Introduction
Clinical data integration is pivotal in transforming healthcare delivery, ensuring that medical professionals have access to comprehensive patient information necessary for informed decision-making. This process enhances care coordination and accuracy while addressing critical challenges such as information silos and regulatory compliance that impede effective patient care. As healthcare organizations pursue improved interoperability, a pressing question arises: what best practices can be implemented to navigate these complexities and fully leverage the potential of clinical data integration?
Define Clinical Data Integration and Its Importance
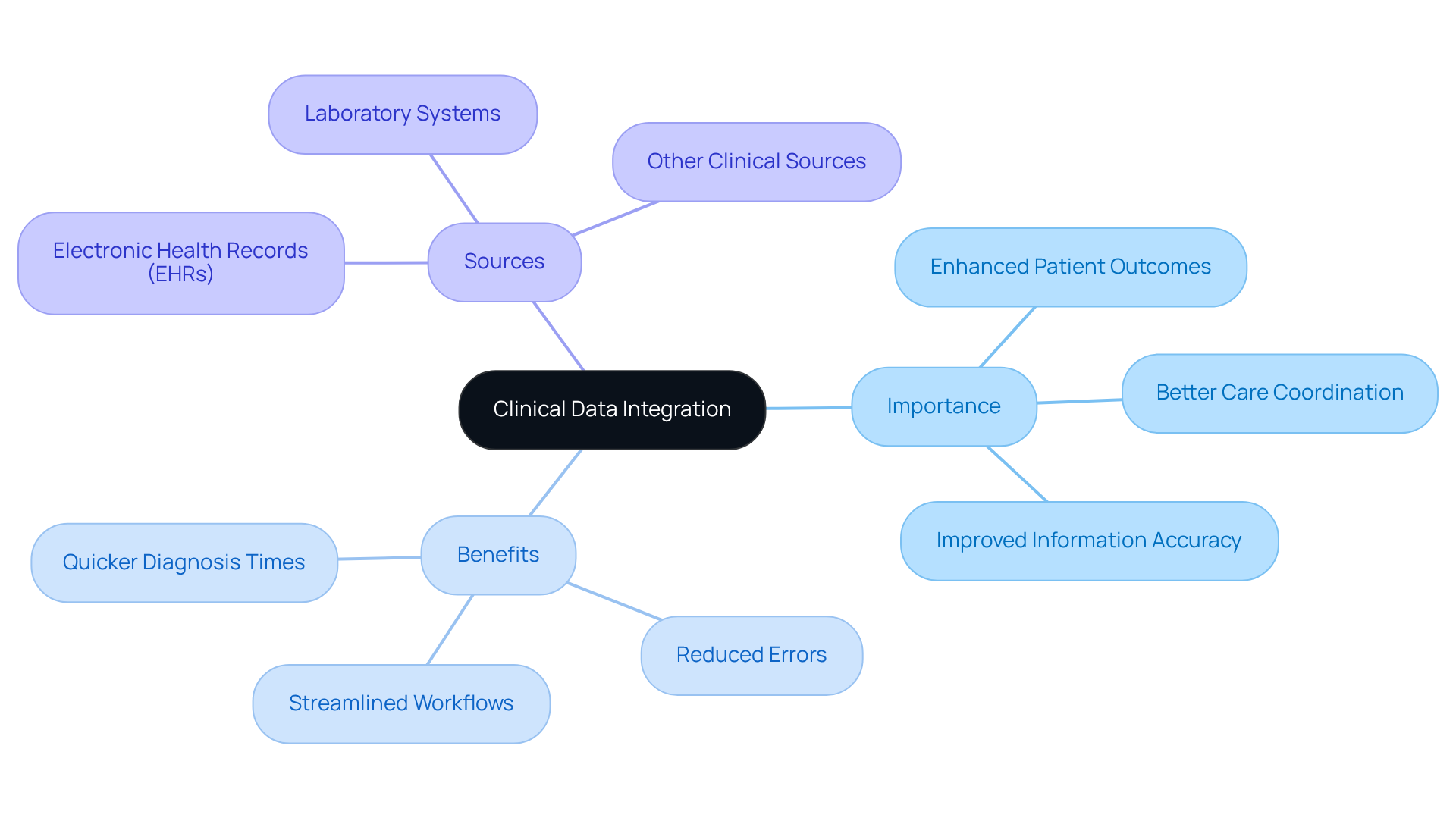
Clinical data integration involves the process of aggregating and harmonizing clinical information from various sources into a unified format. This unification is essential for ensuring that medical providers have access to complete individual information, which is necessary for making informed clinical decisions. The significance of clinical data integration lies in its ability to enhance patient outcomes by promoting better care coordination, improving information accuracy, and allowing real-time access to essential health details.
Healthcare organizations can streamline workflows, reduce errors, and ultimately provide higher quality care by utilizing clinical data integration from electronic health records (EHRs), laboratory systems, and other clinical sources. Emergency departments demonstrate significantly quicker diagnosis times when doctors can promptly access comprehensive medical histories, illustrating the immediate advantages of unification in critical care scenarios.
As Lifepoint Informatics states, “When systems exchange information accurately and swiftly, individuals receive improved care.” Furthermore, the global healthcare information unification market is projected to reach $7.1 billion by 2026, underscoring the necessity and significance of efficient unification methods in enhancing care for individuals.
Identify Challenges in Clinical Data Integration
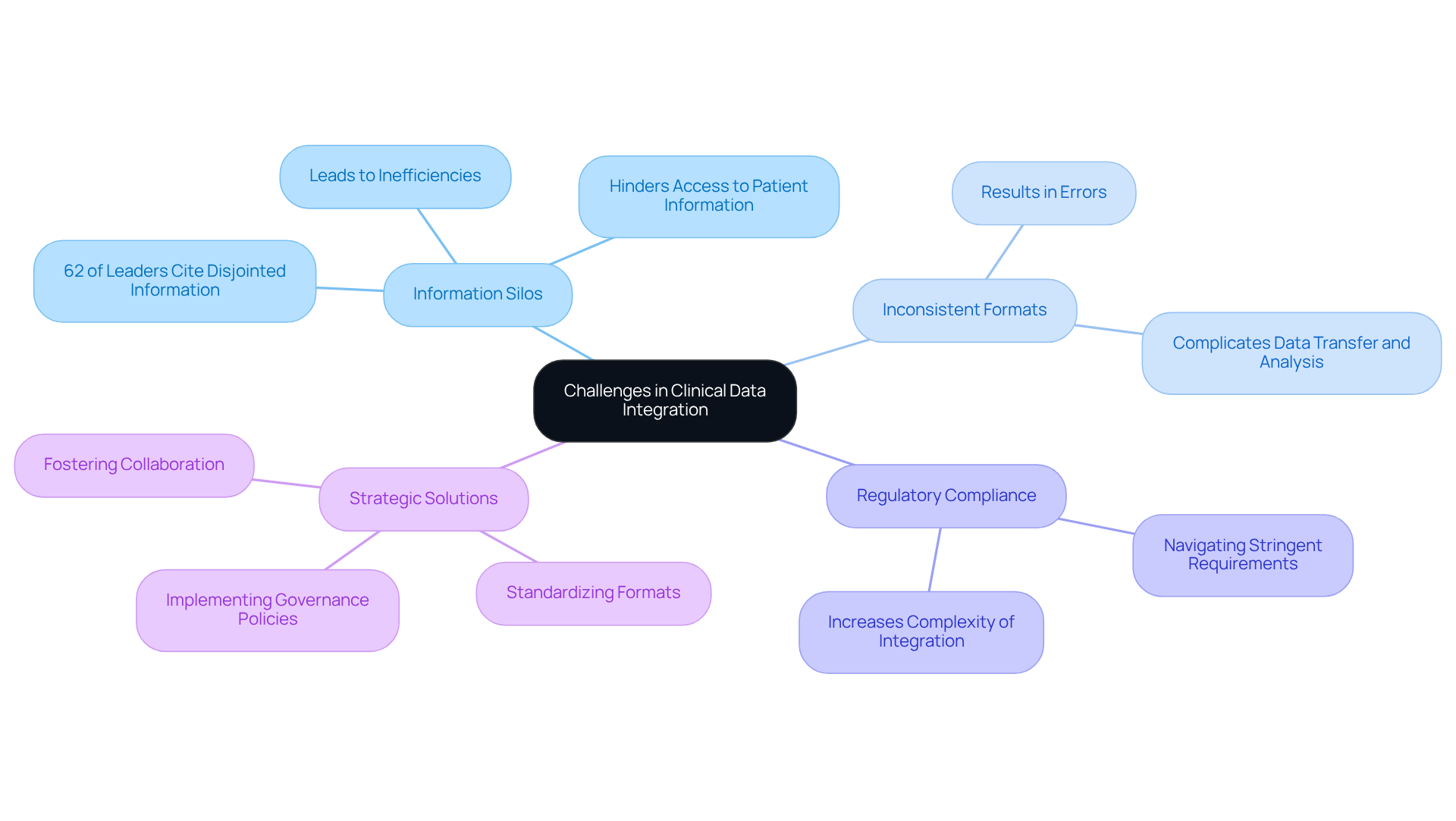
Effective clinical data integration encounters several challenges, particularly information silos, inconsistent formats, and regulatory compliance issues. Information silos arise when knowledge is confined within separate systems, hindering access to essential patient information. This fragmentation results in significant inefficiencies, as medical organizations struggle to share critical information across platforms. Statistics indicate that 62% of medical leaders identify disjointed information as the primary barrier to achieving clinical data integration and improving interoperability. Furthermore, the lack of clinical data integration in fragmented healthcare systems imposes an estimated cost of $3.1 trillion annually on the global healthcare economy due to inefficiencies, underscoring the broader impact of information silos. The lack of uniform information formats complicates transfer and analysis, often resulting in errors that can jeopardize patient care.
Regulatory compliance adds another layer of complexity, as organizations must navigate stringent requirements while striving to achieve clinical data integration. The rapid increase in information generated from diverse sources, such as wearable devices and telehealth platforms, further complicates unification efforts. To tackle these challenges, a strategic approach is imperative. This involves:
- Standardizing formats
- Implementing robust governance policies
- Fostering collaboration among stakeholders
Successful initiatives, such as the adoption of interoperability standards like FHIR and the integration with Health Information Exchanges (HIEs), illustrate that overcoming information silos is achievable, leading to enhanced sharing and improved patient outcomes.
Implement Best Practices for Effective Data Integration
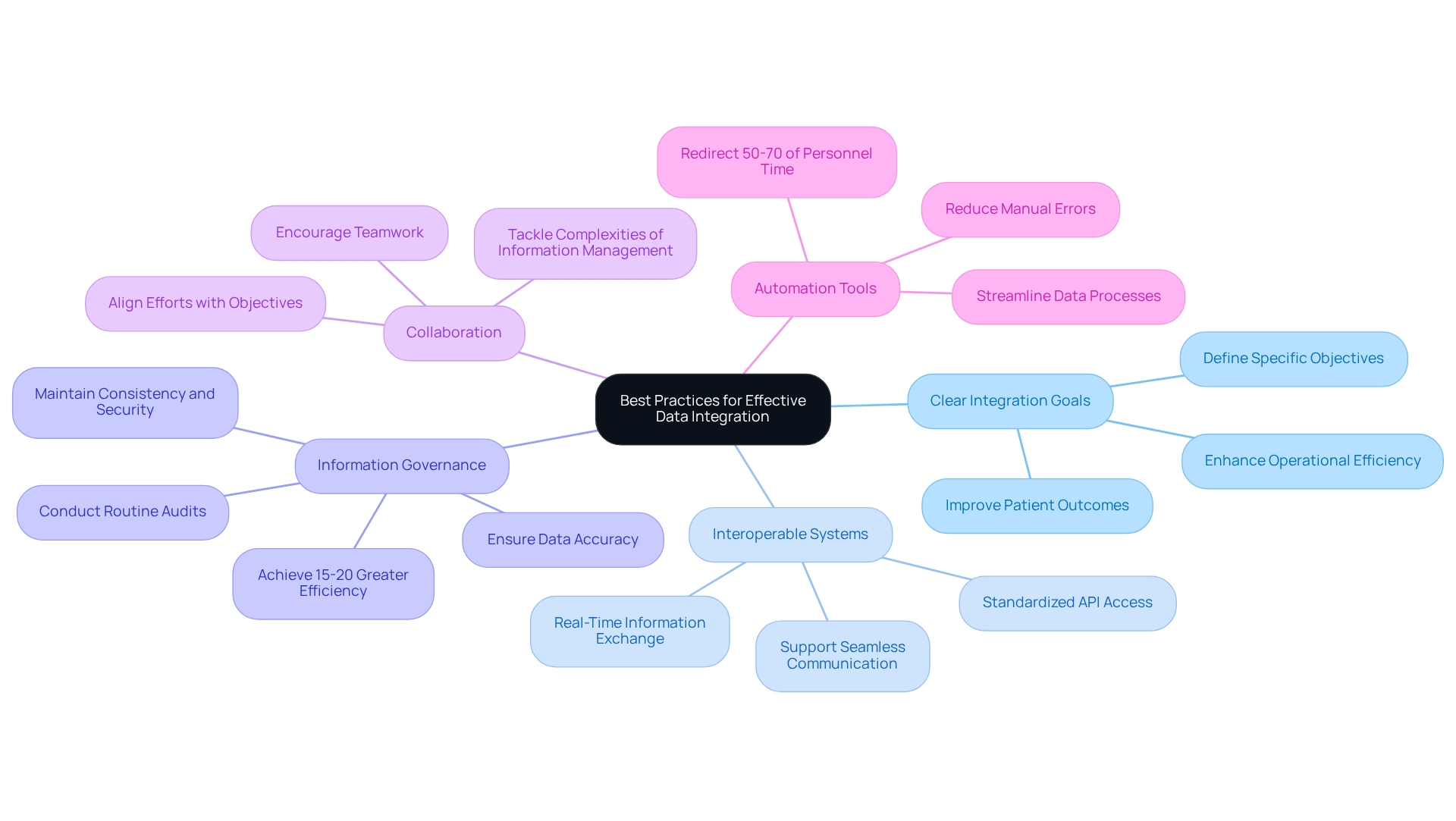
To achieve effective clinical data integration, organizations should adopt several best practices:
- Establish Clear Integration Goals: Defining specific objectives for information integration projects is crucial. Goals such as improving patient outcomes or enhancing operational efficiency provide direction and measurable benchmarks for success.
- Invest in Interoperable Systems: Selecting technologies that support interoperability is essential. Systems must be capable of seamless communication, as required by the 21st Century Cures Act, which highlights the necessity for standardized API access and real-time information exchange.
- Implement Information Governance: Creating strong information governance policies guarantees information accuracy, consistency, and security. Routine audits and quality assessments are essential, as organizations with developed governance frameworks report 15-20% greater operational efficiency, directly affecting patient care and regulatory compliance.
- Foster Collaboration: Encouraging teamwork among clinical, IT, and administrative teams is essential to align cooperative efforts with organizational objectives. This multidisciplinary approach helps tackle the complexities of information management and enhances the effectiveness of clinical data integration efforts.
- Utilize Automation Tools: Leveraging automation tools can significantly streamline information extraction, transformation, and loading processes. This reduces manual errors and improves efficiency, allowing healthcare organizations to focus on performance improvement initiatives rather than administrative burdens. Research shows that automating organized information capture can redirect 50-70% of personnel time from information collection to performance improvement efforts.
Leverage Technology for Enhanced Data Integration
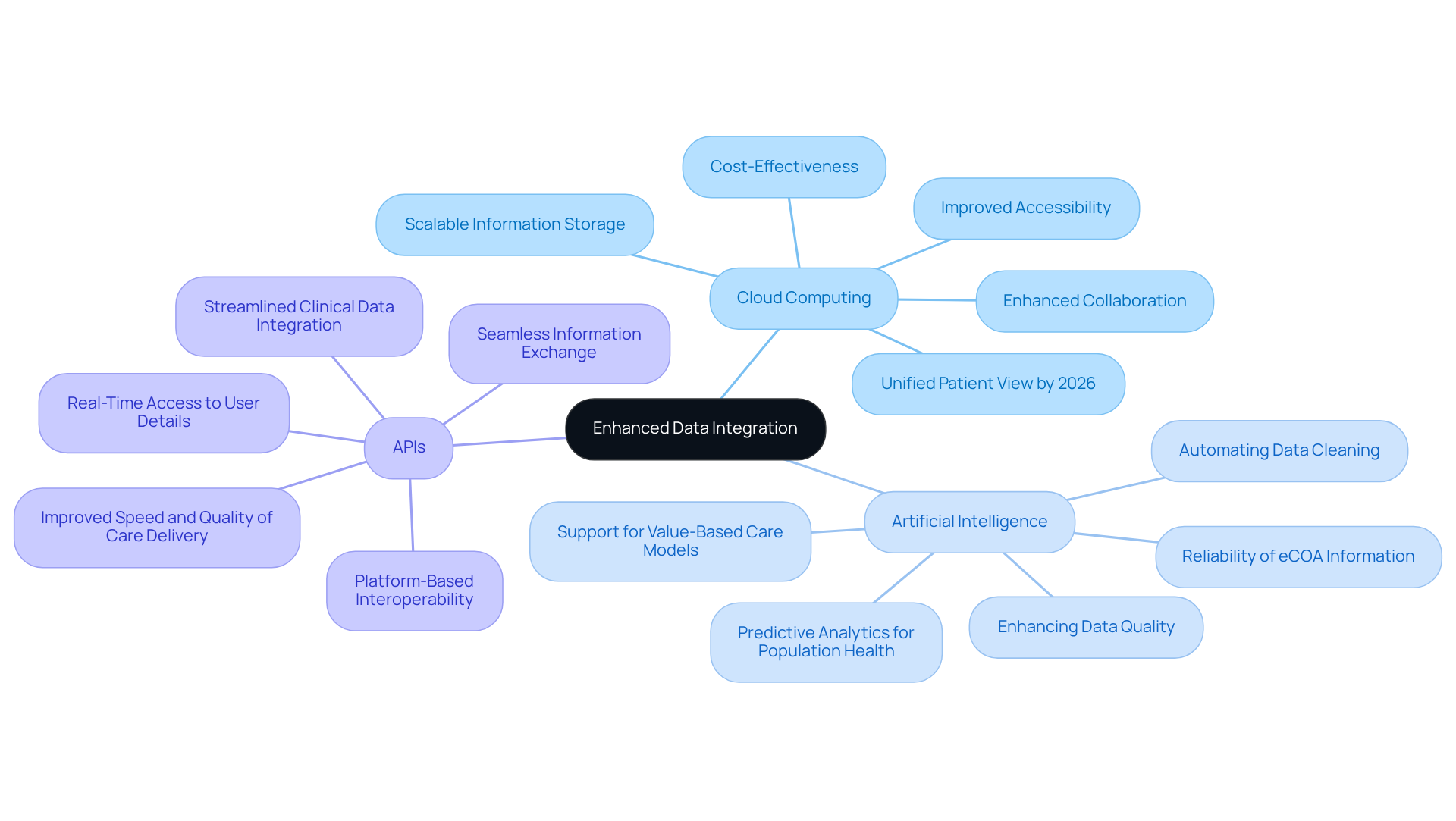
To enhance clinical data integration, organizations should leverage advanced technologies such as cloud computing, artificial intelligence (AI), and application programming interfaces (APIs).
- Cloud Computing: The utilization of cloud-based solutions facilitates scalable information storage and processing, enabling organizations to efficiently manage large volumes of data. The benefits of cloud computing in medical information management include improved accessibility, cost-effectiveness, and enhanced collaboration among stakeholders. By 2026, the medical sector will necessitate a unified perspective of the patient, which cloud solutions-particularly those employing FHIR-native architectures-can provide by merging various information sources into a cohesive framework.
- Artificial Intelligence: AI plays a crucial role in automating information cleaning and normalization processes, significantly enhancing data quality and reducing the time required for integration. By 2026, AI tools will be indispensable for managing population health at scale, offering predictive analytics that empower healthcare teams to act earlier and with greater accuracy. This capability is essential as organizations transition towards value-based care models, where the integrity of information directly impacts financial performance. Moreover, the growing emphasis on the reliability and integrity of electronic Clinical Outcome Assessment (eCOA) information underscores the importance of AI in ensuring high-quality management.
- APIs: The implementation of APIs facilitates seamless information exchange between various systems, allowing for real-time access to user details. This unification is critical as organizations move away from years of point-to-point interfaces towards platform-based interoperability, thereby enhancing the speed and quality of care delivery. By adopting these technologies, including robust API frameworks, healthcare organizations can streamline their clinical data integration efforts, improve data accuracy, and ultimately enhance overall patient care.
Conclusion
Clinical data integration is an essential process that consolidates clinical information from various sources into a cohesive format, thereby enhancing patient care and outcomes. By ensuring healthcare providers have access to complete and accurate patient data, organizations can improve care coordination, reduce errors, and facilitate timely clinical decisions, especially in critical care settings.
This article outlines several key practices and strategies for achieving effective clinical data integration:
- Establishing clear integration goals
- Investing in interoperable systems
- Implementing robust information governance
- Fostering collaboration among teams
- Leveraging advanced technologies such as cloud computing, AI, and APIs
These strategies not only address the barriers to integration but also underscore the significant financial implications of inefficiencies within the healthcare system.
Given the increasing importance of clinical data integration, organizations must prioritize these best practices to enhance patient care and operational efficiency. Embracing technology and fostering collaboration among stakeholders will be vital in navigating the complexities of data management. By taking decisive action towards effective clinical data integration, healthcare organizations can ensure they are well-equipped to meet the evolving demands of patient care and improve overall health outcomes.
Frequently Asked Questions
What is clinical data integration?
Clinical data integration is the process of aggregating and harmonizing clinical information from various sources into a unified format.
Why is clinical data integration important?
It is important because it ensures that medical providers have access to complete individual information necessary for making informed clinical decisions, which enhances patient outcomes, promotes better care coordination, and improves information accuracy.
How does clinical data integration benefit healthcare organizations?
It helps streamline workflows, reduce errors, and ultimately provide higher quality care by utilizing data from electronic health records (EHRs), laboratory systems, and other clinical sources.
What impact does clinical data integration have in emergency departments?
In emergency departments, clinical data integration leads to significantly quicker diagnosis times, as doctors can promptly access comprehensive medical histories.
What is the projected market size for global healthcare information unification by 2026?
The global healthcare information unification market is projected to reach $7.1 billion by 2026.
How does accurate and swift information exchange improve patient care?
When systems exchange information accurately and swiftly, individuals receive improved care, as stated by Lifepoint Informatics.
List of Sources
- Define Clinical Data Integration and Its Importance
- Improve patient outcomes through healthcare data integration | Boost efficiency and data accuracy | Lumenalta (https://lumenalta.com/insights/data-integration-in-healthcare)
- Clinical Data Integration Platform: 5 Powerful Benefits in 2025 (https://lifebit.ai/blog/clinical-data-integration-platform)
- Healthcare Data Integration: The Key to Better Patient Outcomes – Lifepoint Informatics (https://lifepoint.com/healthcare-data-integration-the-key-to-better-patient-outcomes)
- Why Clinical Data Integration Is Critical in Healthcare? – Vorro (https://vorro.net/why-clinical-data-integration-is-critical-for-modern-healthcare)
- In 2026, healthcare data will show a unified view of the patient (https://healthcareitnews.com/news/2026-healthcare-data-will-show-unified-view-patient)
- Identify Challenges in Clinical Data Integration
- 7 Healthcare Data Silos Killing Efficiency in 2026 (And How to Spot Them) – AI Enabled Data Integrations and Analytics (https://bizdata360.com/7-healthcare-data-silos)
- 7 EHR Integration Challenges In 2026 (+ Solutions) (https://murphi.ai/ehr-integration-challenges)
- Interoperability woes still plague healthcare in 2026. Here’s what to do about it. | TechTarget (https://techtarget.com/searchhealthit/feature/Interoperability-woes-still-plague-healthcare-in-2026-Heres-what-to-do-about-it)
- 7 Clinical Informatics Challenges in 2026 Amid AI Adoption | ATA posted on the topic | LinkedIn (https://linkedin.com/posts/americantelemed_clinicalinformatics-healthit-aiinhealthcare-activity-7408876707161477122-TRPU)
- Data Silos Stall AI Expansion in Health Care Revenue Cycle – ACA International (https://acainternational.org/news/data-silos-stall-ai-expansion-in-health-care-revenue-cycle)
- Implement Best Practices for Effective Data Integration
- Data Quality Improvement Stats from ETL – 50+ Key Facts Every Data Leader Should Know in 2026 (https://integrate.io/blog/data-quality-improvement-stats-from-etl)
- 21st Century Cures Act EHR Requirements: 2026 Integration Guide (https://anisolutions.com/2026/04/02/how-the-21st-century-cures-act-changes-your-ehr-integration-requirements)
- Why Data Management in Healthcare Must Evolve in 2026 (https://americandatanetwork.com/healthcare-analytics/why-data-management-in-healthcare-must-evolve-2026)
- Data Governance in Healthcare: A Board-Level Imperative (https://blog.mastek.com/data-governance-in-healthcare-board-level-concern)
- Best Practices in Clinical Data Management for High-Quality Outcomes – Vita Global Sciences (https://vitaglobalsciences.com/blog/best-practices-in-clinical-data-management)
- Leverage Technology for Enhanced Data Integration
- Clinical trial predictions and the role of technology in 2026 (https://clinicaltrialsarena.com/sponsored/clinical-trial-predictions-and-the-role-of-technology-in-2026)
- In 2026, healthcare data will show a unified view of the patient (https://healthcareitnews.com/news/2026-healthcare-data-will-show-unified-view-patient)
- Technology Trends Shaping Clinical Trial Execution in 2026 | Applied Clinical Trials Online (https://appliedclinicaltrialsonline.com/view/technology-trends-clinical-trial-execution-2026)
- 2026 Clinical Data Trend Report | Veeva (https://veeva.com/2026-clinical-data-trend-report)
- Future of Healthcare Integration Technology in 2026 (https://emorphis.health/blogs/future-of-healthcare-integration-technology)
