Introduction
Medical coding systems are essential in the healthcare industry, converting intricate medical information into standardized codes that facilitate accurate billing, compliance, and reimbursement. As the demand for precision in healthcare documentation increases, it is crucial for providers to understand the features, benefits, and costs associated with various coding systems to optimize their operations.
With multiple frameworks available, such as ICD-10, CPT, and HCPCS, healthcare professionals face the challenge of navigating the complexities of selecting the appropriate software that aligns with their unique needs while balancing cost and functionality.
Overview of Medical Coding Systems
serve as essential structures that translate medical diagnoses, procedures, services, and equipment into standardized alphanumeric codes. The primary frameworks in use include:
- ICD-10 (International Classification of Diseases)
- CPT (Current Procedural Terminology)
- HCPCS (Healthcare Common Procedure Coding System)
Each framework has a distinct role: ICD-10 codes are primarily utilized for diagnosing conditions, CPT codes document medical procedures, and HCPCS codes encompass services and equipment.
The significance of these frameworks is paramount, as they are integral to the invoicing, compliance, and billing processes within the medical field. Hospitals, for instance, rely heavily on coding systems to ensure accurate billing, which is crucial for securing appropriate reimbursements from insurance providers. Notably, over 90% of healthcare providers have adopted ICD-10 classification to meet regulatory requirements and enhance billing accuracy.
Healthcare professionals stress that proper documentation is vital for compliance and financial stability. As one expert noted, “Precise documentation reduces denied claims and speeds up reimbursement, which is essential for sustaining cash flow in medical practices.” Furthermore, revisions to these classification frameworks, such as the transition from ICD-9 to ICD-10, have introduced enhanced precision, facilitating better monitoring of public health trends and more efficient management of medical resources.
The integration of software into medical operations not only streamlines processes but also supports adherence to evolving regulations. As the healthcare landscape continues to change, the reliance on ICD-10, CPT, and HCPCS classifications is expected to grow, making it imperative for providers to stay informed about updates and best practices. Additionally, the healthcare classification market was valued at USD 14.4 billion in 2023 and is projected to expand at a CAGR of 10.1% from 2024 to 2032, underscoring the increasing importance of these frameworks in the sector.
Key Features of Leading Medical Coding Systems
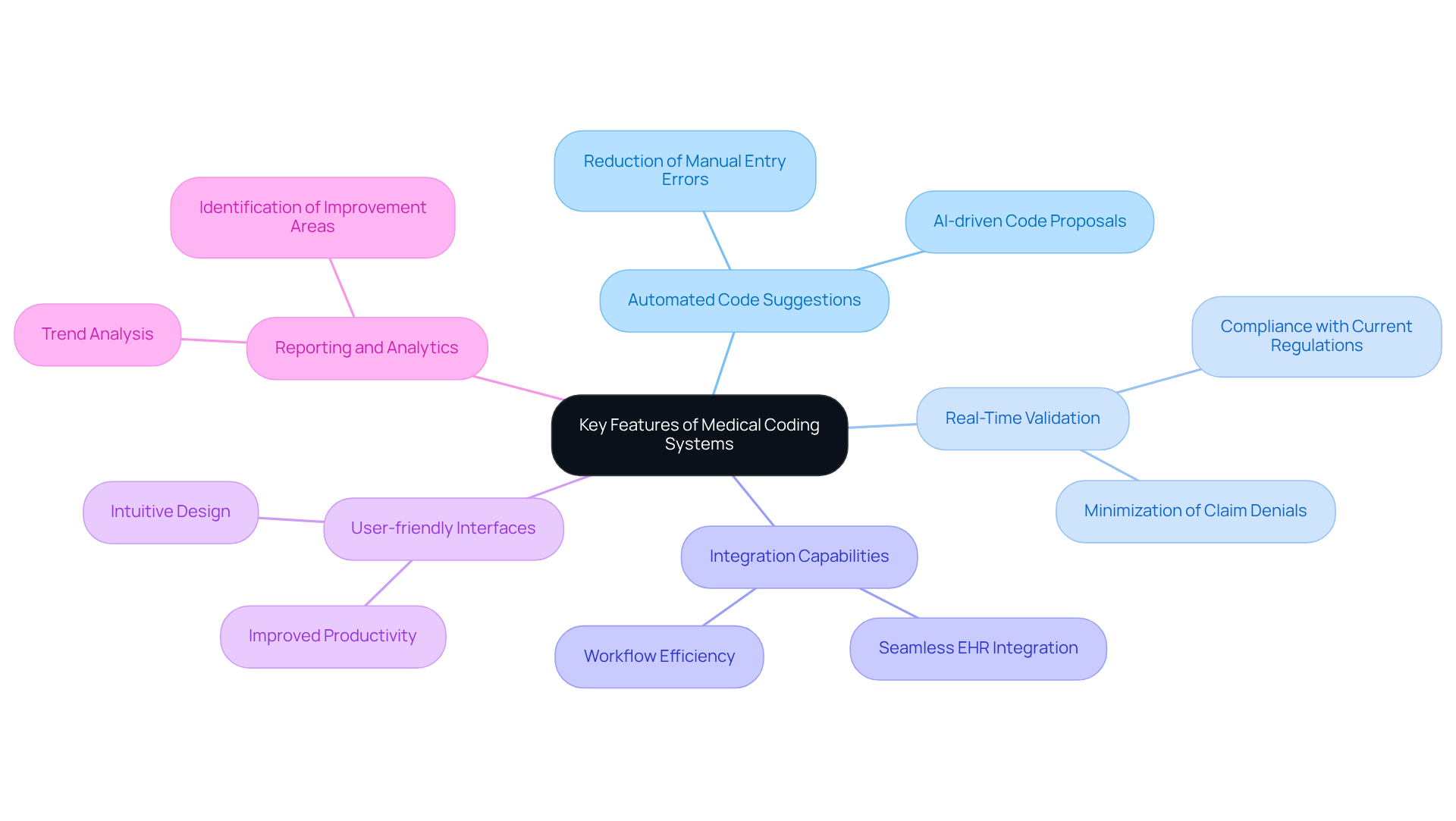
The variety of features offered by leading medical coding systems is designed to streamline coding processes and enhance accuracy. These frameworks incorporate several key functionalities:
- Artificial intelligence: Many systems leverage artificial intelligence to propose codes based on clinical documentation, which significantly reduces manual entry errors.
- Compliance monitoring: The compliance monitoring feature ensures that codes adhere to current regulations and minimizes the risk of claim denials.
- Integration capabilities: The ability of systems to seamlessly integrate with Electronic Health Records (EHR) and billing platforms is essential for maintaining workflow efficiency.
- User-friendly interfaces: User-friendly interfaces provide intuitive designs that facilitate easy navigation for coders, ultimately improving productivity.
- Reporting tools: Advanced reporting tools in medical coding systems empower medical providers to analyze trends and identify areas for improvement.
Benefits of Each Medical Coding System
Each presents distinct advantages that significantly enhance medical billing processes:
- ICD-10: This system improves patient care by providing detailed coding for diseases and conditions. Its implementation has been shown to reduce claim denials, leading to more efficient payment processes.
- CPT: The CPT system is essential for accurate invoicing of medical procedures. It ensures that medical providers receive precise reimbursement for their services. Practices utilizing CPT coding have reported a decrease in billing errors, with studies indicating that accurate coding can result in a 30% reduction in labor costs associated with invoicing. This efficiency is crucial as the medical landscape evolves, particularly with the anticipated introduction of new technologies. As Jasmine Oliver notes, “AI in healthcare is present, and 2026 signifies the year when it becomes obligatory for most providers.”
- HCPCS: The HCPCS provides a comprehensive framework for classifying non-physician services and equipment, which is vital for invoicing in a diverse healthcare environment. This framework enhances the CPT by encompassing a broader range of services, ensuring that all aspects of patient care are accounted for in invoicing.
- AI Technologies: These innovative tools significantly improve coding speed and accuracy while reducing administrative burdens. By automating routine tasks, AI-enhanced technologies allow invoicing teams to focus on more complex issues, ultimately improving compliance with evolving regulations. As healthcare providers prepare for the mandatory integration of AI in medical billing by 2026, the advantages of these technologies become increasingly apparent. Experts suggest that successful AI implementations depend more on efficient processes and staff training than on the technology itself. Additionally, it is noteworthy that 61% of physicians express concern that payer AI is increasing denial rates, underscoring the challenges associated with these advancements. Furthermore, the deadline for public reporting of approval/denial rates is March 31, 2026, highlighting the urgency for practices to adapt.
Cost Analysis of Medical Coding Systems
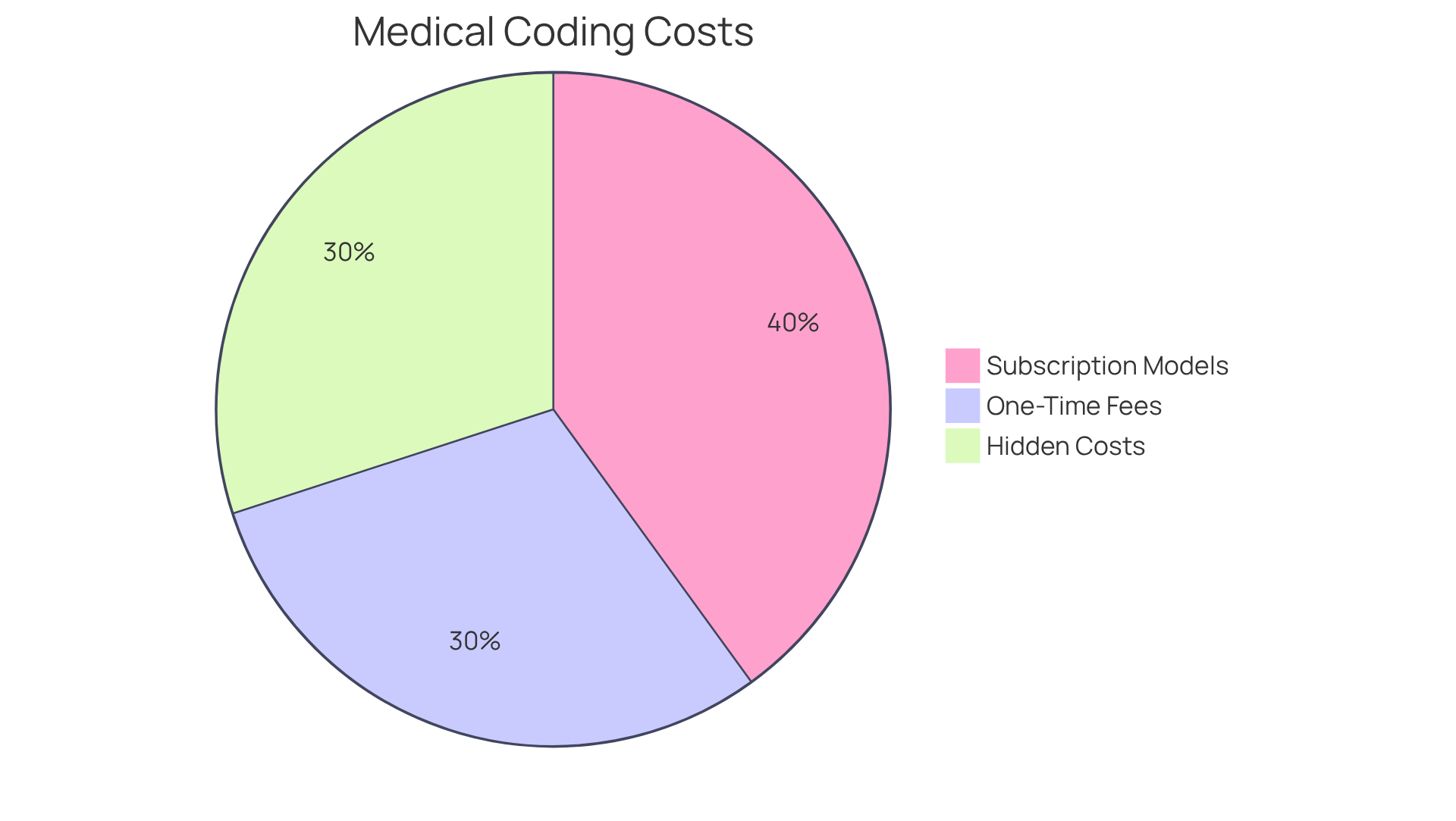
The costs can vary significantly based on features, deployment models, and provider size. Understanding these variations is crucial for making informed decisions.
Subscription Models typically range from $50 to $600+ per provider per month. This pricing depends on the provider type, reflecting the diverse needs of different organizations.
One-time fees may also apply, with some systems requiring a one-time purchase fee that can range from $1,000 to $10,000. This cost is influenced by the complexity of the software, which can vary widely among different solutions.
Additionally, providers should be aware of additional costs that may arise. These can include setup fees, training expenses, and ongoing support costs. A thorough analysis of these factors is essential for making a budget.
Conclusion
The exploration of medical coding systems software underscores their essential role in enhancing healthcare operations through improved accuracy, compliance, and efficiency. By comprehensively understanding the distinct functions of ICD-10, CPT, and HCPCS, healthcare providers can make informed decisions that align with their operational needs and regulatory requirements.
Key insights from the article highlight the necessity of adopting the appropriate coding system tailored to specific healthcare practices. Features such as automated code suggestions, real-time validation, and seamless integration with existing systems not only streamline billing processes but also mitigate the potential for claim denials. Moreover, the anticipated integration of AI in medical coding by 2026 presents both opportunities and challenges that healthcare providers must navigate with care.
As the landscape of medical coding continues to evolve, it is crucial to stay informed about the latest features, benefits, and costs associated with these systems to maintain a competitive edge. Embracing these advancements enhances operational efficiency and ensures that healthcare providers can deliver high-quality care while optimizing their financial performance. The future of medical coding systems is promising, and proactive engagement with these tools will be vital for success in the healthcare industry.
Frequently Asked Questions
What are medical coding systems?
Medical coding systems are frameworks that translate healthcare diagnoses, procedures, services, and equipment into standardized alphanumeric codes.
What are the primary medical coding frameworks?
The primary medical coding frameworks are ICD-10 (International Classification of Diseases), CPT (Current Procedural Terminology), and HCPCS (Healthcare Common Procedure Coding System).
What is the role of ICD-10 codes?
ICD-10 codes are primarily used for diagnosing medical conditions.
What do CPT codes document?
CPT codes document medical procedures performed by healthcare providers.
What do HCPCS codes encompass?
HCPCS codes encompass services and equipment used in healthcare.
Why are medical coding systems significant?
They are crucial for invoicing, compliance, and reimbursement processes within the medical field, helping ensure accurate documentation and appropriate reimbursements from insurance providers.
How has the adoption of ICD-10 affected healthcare providers?
Over 90% of healthcare providers have adopted ICD-10 to meet regulatory requirements and enhance billing accuracy.
What is the impact of proper documentation in medical coding?
Proper documentation is vital for compliance and financial stability, as it reduces denied claims and speeds up reimbursement processes.
What improvements came with the transition from ICD-9 to ICD-10?
The transition introduced enhanced precision in coding, facilitating better monitoring of public health trends and more efficient management of medical resources.
How does medical coding software benefit healthcare operations?
Medical coding software streamlines billing procedures and supports adherence to evolving regulations.
What is the projected growth of the healthcare classification market?
The healthcare classification market was valued at USD 14.4 billion in 2023 and is projected to expand at a CAGR of 10.1% from 2024 to 2032.
List of Sources
- Overview of Medical Coding Systems
- Medical Coding Market Size & Share – Trends Report, 2032 (https://gminsights.com/industry-analysis/medical-coding-market)
- CoxHealth Case Study | Infusion Billing Automation (https://medaptus.com/coxhealth-charge-pro-case-study)
- A Simple Guide to CPT, HCPCS, and ICD Codes for Healthcare Providers (https://infohubconsultancy.com/blog/a-simple-guide-to-cpt-hcpcs-and-icd-codes-for-healthcare-providers)
- AI Medical Coding Case Studies | PCG Software (https://pcgsoftware.com/efficiency.profitability.case.studies.pcg)
- The 4 Medical Coding Systems & What They Represent (https://globalhealthcareresource.com/blog/understanding-medical-coding-systems)
- Key Features of Leading Medical Coding Systems
- Top 10 Automated Medical Coding Software for 2026 (https://aptarro.com/insights/top-automated-medical-coding-software)
- Emerging Medical Coding Trends | Insights by ScribeMedics. (https://scribemedics.org/medical-coding-trends)
- How AI and Automation Are Changing Medical Coding Accuracy (https://statmedical.net/how-ai-and-automation-are-changing-medical-coding-accuracy)
- How AI is Revolutionizing Medical Billing and Coding (https://utsa.edu/pace/news/ai-in-medical-billing-and-coding.html)
- Medical Coding Software: Key Features, Benefits, and Trends to Watch – Matellio (https://matellio.com/blog/medical-coding-software-development)
- Benefits of Each Medical Coding System
- 8 Key Benefits of ICD-10 Implementation – Flatworld Solutions (https://flatworldsolutions.com/healthcare/articles/icd-10-implementation-benefits.php)
- CPT Coding: New AI-Augmented Medical Billing Can Benefit Your Practice (https://unislink.com/rcm-best-practices-blog/the-amas-2026-cpt-updates-what-physician-groups-need-to-know-about-ai-augmented-codes)
- Everything About AI in Medical Billing for 2026 AI in Medical Billing for 2026 | Key Trends, Laws, & Solutions (https://medcaremso.com/blog/everything-about-ai-in-medical-billing)
- AI and Beyond: What’s Ahead for Healthcare RCM in 2026 (https://blog.quadax.com/ai-and-beyond-whats-ahead-for-healthcare-rcm-in-2026)
- Cost Analysis of Medical Coding Systems
- Medical billing software cost: A complete pricing guide (2026) (https://tebra.com/theintake/getting-paid/how-much-does-medical-billing-software-cost)
- The Hidden Costs of Manual Medical Coding and How AI Saves Money (https://blog.nym.health/hidden-costs-of-manual-medical-coding-how-ai-saves-money)
