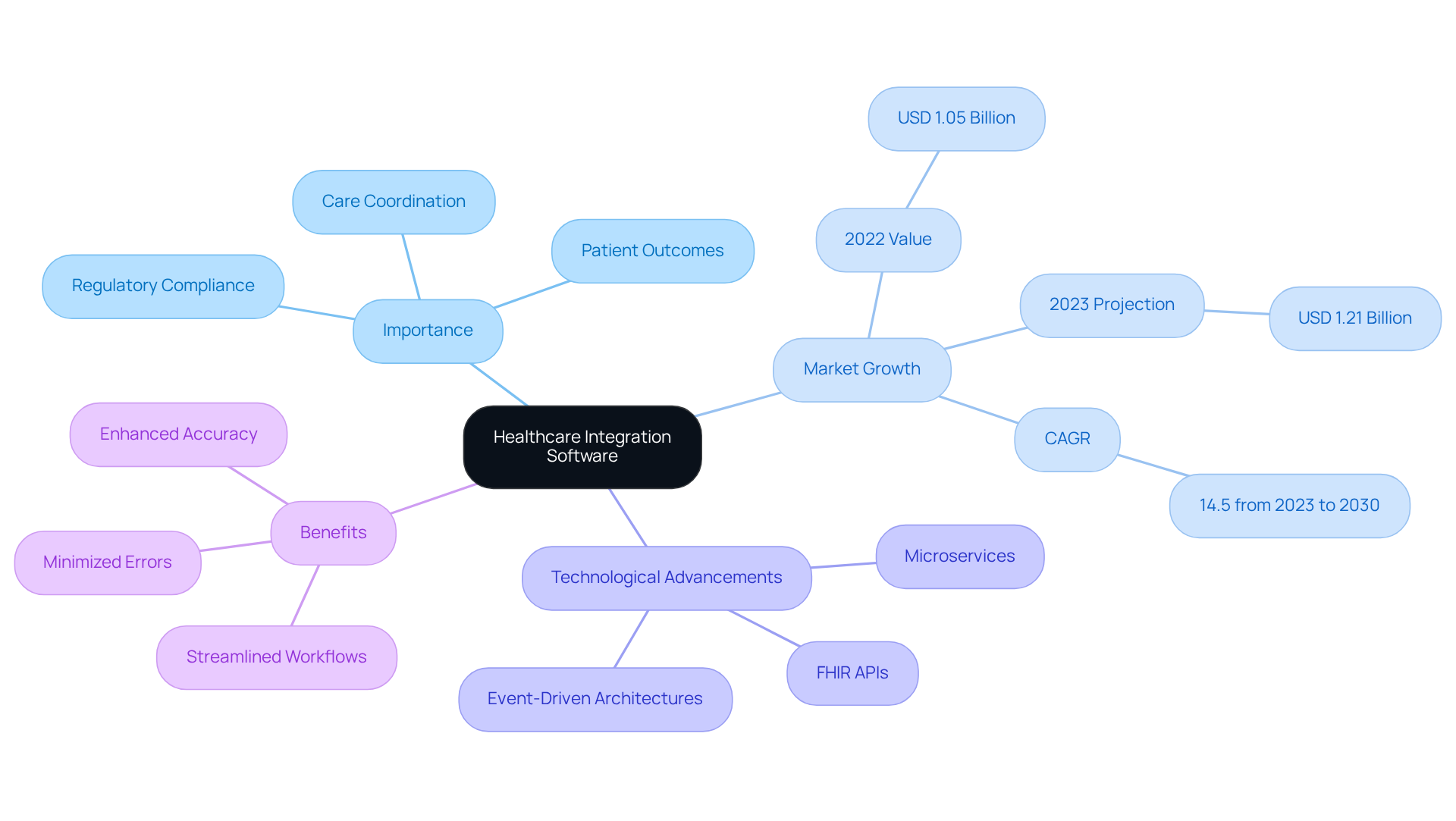
Healthcare integration software includes platforms and applications designed to connect various medical IT solutions, facilitating seamless data exchange and communication across diverse networks. The use of healthcare integration software is crucial for enhancing care coordination, improving patient outcomes, and ensuring compliance with regulatory standards. By promoting interoperability, healthcare integration software enables efficient sharing of patient information among electronic health records (EHRs), laboratory platforms, billing applications, and other medical tools.
The significance of healthcare integration software is substantial; it streamlines workflows, minimizes the risk of errors, and enhances accuracy, ultimately leading to improved patient care. For example, integrated frameworks can significantly reduce the time medical providers spend on administrative tasks, allowing them to concentrate more on patient engagement and support. In fact, the medical data unification market was valued at USD 1.05 billion in 2022 and is projected to grow to USD 1.21 billion in 2023, reaching USD 3.11 billion by 2030, with a compound annual growth rate (CAGR) of 14.5% from 2023 to 2030. This trend underscores the growing recognition of the value of these systems, particularly as North America accounted for over 38% of the global revenue in 2022.
Recent advancements in medical system software, such as the adoption of FHIR APIs and event-driven architectures, are revolutionizing the operations of medical organizations. These technologies facilitate immediate responses to clinical events, thereby enhancing the overall efficiency of medical services. Successful examples of healthcare integration software demonstrate that organizations employing these systems can achieve improved patient outcomes, optimize operations, and maintain compliance with evolving regulatory standards. Notably, the hospital sector represented more than 51% of the medical information unification market in 2022, highlighting the critical role hospitals play in this domain. Furthermore, the tools sector dominated the market with over 69% share of global revenue in 2022, emphasizing the importance of information unification tools in medical IT.
Identify Essential Features for Effective Integration Software
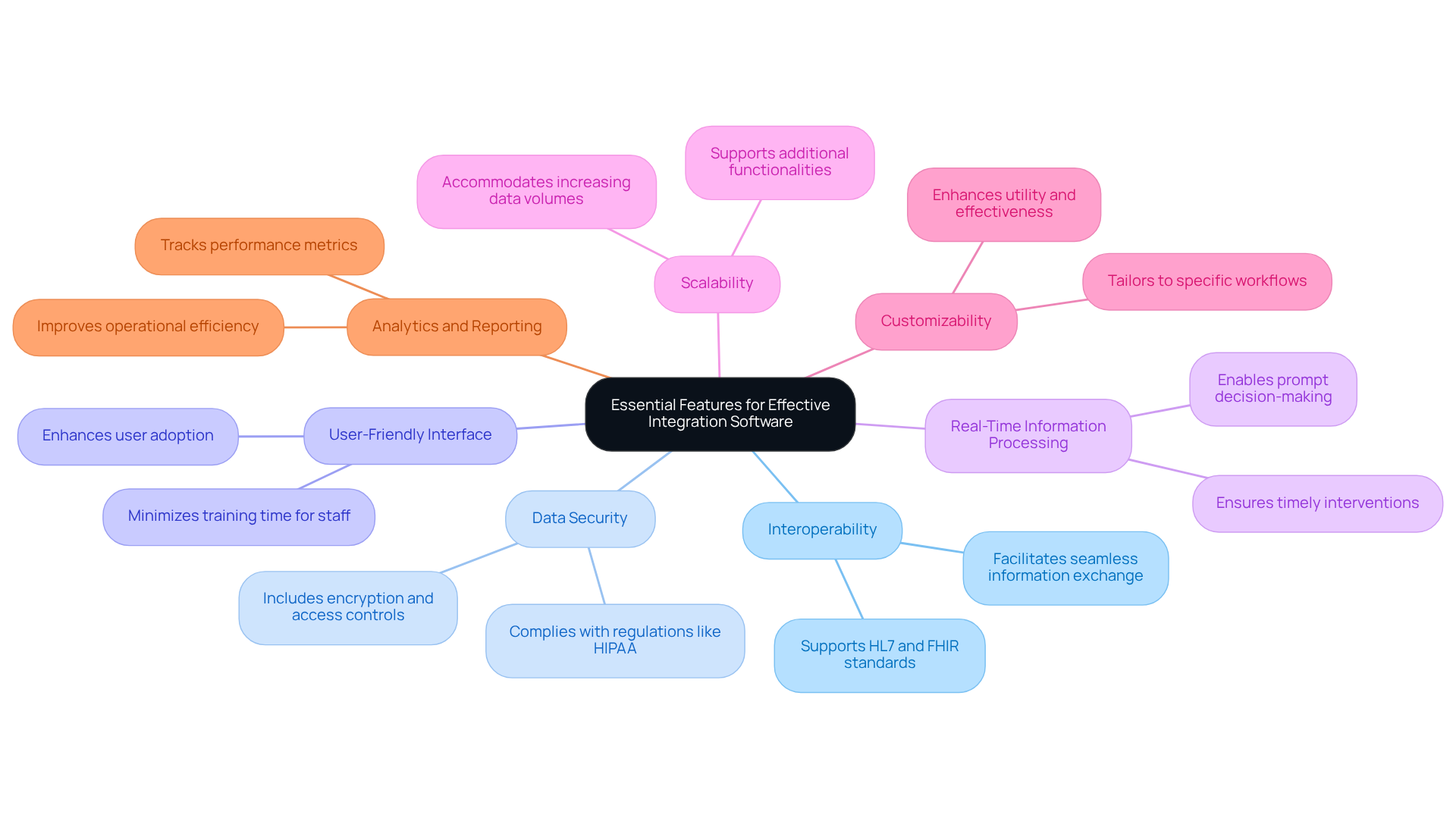
Organizations must prioritize several essential features when selecting healthcare integration software to ensure effectiveness. The following key features are critical:
- Interoperability: The capacity to interact with various systems and standards, such as HL7 and FHIR, is essential for seamless information exchange.
- Data Security: Robust security measures, including encryption and access controls, are necessary to protect sensitive patient information and comply with regulations like HIPAA.
- User-Friendly Interface: A straightforward interface enhances user adoption and minimizes training time for staff, facilitating smoother transitions.
- Real-Time Information Processing: The ability to process and share information instantly is crucial for prompt decision-making in patient care, ensuring timely interventions.
- Scalability: The software should be capable of growing with the organization, accommodating increasing data volumes and additional functionalities as needed.
- Customizability: Flexibility to tailor the software to specific organizational workflows and requirements can significantly enhance its utility and effectiveness.
- Analytics and Reporting: Built-in analytics tools enable organizations to track performance metrics and improve operational efficiency, driving better outcomes.
By concentrating on these attributes, medical organizations can ensure they select healthcare integration software that aligns with their operational needs and enhances patient care.
Implement Best Practices for Successful Integration
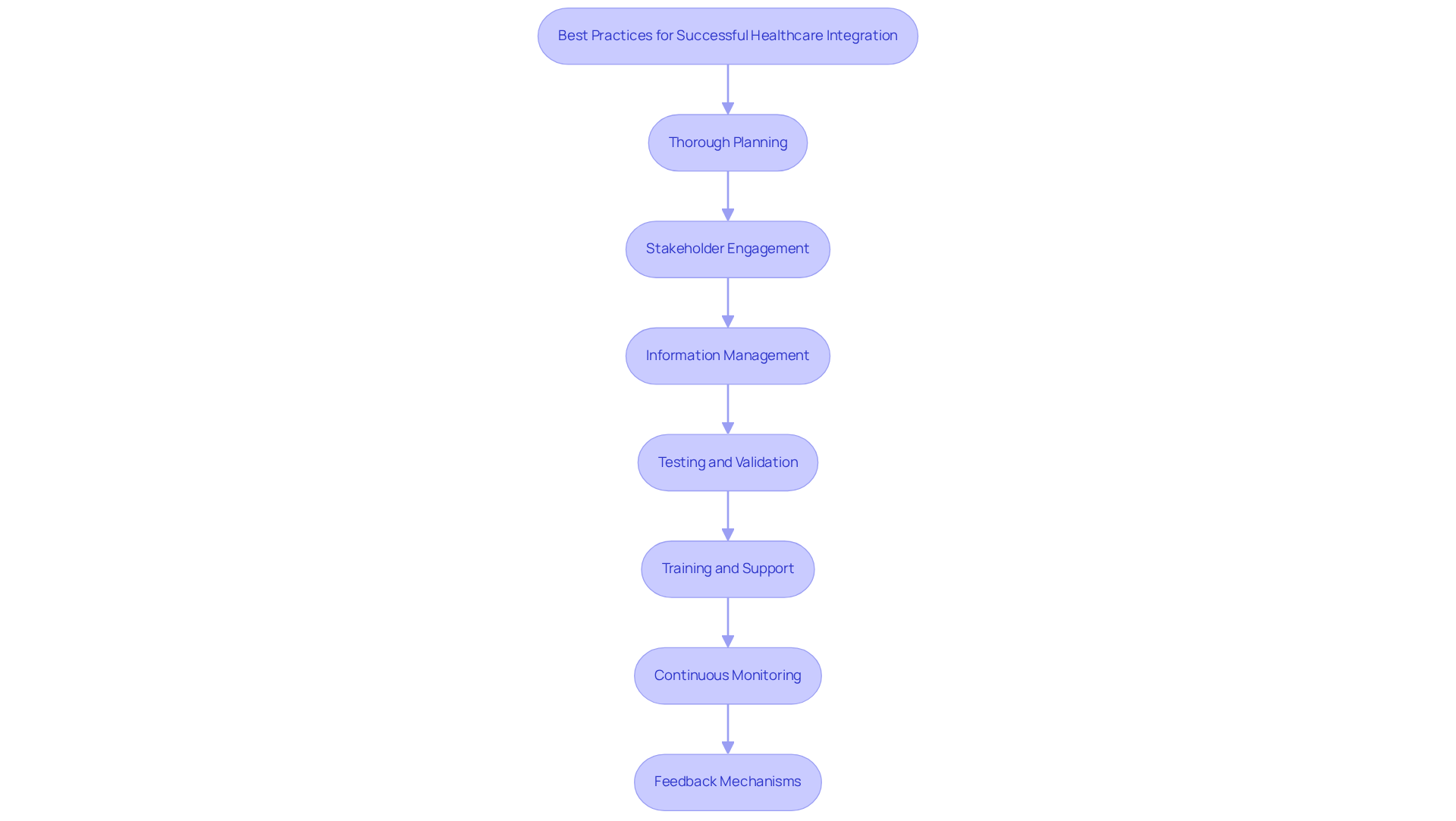
To achieve successful healthcare integration, organizations should implement several best practices:
- Thorough Planning: Begin with a comprehensive evaluation of existing systems and workflows to identify connection needs and objectives. This planning phase is essential for aligning coordination efforts with the overarching goals of the organization.
- Stakeholder Engagement: Engage key stakeholders, including clinical staff and IT personnel, throughout the implementation process. Their involvement ensures that the software effectively meets user needs and expectations.
- Information Management: Establish clear information governance policies to oversee the quality, security, and compliance of information during the unification process. This governance is critical for maintaining integrity and trust in the system.
- Testing and Validation: Conduct thorough testing of the integration software to identify and rectify issues prior to full deployment. This process includes validating data accuracy and assessing the platform’s performance.
- Training and Support: Offer comprehensive training for users to ensure familiarity with the new platform. Ongoing support is also vital to address any challenges that may arise after implementation.
- Continuous Monitoring: Utilize monitoring tools to track system performance and user engagement, enabling timely adjustments and enhancements as needed.
- Feedback Mechanisms: Create channels for users to provide feedback on the integration process and software functionality, fostering an environment of continuous improvement.
By adhering to these best practices, healthcare organizations can enhance their collaborative efforts with healthcare integration software, leading to improved operational efficiency and better patient support.
Address Challenges in Implementing Integration Software
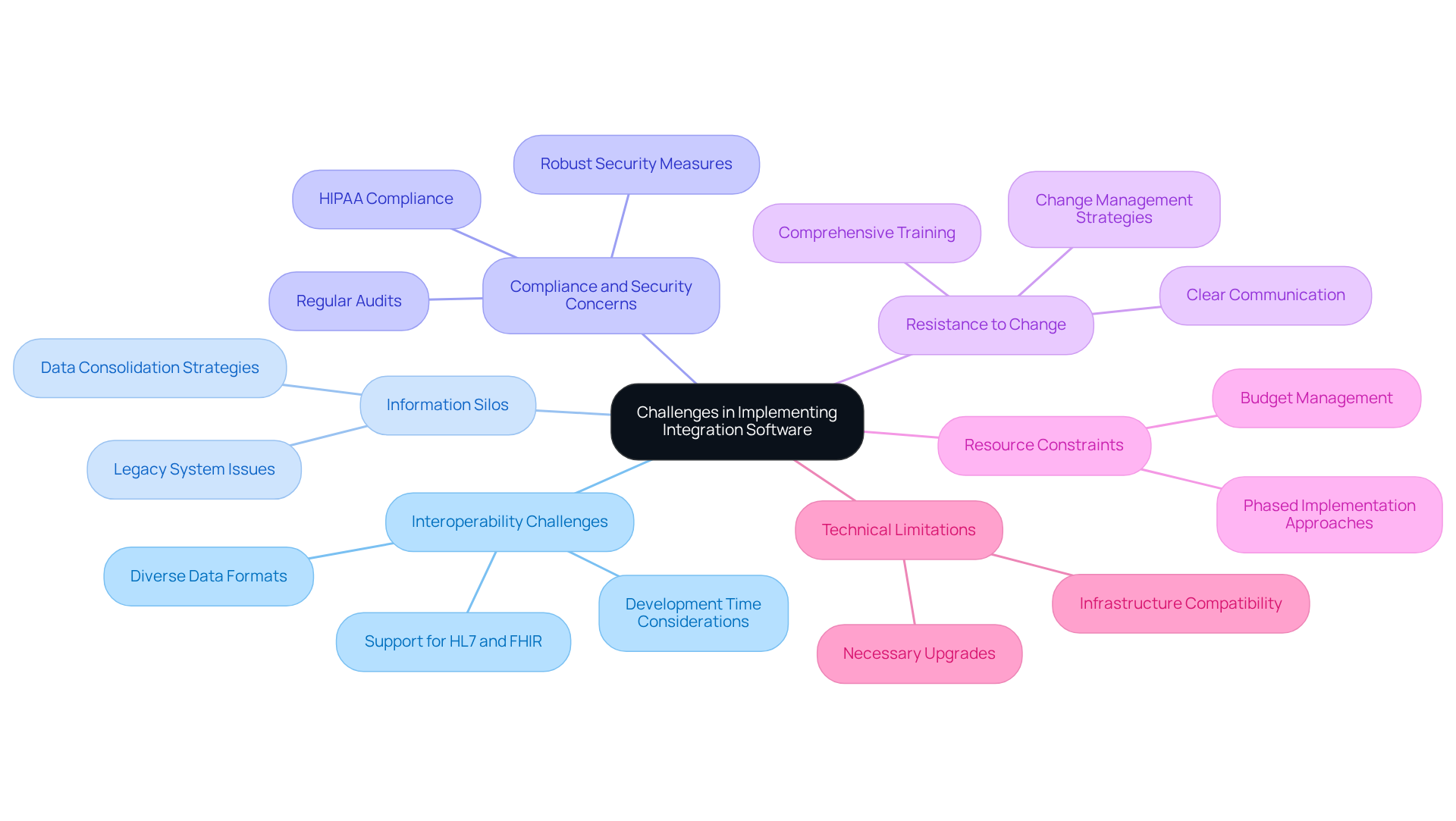
Implementing healthcare integration software presents several challenges that organizations must navigate to ensure success. Key challenges include:
- Interoperability Challenges: Various platforms often employ diverse data formats and standards, which can hinder smooth unification. Organizations should prioritize software that supports widely accepted standards such as HL7 and FHIR to facilitate effective communication between networks. It is important to note that “a basic read-only FHIR integration might take four to eight weeks of development,” a consideration organizations should factor into their integration planning.
- Information Silos: Legacy systems can create information silos that obstruct knowledge sharing. To address this issue, organizations should develop strategies to consolidate data, ensuring accessibility across all platforms, which in turn enhances operational efficiency.
- Compliance and Security Concerns: Navigating compliance with regulations like HIPAA can be complex. Organizations must implement robust security measures and conduct regular audits to maintain compliance, as security reviews and BAA negotiations typically account for a significant portion of the time involved in EHR incorporation.
- Resistance to Change: Staff may resist adopting new systems due to unfamiliarity or perceived complexity. Effective change management strategies, including comprehensive training and clear communication, are essential to facilitate user acceptance and minimize disruptions during the transition. As Michael Nikitin emphasizes, “a structured FHIR connection roadmap from MVP to market prevents the most costly early errors.”
- Resource Constraints: Limited budgets and personnel can impede unification efforts. Organizations should consider phased implementation approaches to distribute costs and resource demands over time, allowing for a more manageable transition. Integration projects can sometimes take longer or incur higher costs than anticipated, with minor delays impacting operations, particularly in smaller clinics.
- Technical Limitations: Existing infrastructure may not support new unification solutions. Organizations ought to evaluate their current technology environment and invest in necessary upgrades or replacements to ensure compatibility with contemporary connection tools.
By recognizing and addressing these challenges, healthcare organizations can significantly enhance their chances of successful integration using healthcare integration software, ultimately leading to improved patient care and operational efficiency.
Conclusion
In conclusion, the implementation of healthcare integration software represents not merely a technical task but a strategic initiative that can profoundly enhance patient care and operational efficiency. By adopting the best practices outlined and proactively addressing potential challenges, healthcare organizations can position themselves to excel in an increasingly interconnected medical landscape. Investing in robust integration solutions today will lay the groundwork for a more efficient and patient-centered healthcare system in the future.
Frequently Asked Questions
What is healthcare integration software?
Healthcare integration software includes platforms and applications designed to connect various medical IT solutions, facilitating seamless data exchange and communication across diverse networks.
Why is healthcare integration software important?
It is crucial for enhancing care coordination, improving patient outcomes, and ensuring compliance with regulatory standards by promoting interoperability and enabling efficient sharing of patient information among different medical tools.
How does healthcare integration software improve patient care?
It streamlines workflows, minimizes the risk of errors, enhances accuracy, and reduces the time medical providers spend on administrative tasks, allowing them to focus more on patient engagement and support.
What is the current market trend for medical data unification?
The medical data unification market was valued at USD 1.05 billion in 2022 and is projected to grow to USD 1.21 billion in 2023, reaching USD 3.11 billion by 2030, with a compound annual growth rate (CAGR) of 14.5% from 2023 to 2030.
What role does North America play in the healthcare integration software market?
North America accounted for over 38% of the global revenue in the healthcare integration software market in 2022.
What recent advancements are impacting healthcare integration software?
Advancements such as the adoption of FHIR APIs and event-driven architectures are revolutionizing medical organizations’ operations by facilitating immediate responses to clinical events.
What sectors are most involved in the healthcare integration software market?
The hospital sector represented more than 51% of the medical information unification market in 2022, while the tools sector dominated with over 69% share of global revenue in the same year.
List of Sources
- Define Healthcare Integration Software and Its Importance
- EHR Integration And Healthcare Innovation (https://forbes.com/councils/forbestechcouncil/2026/04/01/ehr-integration-and-healthcare-innovation-opportunities-and-considerations)
- Healthcare Interoperability – 2026 Health IT Predictions | Healthcare IT Today (https://healthcareittoday.com/2026/01/08/healthcare-interoperability-2026-health-it-predictions)
- Healthcare Data Integration Market Size, Share Report, 2030 (https://grandviewresearch.com/industry-analysis/healthcare-data-integration-market-report)
- Future of Healthcare Integration Technology in 2026 (https://emorphis.health/blogs/future-of-healthcare-integration-technology)
- Healthcare CIOs see AI integration as a competitive necessity (https://healthcareitnews.com/news/healthcare-cios-see-ai-integration-competitive-necessity)
- Identify Essential Features for Effective Integration Software
- Future of Healthcare Integration Technology in 2026 (https://emorphis.health/blogs/future-of-healthcare-integration-technology)
- The Integration Imperative: Key Takeaways from HIMSS 2026 (https://mitel.com/blog/the-integration-imperative-key-takeaways-from-himss-2026)
- EHR Integration And Healthcare Innovation (https://forbes.com/councils/forbestechcouncil/2026/04/01/ehr-integration-and-healthcare-innovation-opportunities-and-considerations)
- Top Features Every Modern Healthcare App Must Have in 2026 | AWS Builder Center (https://builder.aws.com/content/39nV5yjioYwgFwdHIrfDApBoNAi/top-features-every-modern-healthcare-app-must-have-in-2026)
- 20 Future EHR Trends Transforming Healthcare (https://paceplus.com/ehr-trends)
- Implement Best Practices for Successful Integration
- Healthcare Compliance in 2026: New Standards Every Medical Facility Must Know (https://aurorafinancials.com/healthcare-compliance-in-2026-new-standards-every-medical-facility-must-know)
- 21st Century Cures Act EHR Requirements: 2026 Integration Guide (https://anisolutions.com/2026/04/02/how-the-21st-century-cures-act-changes-your-ehr-integration-requirements)
- Mirth Connect Use Cases 2026: Healthcare Integration for Organizations, Vendors & Startups (https://kpitechservices.com/blogs/mirth-integration-use-cases-in-healthcare)
- Six Trends Shaping Connected Care in 2026 ⋆ LANES (https://lanesla.org/six-trends-shaping-connected-care-in-2026)
- 5 Developments Digital Health Innovators Should Watch in 2026 (https://covingtondigitalhealth.com/2026/01/5-developments-digital-health-innovators-should-watch-in-2026)
- Address Challenges in Implementing Integration Software
- 7 EHR Integration Challenges In 2026 (+ Solutions) (https://murphi.ai/ehr-integration-challenges)
- Interoperability woes still plague healthcare in 2026. Here’s what to do about it. | TechTarget (https://techtarget.com/searchhealthit/feature/Interoperability-woes-still-plague-healthcare-in-2026-Heres-what-to-do-about-it)
- EHR Integration Challenges in 2026: What Healthcare Startups and RCM Teams Are Still Getting Wrong | Blog | Itirra (https://itirra.com/blog/ehr-integration-challenges-in-2026-what-healthcare-startups-and-rcm-teams-are-still-getting-wrong)
- Healthcare Software Development Challenges in 2026 (https://techexactly.com/blogs/healthcare-software-development-challenges-2026)
- Interoperability 2026: Are We FHIRed Up Yet? (https://abouthealthcare.com/industry-news/interoperability-2026-are-we-fhired-up-yet)
