5 Best Practices for Custom Healthcare Software Development Solutions

Introduction
The healthcare landscape is undergoing rapid evolution, propelled by technological advancements and increasing regulatory demands. As organizations endeavor to create tailored healthcare software solutions, grasping the best practices in this domain is essential. This article explores critical strategies that not only ensure compliance with regulations such as HIPAA and FDA guidelines but also bolster the effectiveness and security of healthcare applications.
How can developers adeptly navigate these complexities while delivering innovative solutions that cater to the needs of both providers and patients?
Understand Regulatory Requirements
In healthcare application development, a comprehensive understanding of regulatory requirements is essential. Regulations such as HIPAA (Health Insurance Portability and Accountability Act) impose stringent protocols for handling, storing, and transmitting patient information. Developers must be well-versed in these regulations to ensure compliance and mitigate legal risks. Furthermore, the FDA has established specific guidelines for software that qualifies as a medical device, which can include applications that manage patient data or assist in diagnosis.
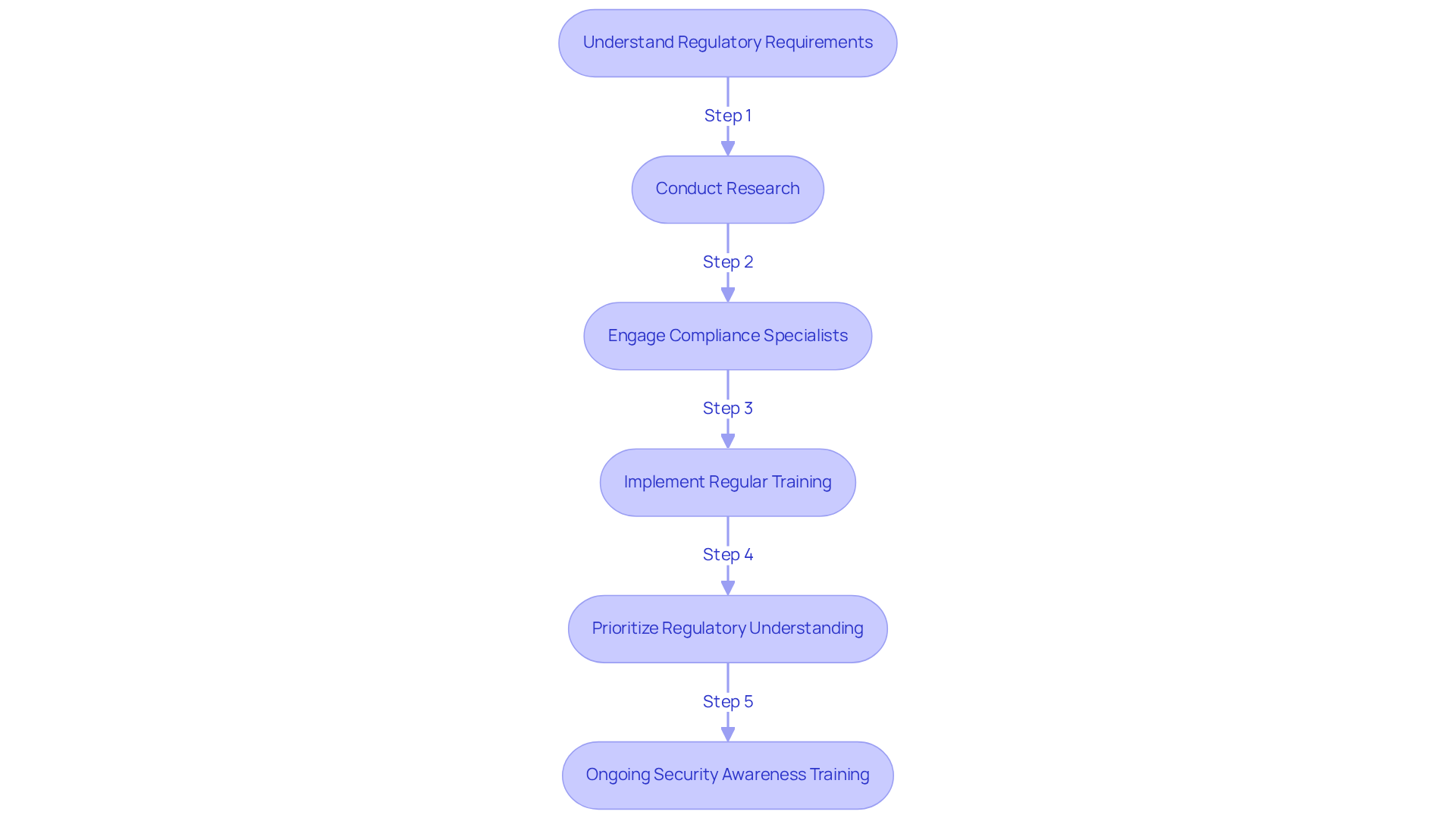
To effectively navigate these complex regulations, development teams should take several key steps:
- Conduct thorough research on applicable laws and guidelines, ensuring alignment with the latest updates.
- Engage compliance specialists early in the creation process to help identify potential pitfalls and streamline adherence to regulations.
- Implement regular training for development teams on compliance updates and best practices; statistics indicate that 62% of organizations report annual training on HIPAA compliance, with 50% testing employees on HIPAA training at least annually.
By prioritizing regulatory understanding, developers can create solutions that not only meet market demands but also uphold the highest standards of patient safety and data integrity. This proactive approach significantly improves the success rates of medical application projects, ensuring they navigate FDA guidelines effectively. Moreover, with the anticipated increase in HIPAA violation penalties in 2026, the urgency for compliance has never been greater. Ongoing security awareness training is also crucial to combat evolving cyber threats, ensuring that all team members are equipped to handle sensitive information responsibly.
Define Clear Objectives
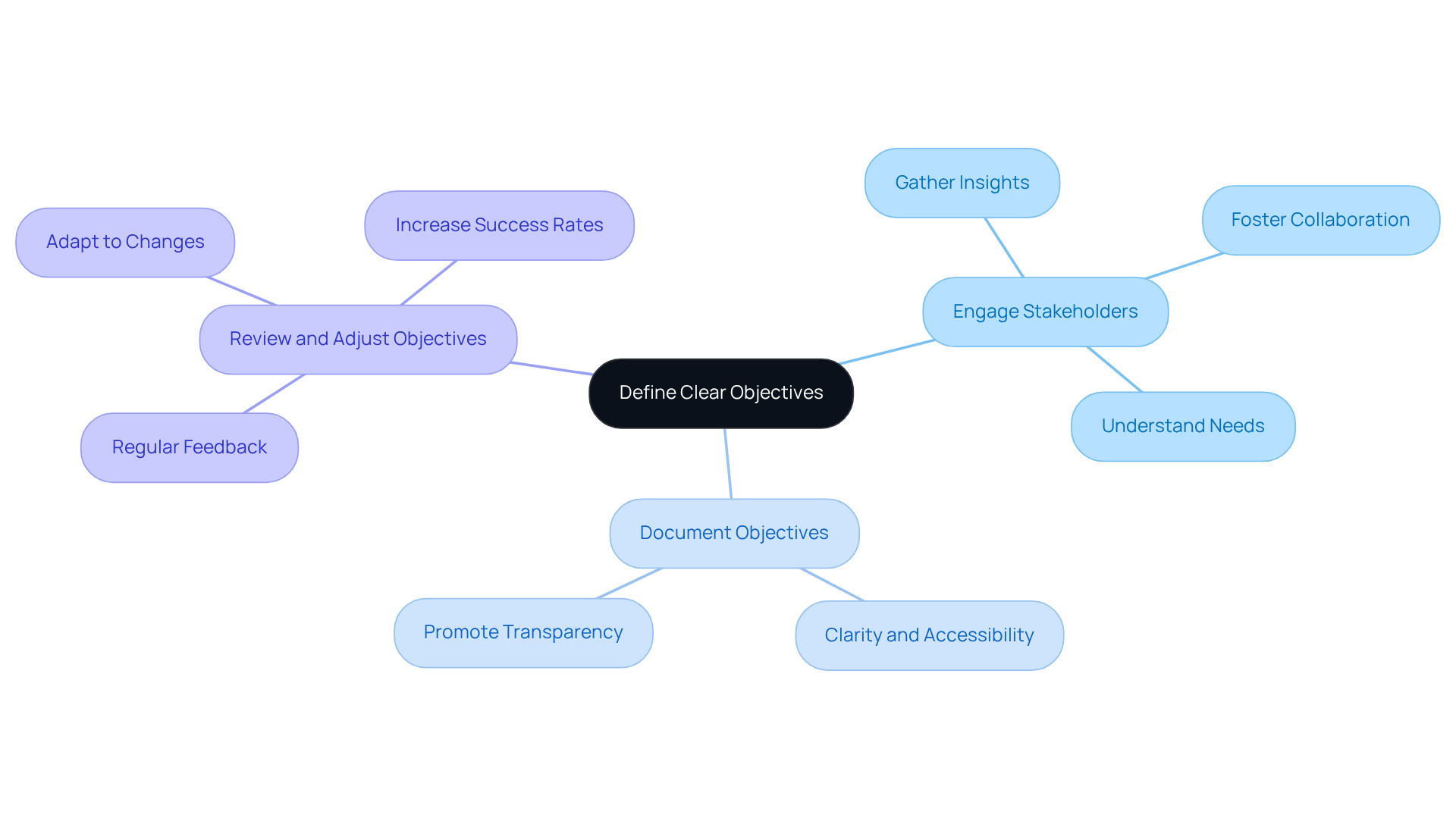
Establishing clear objectives is a crucial step in the creation process of medical applications. These objectives should adhere to the SMART criteria: specific, measurable, achievable, relevant, and time-bound. This clarity aids in aligning the team and stakeholders toward shared goals, thereby enhancing project success. To effectively define objectives, consider the following steps:
- Engage stakeholders to gather insights on their needs and expectations, fostering a collaborative environment. As Stephen Covey states, "Technology and tools are useful and powerful when they are your servant and not your master," which underscores the importance of understanding stakeholder needs.
- Document objectives clearly and concisely, ensuring that they are accessible to all team members. This promotes transparency and alignment within the team.
- Review and adjust objectives regularly based on stakeholder feedback and evolving requirements. Research indicates that companies that review goals more frequently are 31% more likely to achieve them than those that do not, highlighting the significance of regular reviews.
By setting clear goals, teams can strengthen focus, enhance communication, and ultimately provide solutions that effectively meet the needs of medical providers and patients alike. This method not only simplifies the creation process but also significantly increases the chances of project success, as evidenced by numerous successful medical applications that prioritize clear goals. For instance, the case study on the "Importance of Regular Goal Reviews" illustrates how frequent assessments can lead to improved performance and alignment with project objectives.
Choose the Right Development Partner
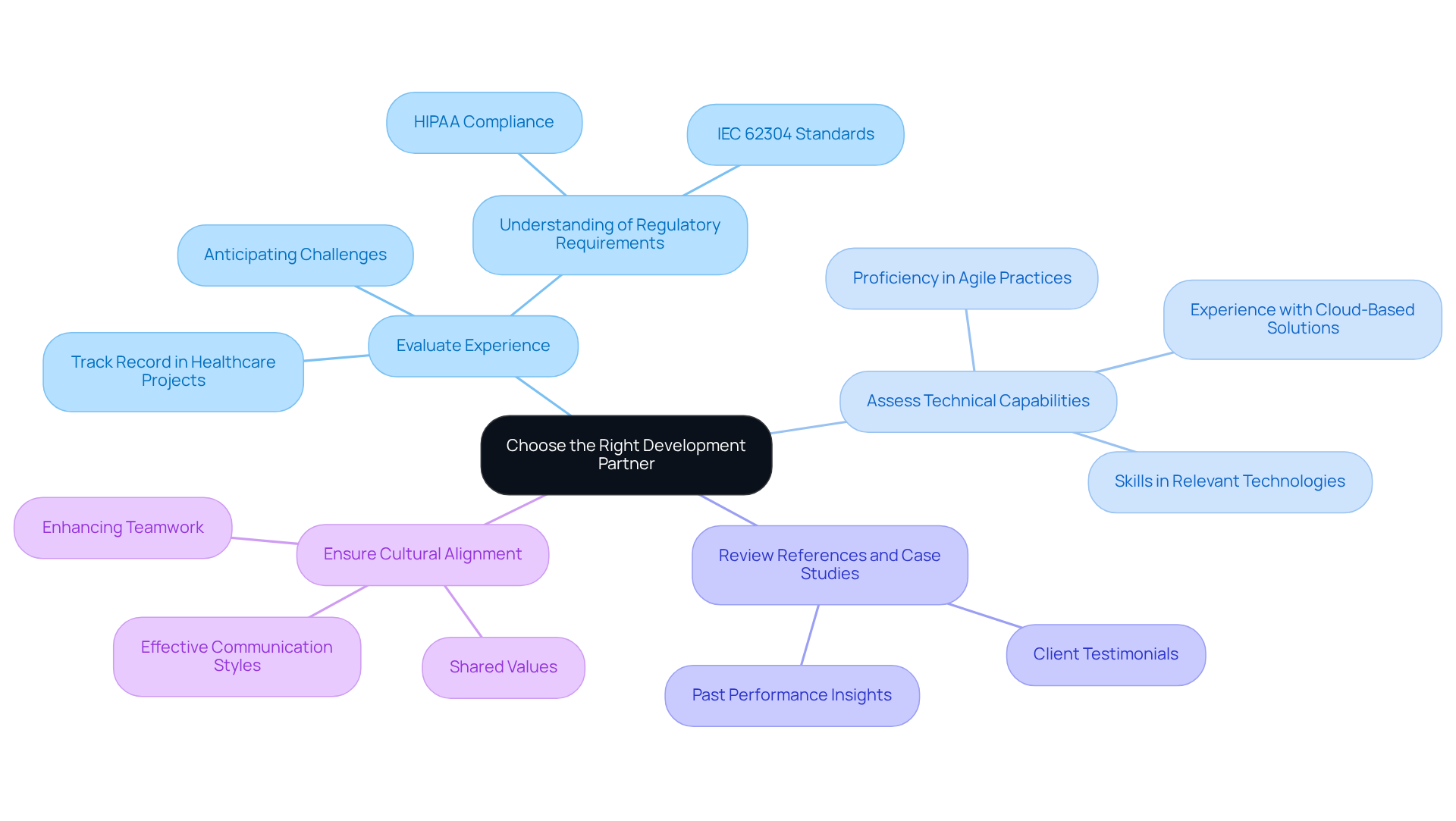
Choosing the right development partner is crucial in medical software development. An experienced collaborator can effectively manage the complexities of compliance and user needs. Here are key considerations for making an informed choice:
-
Evaluate Experience: Focus on the partner’s track record in healthcare projects, particularly their understanding of regulatory requirements such as HIPAA and IEC 62304 standards. A partner with a proven history in the medical field is better equipped to anticipate challenges and ensure compliance.
-
Assess Technical Capabilities: Ensure the partner possesses the necessary skills in relevant technologies and methodologies, such as Agile practices and cloud-based solutions. Their technical expertise should align with the specific needs of your project.
-
Review References and Case Studies: Investigate past performance through client testimonials and case studies. This examination provides insights into their ability to deliver successful outcomes and maintain client satisfaction.
-
Ensure Cultural Alignment: A strong cultural fit between your organization and the partner is vital for fostering effective collaboration. Shared values and communication styles can significantly enhance teamwork and project efficiency.
By carefully selecting a development partner, organizations can access specialized expertise, thereby increasing the likelihood of successful project outcomes in the dynamic medical field.
Ensure Seamless Integration with Existing Systems
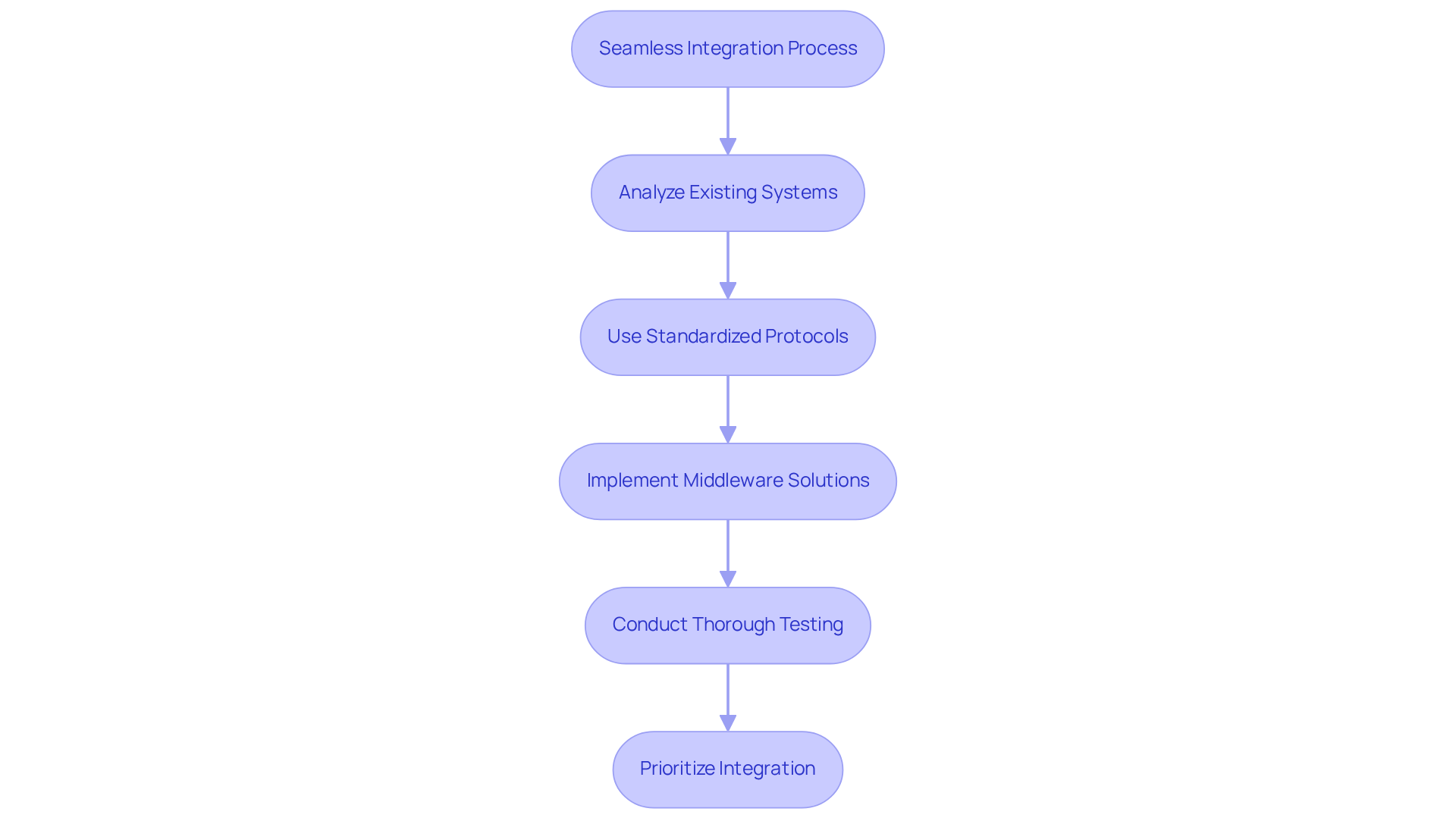
Smooth integration with existing systems is essential for the success of medical software solutions. Healthcare organizations typically utilize a variety of systems for patient management, billing, and electronic health records (EHR). To ensure effective integration, consider the following best practices:
-
Conduct a thorough analysis of existing systems to understand their architecture and data flow. This foundational step helps identify potential integration challenges and opportunities for optimization.
-
Employ standardized protocols such as HL7 or FHIR for information exchange. Over 90% of U.S. medical organizations currently utilize HL7 V2 standards, and the adoption rate of FHIR among medical institutions in the U.S. is 85%. These protocols significantly enhance interoperability, allowing for smoother data sharing across systems.
-
Implement middleware solutions to facilitate communication between disparate systems. This approach can streamline processes and reduce the complexity often associated with traditional integration methods.
-
Test integration thoroughly to identify and resolve any issues before full deployment. Rigorous testing ensures that systems work harmoniously, minimizing disruptions to patient care and operational workflows.
As noted by an IT expert, "Effective information exchange through HL7 leads to better medical decisions and improved patient outcomes." By prioritizing integration, medical applications can enhance operational efficiency and improve patient care results, ultimately leading to better service delivery in a rapidly evolving landscape. Furthermore, implementation times for claim processing services have been reduced by 75%, from 16 weeks to just 4 weeks, showcasing the tangible benefits of effective integration practices.
Prioritize Data Security and Privacy
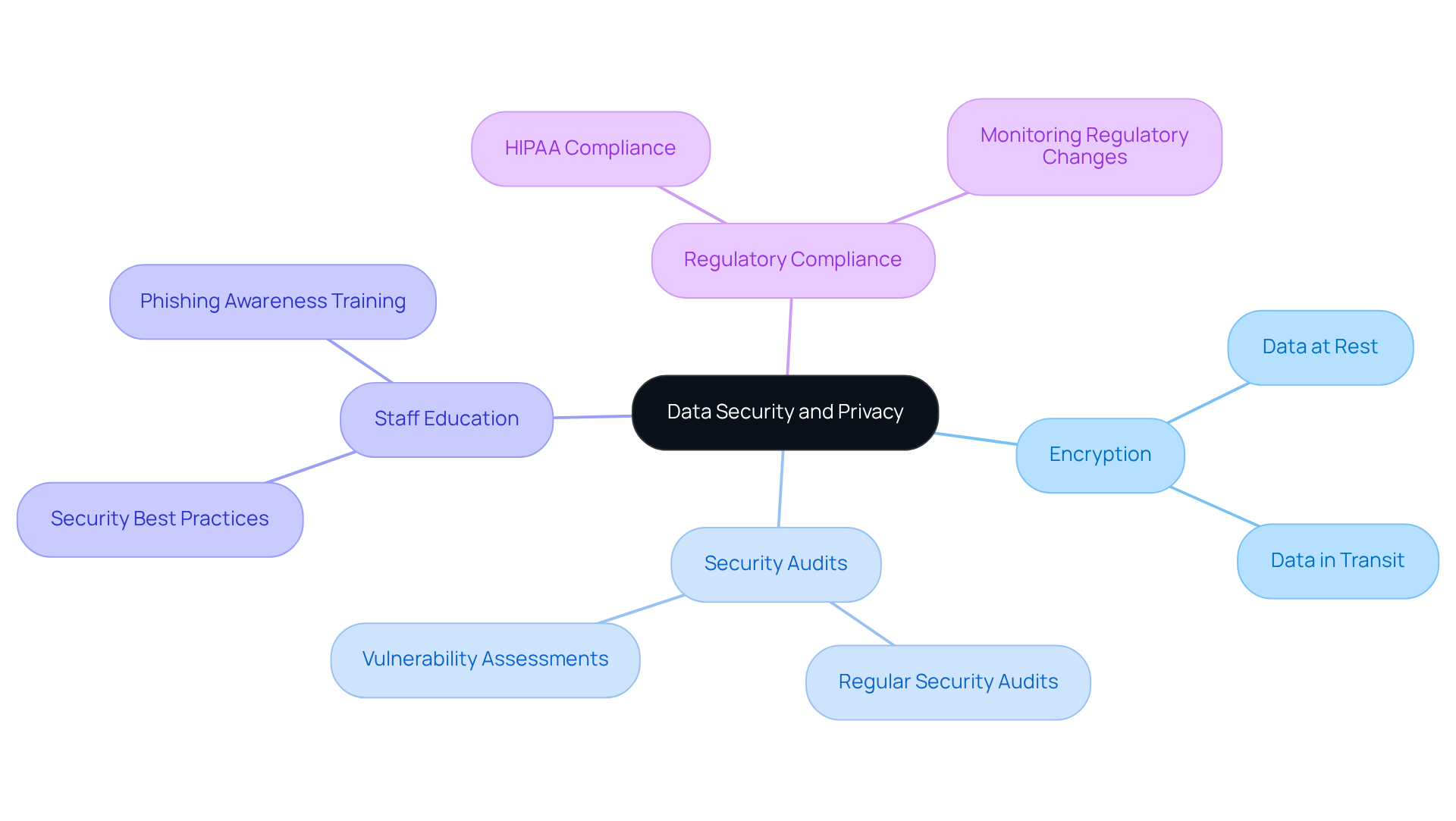
Focusing on information security and privacy is essential in custom healthcare software development solutions. As cyber threats increase and regulations become more stringent, developers must implement comprehensive security measures. Key strategies to enhance data security include:
- Implementing encryption for data at rest and in transit, which protects sensitive information from unauthorized access.
- Conducting regular security audits and vulnerability assessments to identify and address potential weaknesses.
- Educating staff on information security best practices to foster a culture of security awareness within the organization.
- Staying updated on regulatory changes to ensure ongoing compliance with laws such as HIPAA.
By prioritizing data security and privacy, healthcare software developers can create custom healthcare software development solutions that safeguard patient information and build trust with users.
Conclusion
In the field of custom healthcare software development, adhering to established practices is essential for crafting effective and compliant solutions. A strong emphasis on regulatory understanding, clear objectives, appropriate development partnerships, seamless integration, and robust data security ensures that healthcare applications not only fulfill the needs of providers and patients but also adeptly navigate the complexities of the industry.
This article underscores several key strategies, including the necessity of comprehending regulatory requirements such as HIPAA and FDA guidelines, the significance of setting SMART objectives, and the pivotal role of selecting an experienced development partner. Furthermore, ensuring smooth integration with existing systems and prioritizing data security are critical for enhancing operational efficiency and protecting patient information. Each of these practices contributes to a more successful development process, ultimately leading to improved healthcare outcomes.
As the landscape of healthcare software development continues to evolve, embracing these best practices will be vital for organizations aiming to excel in 2025 and beyond. By prioritizing compliance, clear communication, strategic partnerships, and data security, developers can create innovative solutions that not only address current challenges but also anticipate future needs within the healthcare sector. Taking proactive measures in these areas will safeguard patient information, foster trust, and enhance the overall quality of care delivered.