Introduction
The rapid evolution of medical technology has significantly transformed the healthcare landscape, making effective software integration increasingly critical. As organizations face the complexities of electronic health records, telehealth platforms, and a diverse range of medical devices, understanding best practices for seamless integration is essential. This journey, however, is not without its challenges, including:
- Interoperability issues
- Compliance demands
Healthcare providers must navigate this intricate ecosystem to ensure compliance and security while also striving for improved patient outcomes.
Understand the Landscape of Medical Software Integration
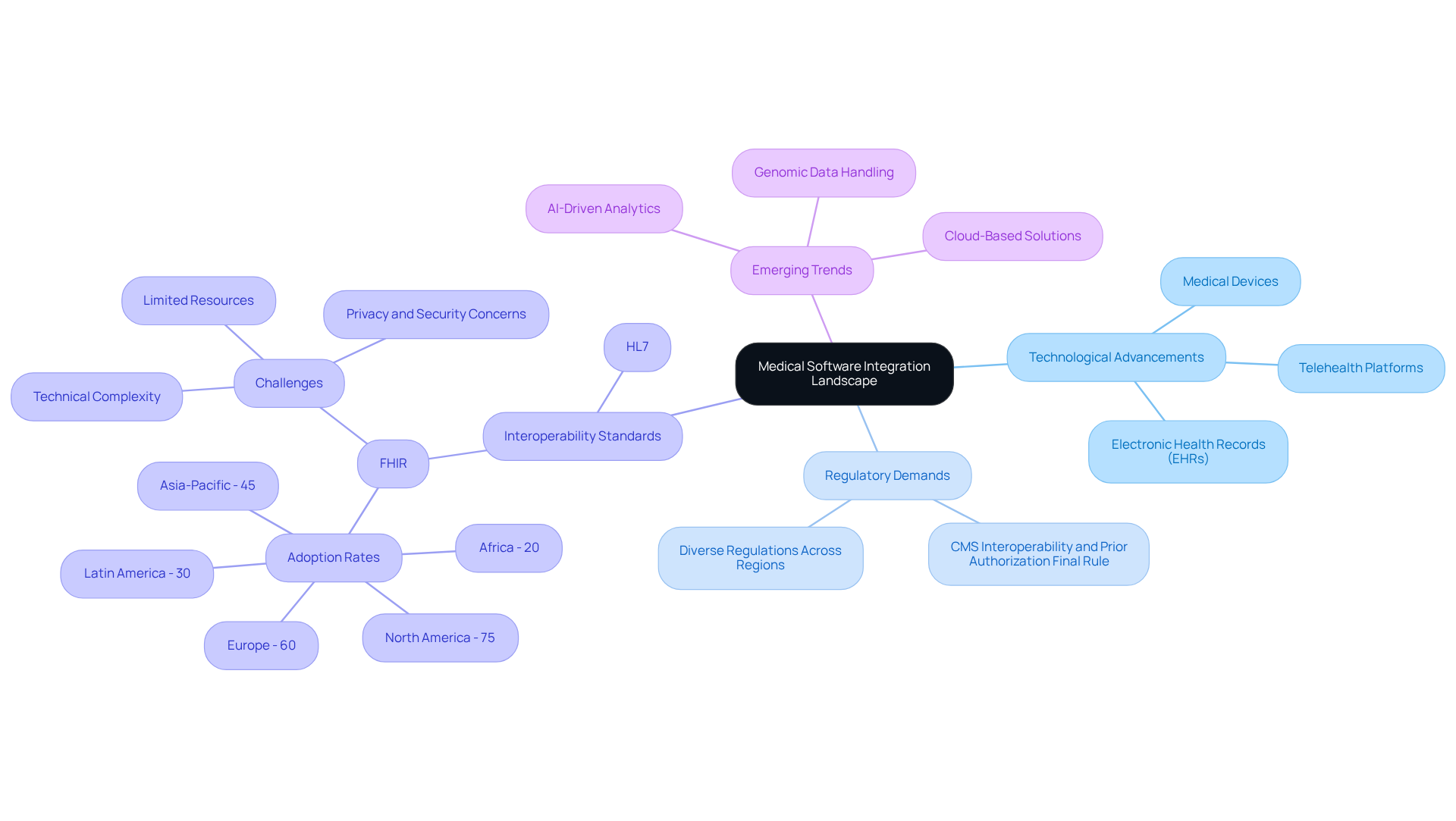
The landscape of medical software integration is shaped by rapid technological advancements and growing regulatory demands. Organizations must navigate a complex ecosystem that involves various stakeholders, including software vendors, telehealth platforms, and various medical devices. Understanding key standards, such as HL7 and FHIR, is essential for facilitating smooth data exchange.
Moreover, the emergence of new technologies and practices is reshaping how healthcare is delivered. It is crucial for stakeholders to remain vigilant regarding compliance and security to ensure their alignment strategies are consistent with industry standards.
Identify and Overcome Common Integration Challenges
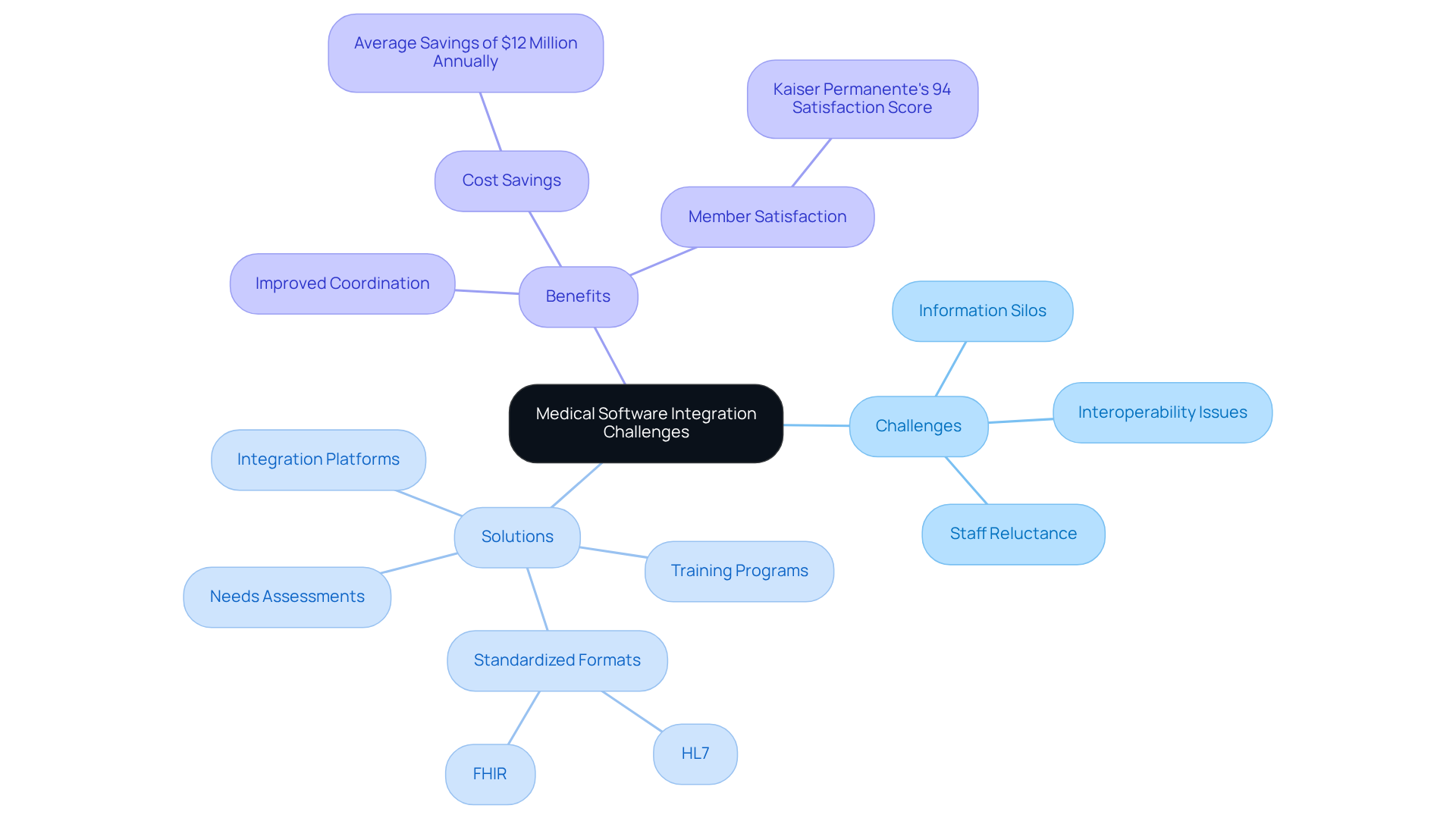
often encounters significant challenges, mainly because of information silos, outdated processes, and staff reluctance to change. Information silos can severely hinder effective communication and information sharing. A Forrester study indicates that 52% of health system executives view the lack of integrated information as a major barrier to delivering quality care. To address these challenges, organizations should initiate thorough planning and actively involve stakeholders from the beginning.
Implementing best practices is crucial for facilitating seamless exchanges across disparate systems. As of 2024, 90% of U.S. hospitals are capable of sending and receiving FHIR-based information, underscoring the advancements in this domain. Additionally, robust training programs are vital to ensure that staff are adequately prepared to adapt to new technologies and processes.
Utilizing integration platforms that support interoperability can significantly improve interoperability, leading to enhanced coordination of care and operational efficiency. A Deloitte study estimates that improved integration can save medical systems an average of $12 million annually in administrative costs, highlighting the financial benefits of addressing these challenges.
Moreover, fostering a culture of collaboration within the organization is essential for effectively overcoming resistance to change. This approach ultimately contributes to a more integrated and efficient ecosystem. Notably, Kaiser Permanente attributes its 94% member satisfaction score to its ability to consolidate data and provide comprehensive care, exemplifying the positive outcomes that can result from successful unification strategies.
Choose the Right Technology and Integration Partners
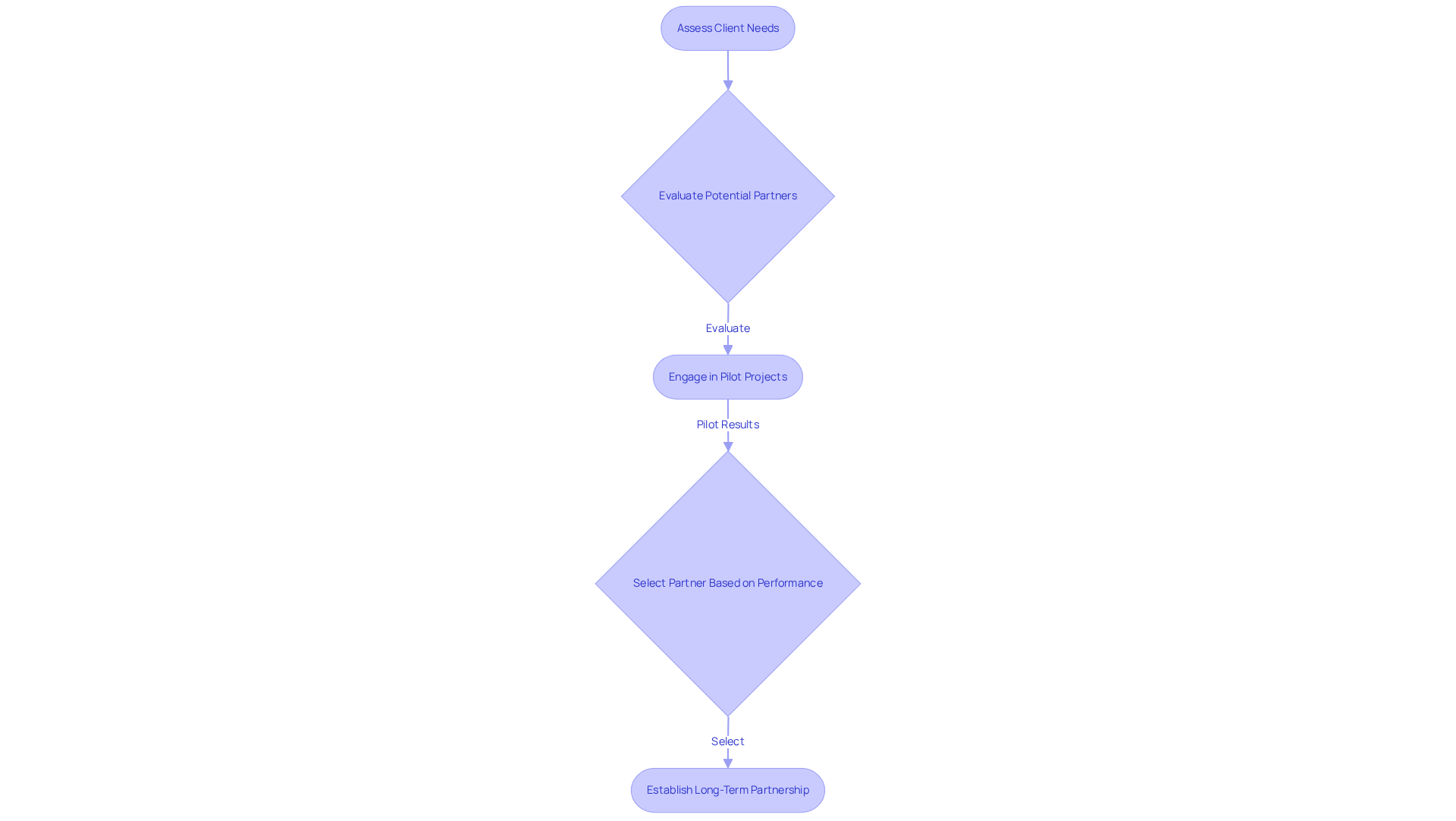
When selecting technology and integration partners, organizations must prioritize vendors with a proven track record in medical software and a robust understanding of integration processes. This approach exemplifies this approach by first collaboratively determining client needs through a comprehensive assessment. Following this, they provide a selection of candidate designers and developers tailored to those specific requirements.
With the market projected to reach USD 388.99 billion by 2030, expanding at a compound annual growth rate of 15.46% from 2025 to 2030, the necessity for trustworthy partners is more critical than ever. Organizations should evaluate potential partners based on their history of successful projects.
It is essential to assess their expertise, as continuous education is vital in navigating the complexities of medical regulations. Engaging in discussions about compatibility and performance prior to entering long-term partnerships is crucial.
Furthermore, consider partners like those that offer solutions to the evolving demands of the medical field, ensuring that your organization remains compliant and effective in a rapidly changing environment.
Ensure Compliance and Security in Integration Processes
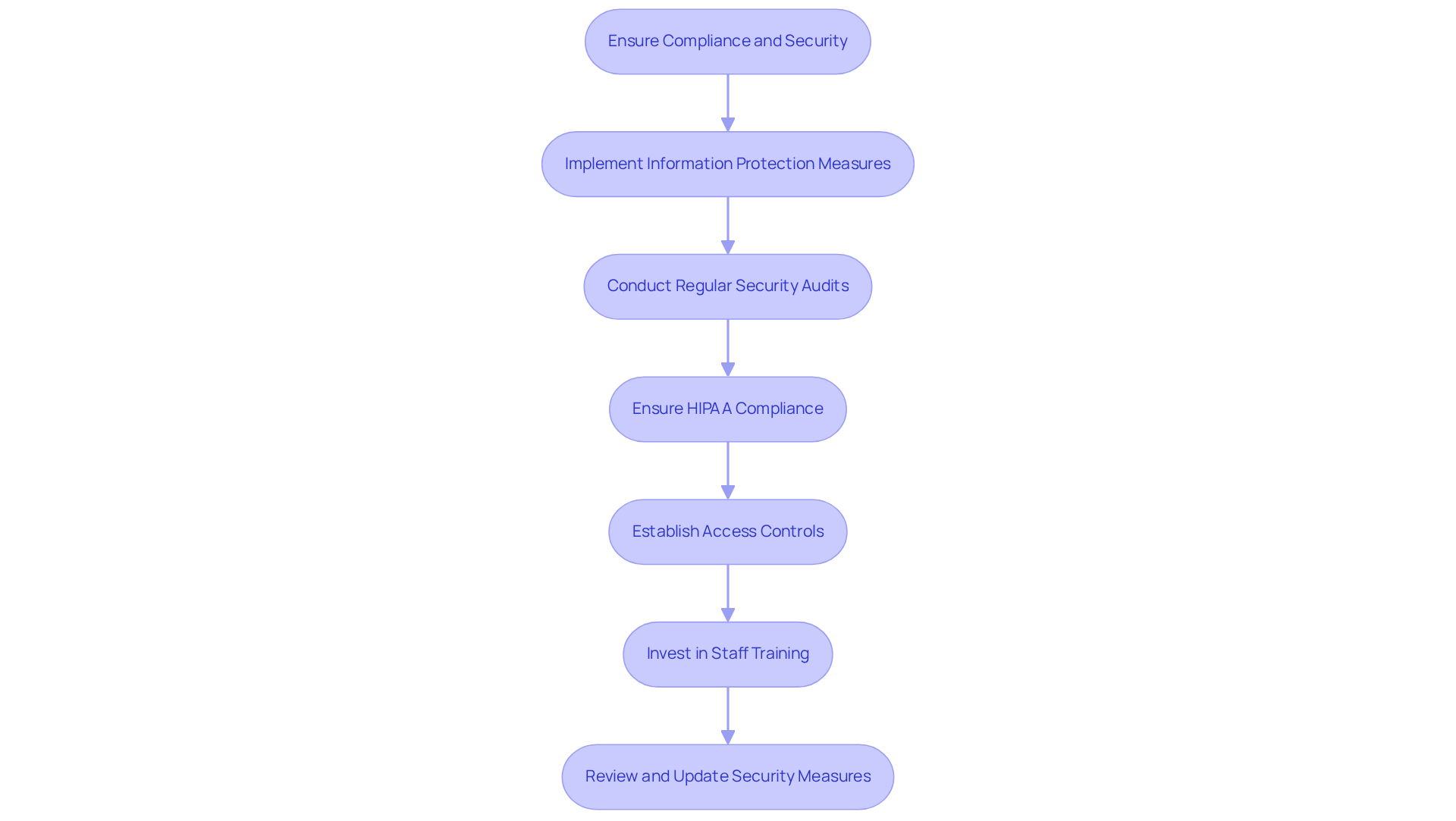
To ensure adherence and security during integration processes, organizations must implement comprehensive security measures. This includes encrypting sensitive information both during transmission and when stored. This is crucial, given that hacking was responsible for nearly 80% of all reported breaches in 2023. That year, the OCR reported 725 breaches, exposing over 133 million records, marking a record year for both breaches and records impacted.
Regular security assessments are essential for identifying vulnerabilities. Additionally, ensuring that all integration partners strictly adhere to compliance standards is non-negotiable. Establishing clear access controls and maintaining detailed audit trails can effectively monitor data access and prevent unauthorized use. This addresses the increasing scrutiny from regulators who demand demonstrable proof of compliance.
Organizations should also stay informed about regulatory changes, as HIPAA’s 2026 updates emphasize security measures, particularly in high-risk environments. Investing in ongoing training for staff is vital to maintain compliance and enhance awareness of evolving threats. For instance, advanced security systems have been shown to detect and contain incidents 98 days faster than average, highlighting the importance of integrating advanced technologies into security protocols.
Consistently reviewing and updating security policies is crucial to adapt to emerging threats, ensuring that entities remain resilient against potential breaches.
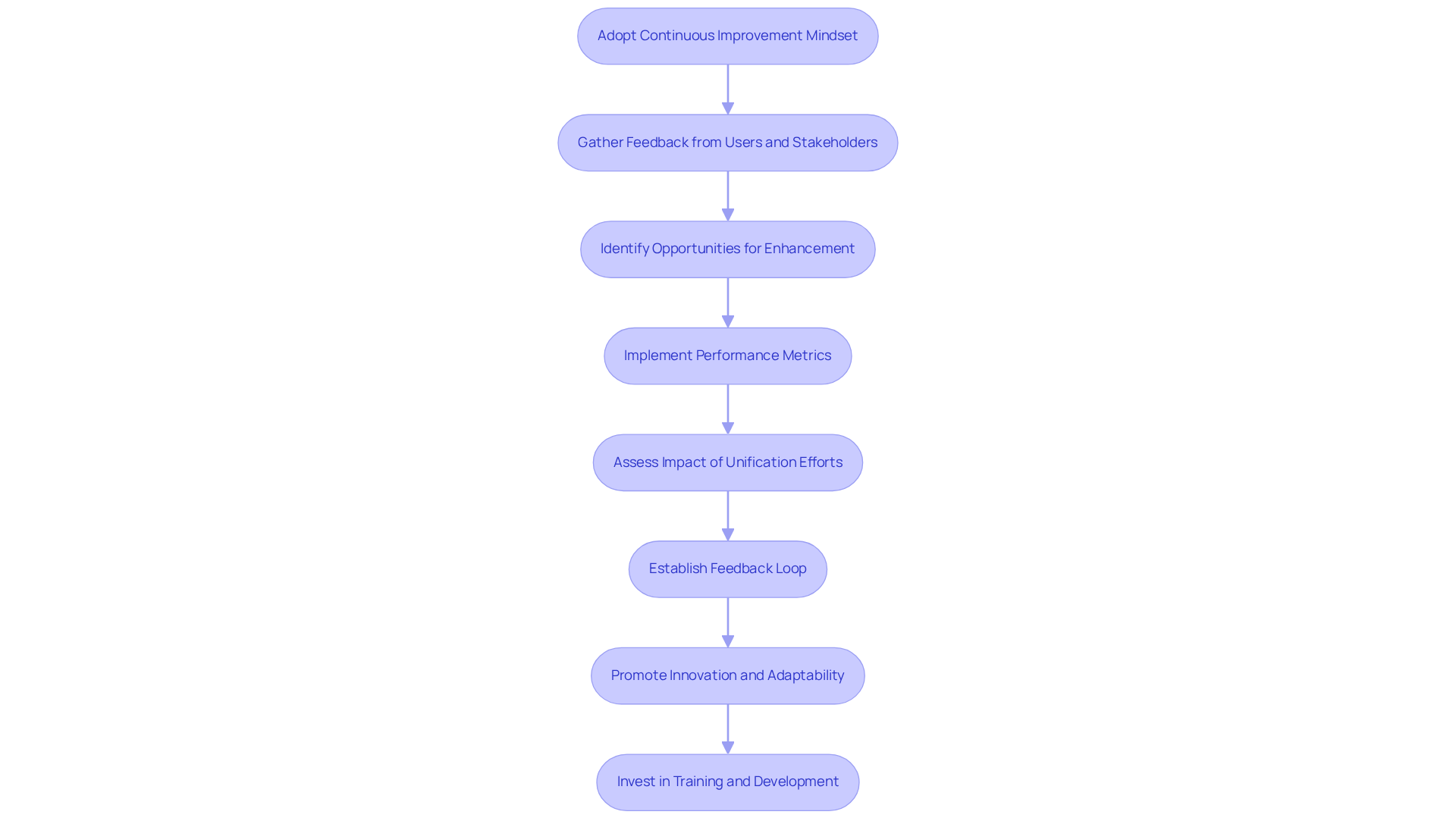
Implement Continuous Improvement Strategies for Integration
To enhance the unification processes of medical software, organizations must adopt a continuous improvement strategy. This approach entails systematically gathering feedback from users and stakeholders to identify opportunities for enhancement. Research indicates that organizations actively implementing improvements can increase efficiency by up to 18%, leading to better service delivery and improved patient outcomes.
Implementing continuous improvement enables organizations to assess the impact of their integration efforts, facilitating data-driven decision-making. Establishing a robust framework, which includes regular reviews and updates to integration strategies, promotes innovation and adaptability in the rapidly evolving healthcare landscape.
Moreover, investing in training ensures that staff possess the latest skills and knowledge necessary to support ongoing improvements. This investment ultimately enhances the overall integration process.
Conclusion
The effective integration of medical software is crucial for enhancing patient care, improving operational efficiency, and ensuring compliance within the dynamic healthcare landscape. By adopting established practices, organizations can adeptly navigate the complexities of integration, aligning their strategies with technological advancements and regulatory requirements.
Key practices such as:
- Understanding the integration landscape
- Overcoming common challenges
- Selecting appropriate technology partners
- Ensuring compliance and security
- Implementing continuous improvement strategies
have been emphasized. Each of these elements is vital in fostering a seamless integration process that ultimately leads to improved healthcare outcomes and heightened satisfaction among stakeholders.
As the healthcare industry continues to evolve, embracing these best practices is not merely advantageous but essential. Organizations are urged to adopt a proactive stance toward medical software integration, consistently seeking innovative solutions and nurturing a culture of collaboration. By doing so, they can enhance their capabilities, improve patient experiences, and maintain a competitive edge, ensuring they are well-prepared to meet future demands.
Frequently Asked Questions
What factors shape the landscape of medical software integration?
The landscape is shaped by rapid technological advancements and growing regulatory demands, requiring organizations to navigate a complex ecosystem involving electronic health records (EHRs), telehealth platforms, and various medical devices.
Why is understanding interoperability standards important in medical software integration?
Understanding interoperability standards, such as HL7 and FHIR, is essential for facilitating smooth information exchange among different medical systems and ensuring effective communication.
What role do cloud-based solutions and AI-driven analytics play in healthcare?
Cloud-based solutions and AI-driven analytics are reshaping how healthcare providers manage patient information, enhancing data accessibility and decision-making processes.
What are common challenges faced in medical software integration?
Common challenges include information silos, interoperability issues, and staff reluctance to change, which can hinder effective communication and information sharing.
How prevalent is the use of FHIR-based information in U.S. hospitals?
As of 2024, 90% of U.S. hospitals are capable of sending and receiving FHIR-based information, indicating significant advancements in medical software integration.
What strategies can organizations implement to overcome integration challenges?
Organizations should conduct thorough needs assessments, involve stakeholders, implement standardized information formats like HL7 and FHIR, and provide robust training programs for staff.
What are the financial benefits of addressing medical software integration challenges?
A Deloitte study estimates that medical software integration and workflow automation can save medical systems an average of $12 million annually in administrative costs.
How can fostering a culture of teamwork and flexibility help in medical software integration?
Fostering a culture of teamwork and flexibility helps overcome resistance to change, contributing to a more integrated and efficient ecosystem.
What example illustrates the positive outcomes of successful unification strategies in healthcare?
Kaiser Permanente’s ability to consolidate data and provide coordinated care has led to a 94% member satisfaction score, exemplifying the benefits of effective integration strategies.
List of Sources
- Understand the Landscape of Medical Software Integration
- The Evolution of the Medical Software Market: Key Shifts from 2026 to 2033 (https://linkedin.com/pulse/evolution-medical-software-market-key-shifts-from-2026-tcxee)
- Global FHIR Adoption Statistics: A Comprehensive Overview – Co-Desion (https://codesion.com/global-fhir-adoption-statistics-a-comprehensive-overview)
- 2026 healthcare AI trends: Insights from experts (https://wolterskluwer.com/en/expert-insights/2026-healthcare-ai-trends-insights-from-experts)
- The top health care trends for 2026 and how they will impact U.S. employers (https://newsroom.cigna.com/top-health-care-trends-for-2026)
- Healthcare IT and EHR Trends to Watch in 2026: What Healthcare Leaders Need to Know (https://csicompanies.com/healthcare-it-and-ehr-trends-to-watch-in-2026-what-healthcare-leaders-need-to-know)
- Identify and Overcome Common Integration Challenges
- 10 Insights from Healthcare Innovators: The Best Quotes from the ‘Leader to Leader’ Podcast in 2024 – Healthcare IT Leaders (https://healthcareitleaders.com/blog/insights-from-healthcare-innovators)
- Bridging Healthcare Data Silos for Better Patient Outcomes (https://teqfocus.com/blog/bridging-healthcare-data-silos-for-better-patient-outcomes)
- Choose the Right Technology and Integration Partners
- 4 Quotes that Underscore the Importance of Compliance (https://compliancebridge.com/4-quote-that-underscore-importance-of)
- Regulatory Innovation as a Catalyst: How New Compliance Strategies Are Speeding Up Healthcare Technology Adoption – MedCity News (https://medcitynews.com/2026/02/regulatory-innovation-as-a-catalyst-how-new-compliance-strategies-are-speeding-up-healthcare-technology-adoption)
- U.S. Healthcare IT Software Market | Industry Report, 2030 (https://grandviewresearch.com/industry-analysis/us-healthcare-it-software-market-report)
- The Hidden Legal Risks in Healthcare AI Implementation: What Medical Practice CEOs Need to Know | Michael Best & Friedrich LLP (https://michaelbest.com/insights/the-hidden-legal-risks-in-healthcare-ai-implementation-what-medical-practice-ceo-102kzcy)
- Healthcare IT Stats, Market Size and Trends Analysis Report (https://radixweb.com/blog/healthcare-it-statistics)
- Ensure Compliance and Security in Integration Processes
- January 2026 Legislative and Compliance Healthcare Updates (https://verisys.com/resources/january-2026-legislative-and-compliance-healthcare-updates)
- Healthcare Data Breach Statistics (https://hipaajournal.com/healthcare-data-breach-statistics)
- 38 Must-Know Healthcare Cybersecurity Stats (https://varonis.com/blog/healthcare-cybersecurity-statistics)
- Healthcare compliance 2026 – Why Proof is the New Policy | Sign In App (https://signinapp.com/blog/healthcare-compliance-in-2026)
- Implement Continuous Improvement Strategies for Integration
- 85 Quotes – Operational Excellence and Continuous Improvement | Rever (https://reverscore.com/85-quotes-operational-excellence-and-continuous-improvement)
- blog.kainexus.com (https://blog.kainexus.com/continuous-improvement/continuous-improvement-leadership-quotes)
- Clinical Intelligence Platforms: Advancing Analytics in Healthcare Systems (https://healthcaretechoutlook.com/news/clinical-intelligence-platforms-advancing-analytics-in-healthcare-systems-nid-4871.html)
- Checking your browser – reCAPTCHA (https://pmc.ncbi.nlm.nih.gov/articles/PMC11031995)
- AI-powered process improvement shows big patient experience ROI (https://healthcareitnews.com/news/ai-powered-process-improvement-shows-big-patient-experience-roi)
