Digital Healthcare Software vs. Traditional Systems: Key Insights for Investors

Introduction
The healthcare landscape is experiencing a significant transformation as digital healthcare software emerges as a robust alternative to traditional systems. This shift not only promises enhanced operational efficiency and improved patient outcomes but also raises essential questions regarding data security and accessibility.
Investors in the healthcare sector must navigate the complexities of these evolving technologies, carefully weighing the distinct advantages of digital solutions against the enduring trust and familiarity provided by conventional practices.
How can stakeholders effectively evaluate the suitability of these systems to address the diverse needs of modern healthcare?
Define Digital Healthcare Software and Traditional Systems
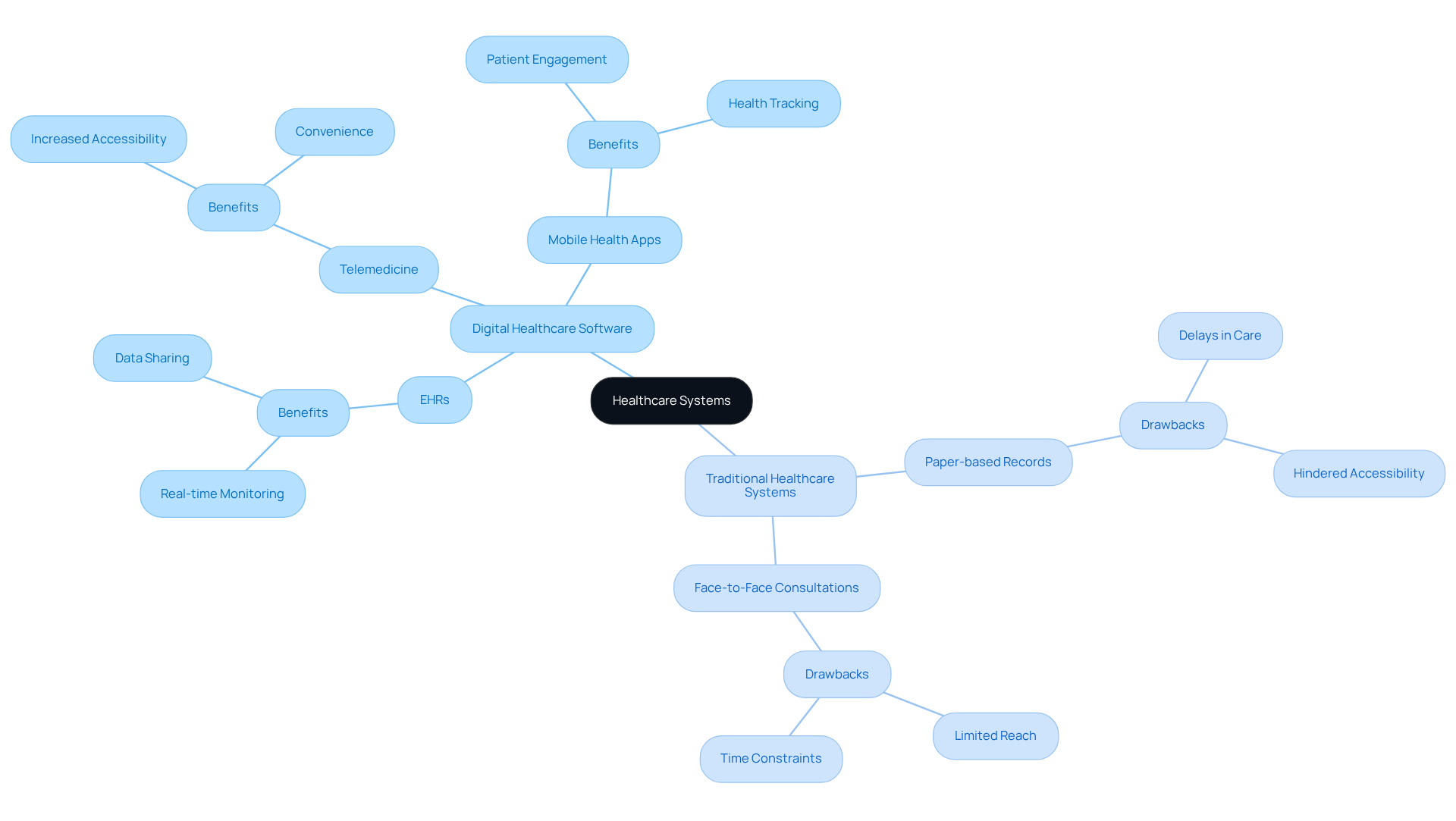
Digital healthcare software encompasses a variety of technologies designed to improve medical delivery through computing platforms, connectivity, and software solutions. This includes electronic health records (EHRs), telemedicine platforms, and mobile health applications that enable real-time monitoring and facilitate seamless data sharing.
In contrast, traditional healthcare frameworks often depend on paper-based records and face-to-face consultations, which can hinder accessibility and efficiency. These conventional systems are marked by organized procedures that frequently involve multiple intermediaries, resulting in delays in care and data access.
As of 2026, approximately 99% of hospitals offer electronic access to health records, reflecting a significant shift towards electronic solutions. Experts in medical technology emphasize that transitioning from traditional systems to digital healthcare software not only enhances operational efficiency but also improves user engagement and the quality of care.
The integration of digital tools is essential for modern medical practices, as it fosters more efficient workflows and better data management, ultimately leading to improved outcomes for patients.
Explore Advantages of Digital Healthcare Software
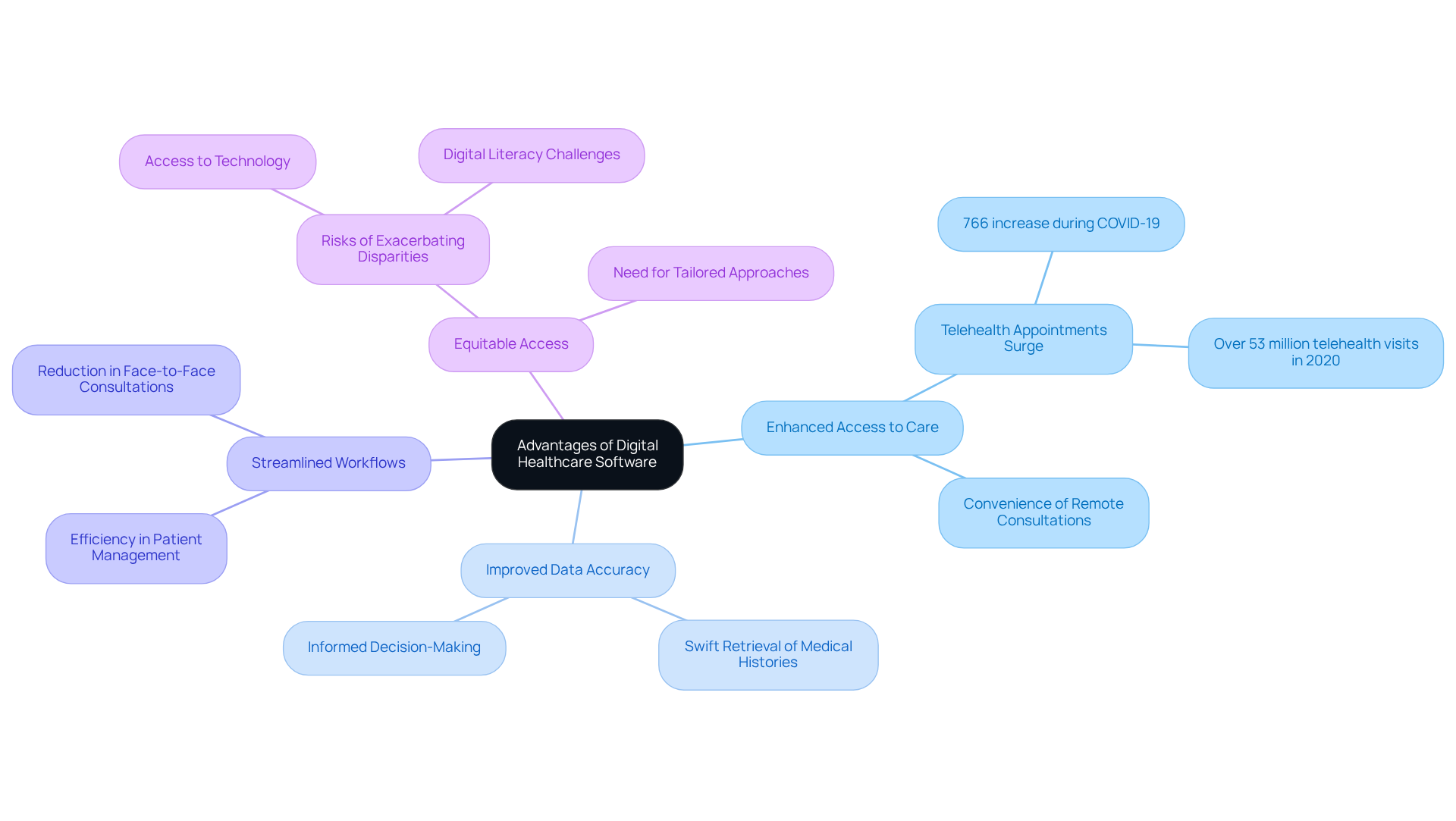
Digital healthcare software provides significant advantages, particularly in enhancing access to care, improving data accuracy, and streamlining workflows. Telemedicine platforms, as a form of digital healthcare software, exemplify this by enabling individuals to consult with healthcare professionals remotely, thereby reducing travel time and increasing convenience.
For instance, telehealth appointments surged by 766% during the first three months of the COVID-19 pandemic, underscoring its critical role in maintaining medical access. Furthermore, digital healthcare software enhances data management, enabling healthcare providers to swiftly retrieve medical histories and make informed decisions.
The integration of digital healthcare software with AI and machine learning fosters predictive analytics, enabling the early identification of potential health risks and ultimately improving outcomes for patients. A recent study revealed that 87% of telehealth users expressed satisfaction with their experience, highlighting the effectiveness of these online solutions in meeting patient needs.
However, it is essential to recognize that telemedicine may exacerbate existing disparities in healthcare services if vulnerable populations lack access to technology and digital literacy. Experts, including Bobby Mukkamala, MD, stress the necessity of ensuring equitable access to these services to fully realize their benefits.
Assess Limitations of Digital Healthcare Software
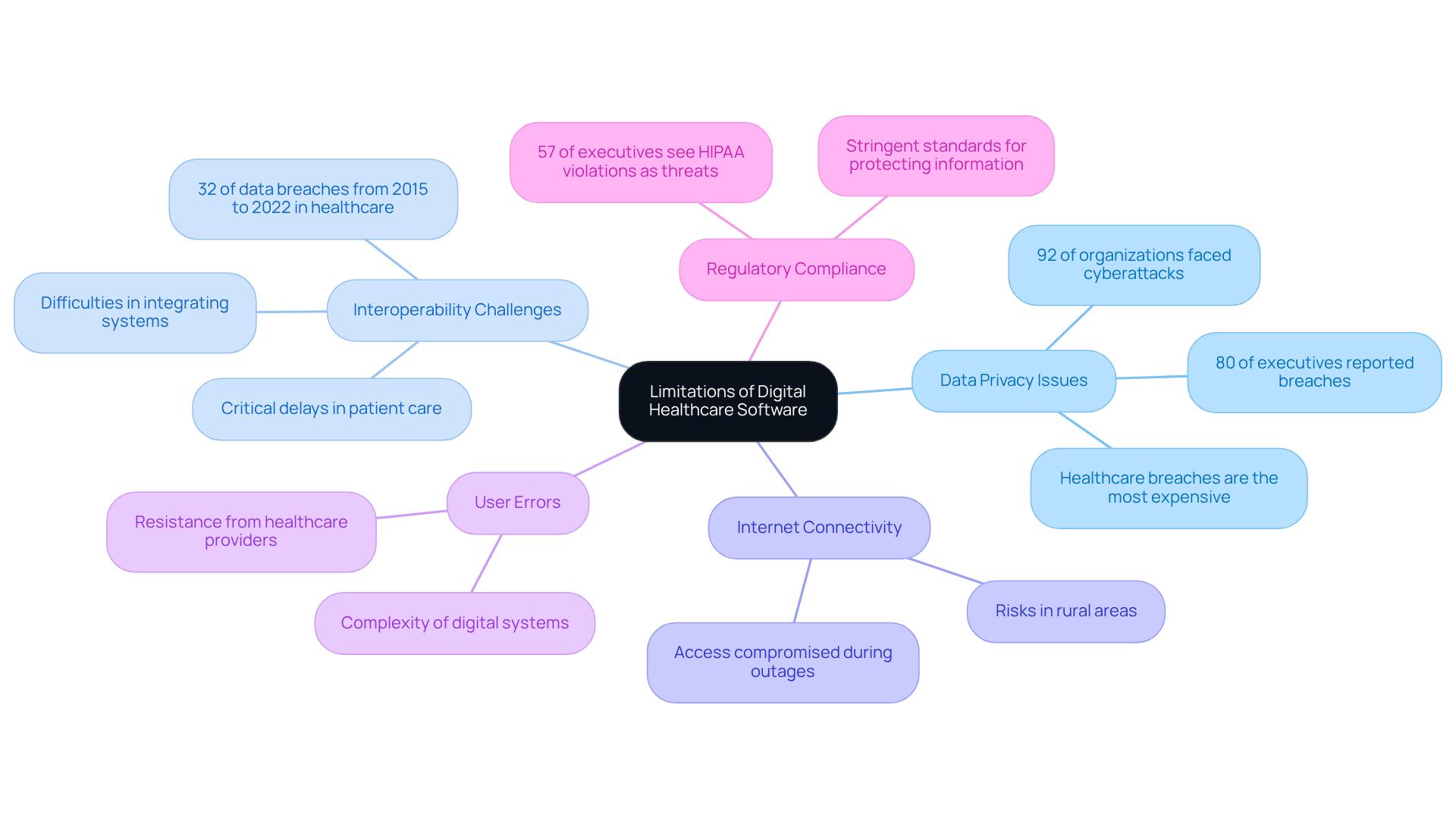
Digital healthcare software presents numerous benefits, yet it also introduces significant challenges that warrant attention. Data privacy issues are paramount; a staggering 92% of medical organizations experienced at least one cyberattack in the past year, with 80% of executives reporting breaches in their information security as a direct result of these attacks. Furthermore, interoperability challenges complicate the landscape; from 2015 to 2022, 32% of all documented data breaches occurred within the medical field, often stemming from difficulties in integrating disparate systems. This lack of seamless communication between online platforms can lead to critical delays in patient care and increased operational costs. Notably, the frequency of data breaches in the medical sector is nearly double that of the financial and manufacturing sectors, highlighting the severity of this issue.
Additionally, reliance on internet connectivity poses risks, particularly in rural areas or during outages, where access to essential health information may be compromised. The complexity of certain digital systems can also lead to user errors or resistance from healthcare providers who are more accustomed to traditional methods. Regulatory compliance adds another layer of challenge; 57% of executives perceive HIPAA violations and privacy breaches as major threats. Digital healthcare software must navigate stringent standards designed to protect individual information, a daunting task for many organizations. As the medical field continues to evolve, addressing these limitations will be crucial for maximizing the potential of digital health solutions.
Evaluate Pros and Cons of Traditional Healthcare Systems
Conventional medical frameworks offer distinct advantages, including established protocols and personal interactions that foster familiarity and trust between individuals and providers. These systems enable individuals to form long-term relationships with their healthcare providers, enhancing the overall care experience.
However, significant drawbacks accompany these benefits. Inefficiencies in data management often lead to prolonged wait times for appointments and limited access to care, particularly for individuals in remote areas. The reliance on paper records can result in errors and delays in treatment, adversely affecting patient outcomes.
For example, one regional healthcare network reported a 15% improvement in its mortality index, underscoring the potential for increased efficiency through improved management practices. Furthermore, medical practitioners emphasize that effective communication and empathy are crucial in building trust, as individuals often remember how they were treated rather than the specifics of their medical care.
This underscores the need for a balance between the personal elements of conventional methods and the effectiveness offered by electronic medical solutions.
Determine Suitability for Your Practice Needs
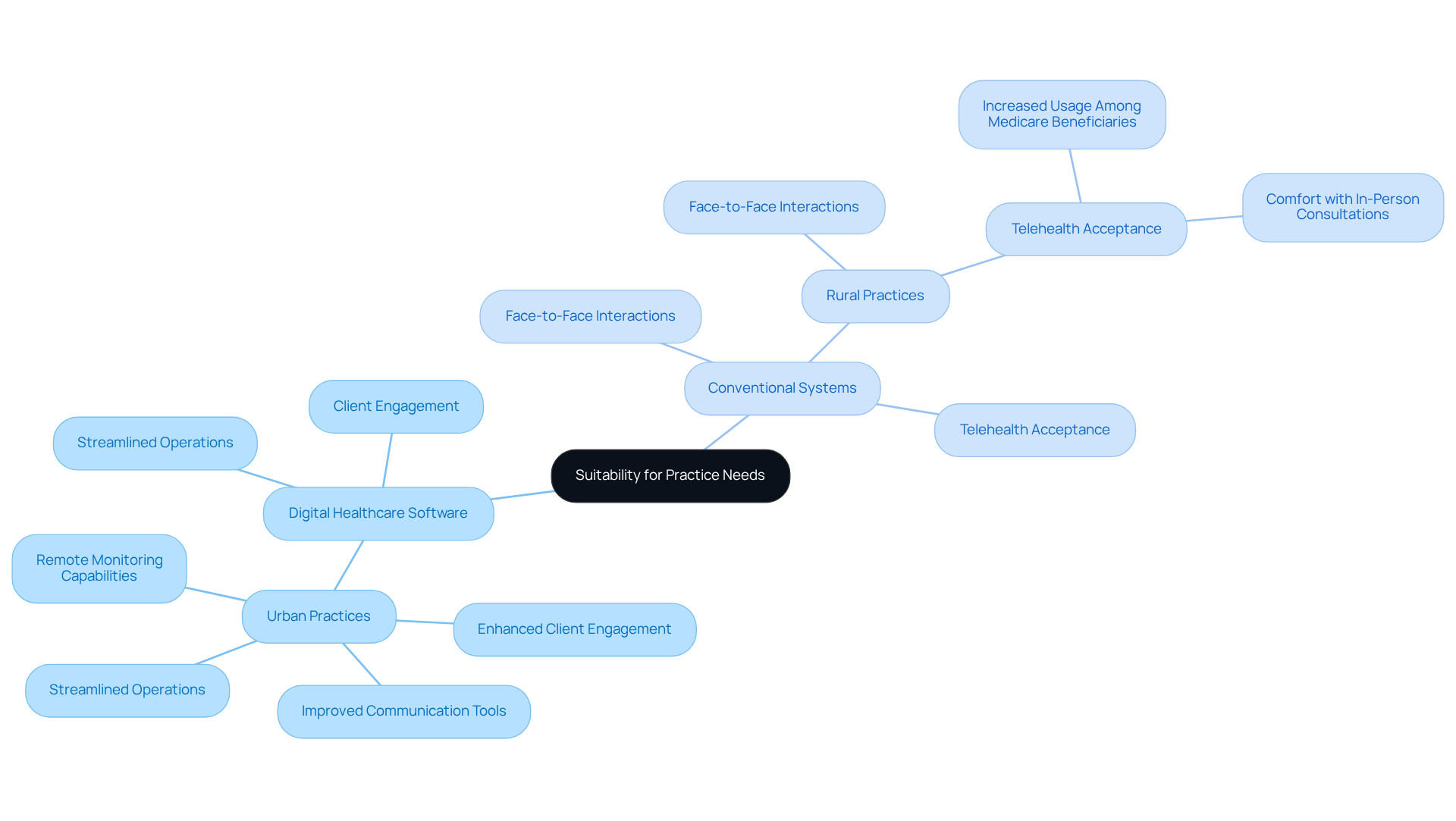
In assessing the appropriateness of digital healthcare software compared to conventional systems, healthcare providers must conduct a thorough evaluation of their specific requirements and the demographics of their clientele. Digital healthcare software is particularly advantageous for practices seeking to enhance client engagement and streamline operations, especially in urban settings where technology adoption is prevalent. For example, urban practices often benefit from improved communication tools and remote monitoring capabilities that digital healthcare software provides.
Conversely, conventional frameworks may still hold significant value in rural areas or among individuals who prefer face-to-face interactions. Many rural individuals may feel more comfortable with in-person consultations, making traditional approaches a more suitable option in these contexts. Data indicates that telehealth usage among rural Medicare beneficiaries increased significantly from 2004 to 2013, underscoring the growing acceptance of technological solutions even in these environments.
Factors influencing the decision between digital healthcare software and conventional platforms include user accessibility, regulatory compliance, and the desired level of technological integration. Notably, the DEA has extended telehealth flexibilities for prescribing controlled substances until December 31, 2025, highlighting the evolving regulatory landscape surrounding digital medical solutions.
Ultimately, the choice should align with the practice’s objectives and the specific needs of its client demographic, ensuring that the selected system effectively supports both operational efficiency and client satisfaction. As Francis Peabody aptly stated, true healing involves caring for the patient’s well-being, underscoring the importance of compassion, empathy, and understanding in healthcare technology decisions.
Conclusion
The evolution of healthcare systems from traditional frameworks to digital solutions marks a significant transformation in the delivery and management of medical services. This shift not only enhances operational efficiency but also markedly improves patient engagement and care quality. As digital healthcare software gains momentum, it is crucial for investors and healthcare providers to grasp the comparative advantages and challenges inherent in both digital and traditional systems.
Insights from this exploration reveal the myriad benefits of digital healthcare software, including:
- Improved access to care
- Streamlined workflows
- Enhanced data management capabilities
However, it is equally vital to recognize the limitations, such as:
- Data privacy concerns
- Potential disparities in access
Traditional healthcare systems continue to provide valuable benefits, particularly in nurturing personal relationships and trust between providers and patients, though they are often accompanied by inefficiencies that can impede timely care.
As the healthcare landscape evolves, stakeholders are urged to carefully evaluate their specific needs. The choice between adopting digital healthcare software or maintaining traditional systems should be informed by the unique demographics of patient populations and the operational objectives of medical practices. A balanced approach that integrates the strengths of both systems may ultimately lead to improved patient outcomes and satisfaction, ensuring that the future of healthcare remains both innovative and compassionate.
Frequently Asked Questions
What is digital healthcare software?
Digital healthcare software includes various technologies aimed at improving medical delivery through computing platforms, connectivity, and software solutions, such as electronic health records (EHRs), telemedicine platforms, and mobile health applications.
How does digital healthcare software differ from traditional systems?
Traditional healthcare systems often rely on paper-based records and in-person consultations, which can limit accessibility and efficiency. In contrast, digital healthcare software facilitates real-time monitoring and seamless data sharing, enhancing operational efficiency and user engagement.
What is the current trend regarding electronic health records in hospitals?
As of 2026, approximately 99% of hospitals are expected to offer electronic access to health records, indicating a significant shift towards digital solutions in healthcare.
What are some advantages of using digital healthcare software?
Digital healthcare software enhances access to care, improves data accuracy, and streamlines workflows. It allows for remote consultations through telemedicine, reducing travel time and increasing convenience for patients.
How did telehealth usage change during the COVID-19 pandemic?
Telehealth appointments increased by 766% during the first three months of the COVID-19 pandemic, highlighting its importance in maintaining medical access.
How does digital healthcare software improve data management?
Digital healthcare software enables healthcare providers to quickly retrieve medical histories, allowing for informed decision-making and improved patient outcomes.
What role do AI and machine learning play in digital healthcare software?
The integration of AI and machine learning with digital healthcare software supports predictive analytics, which helps in early identification of potential health risks and enhances patient outcomes.
What is the patient satisfaction level with telehealth services?
A recent study found that 87% of telehealth users expressed satisfaction with their experience, indicating the effectiveness of these online solutions in meeting patient needs.
What concerns exist regarding access to digital healthcare services?
There is a concern that telemedicine may worsen existing disparities in healthcare services if vulnerable populations lack access to technology and digital literacy. Experts stress the importance of ensuring equitable access to fully realize the benefits of these services.