Introduction
Navigating the complex landscape of medical device software engineering requires a deep understanding of the regulatory frameworks and quality standards that govern industry practices.
With the FDA set to transition to the Quality Management System Regulation in 2026, developers must urgently align their practices with evolving compliance requirements, including the recent Software Bill of Materials mandate.
This article explores best practices that not only ensure adherence to these regulations but also position compliance as a strategic advantage.
How can companies effectively balance the complexities of regulatory demands with the need for innovation in a rapidly changing environment?
Understand Regulatory Requirements and Quality Standards
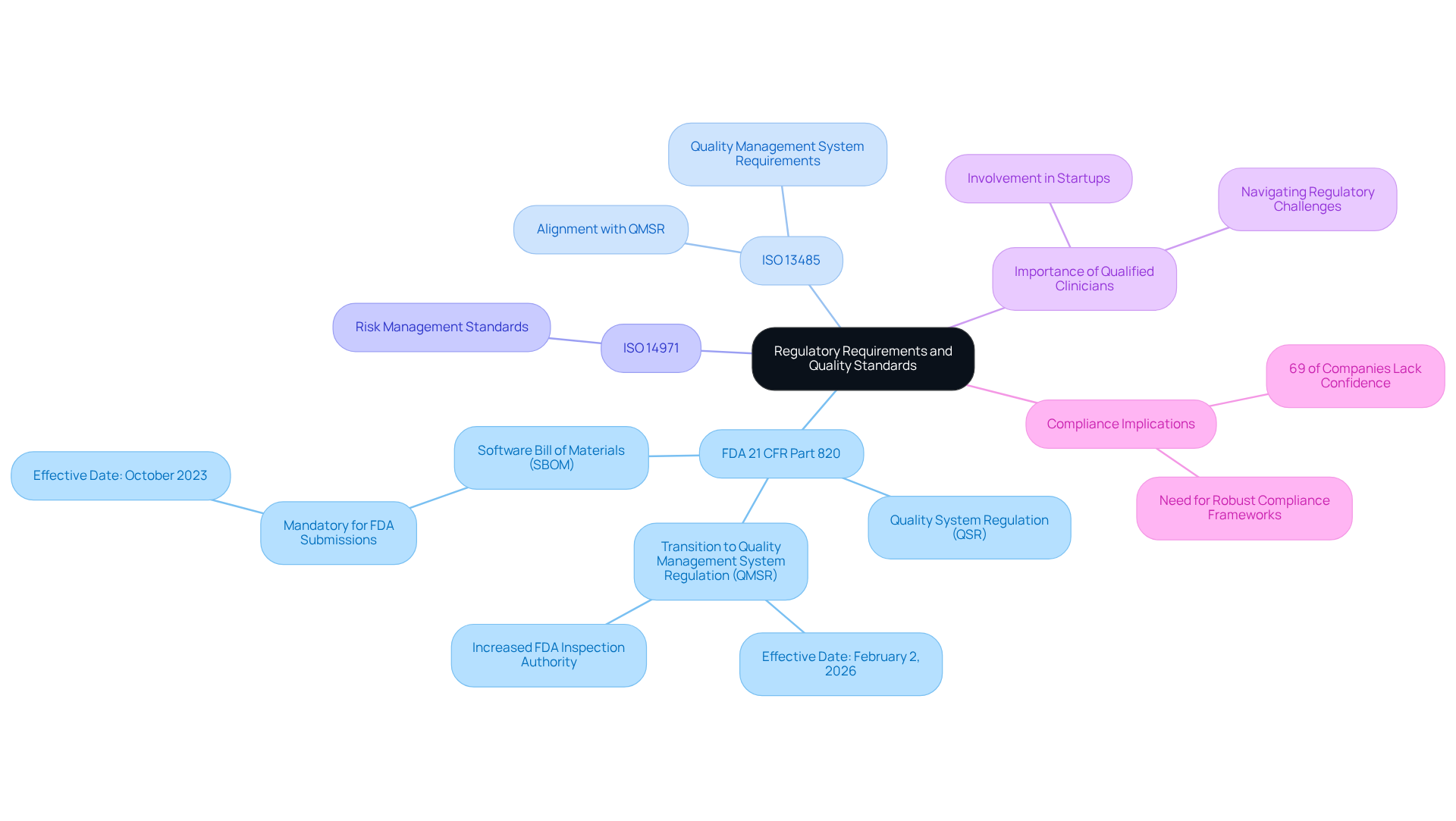
Navigating the landscape of medical device software engineering requires a comprehensive understanding of the regulatory requirements and quality standards that govern the industry. Central to this is the FDA’s 21 CFR Part 820, which outlines the Quality System Regulation (QSR) for medical products. Notably, this regulation will transition to the Quality Management System Regulation (QMSR) effective February 2, 2026. Furthermore, ISO 13485 specifies the requirements for a quality management system, while adherence to ISO 14971 for managing uncertainties is also crucial.
Developers must stay informed about the latest updates in these regulations, particularly the mandatory Software Bill of Materials (SBOM) requirements for FDA submissions, which took effect in October 2023. By ensuring compliance with these standards, developers can mitigate risks and enhance the safety and effectiveness of their medical products. Recent statistics indicate that 69% of companies lack confidence in their current quality management systems‘ ability to support future growth, underscoring the urgent need for robust compliance frameworks.
Industry leaders stress the importance of aligning quality management systems with these standards. For instance, Katie Ogden, a Portfolio Manager in Pharma, points out that while certain products may be exempt from CGMP requirements, manufacturers are still obligated to maintain complaint files and adhere to recordkeeping responsibilities. This perspective is echoed by experts who highlight that startups, in particular, must involve to make informed decisions regarding patient safety, as navigating these regulations can be challenging without the right expertise.
By integrating quality into every phase of product development, companies in the medical device software engineering sector can transform compliance from a regulatory burden into a catalyst for innovation and differentiation.
Implement Effective Risk Management Strategies
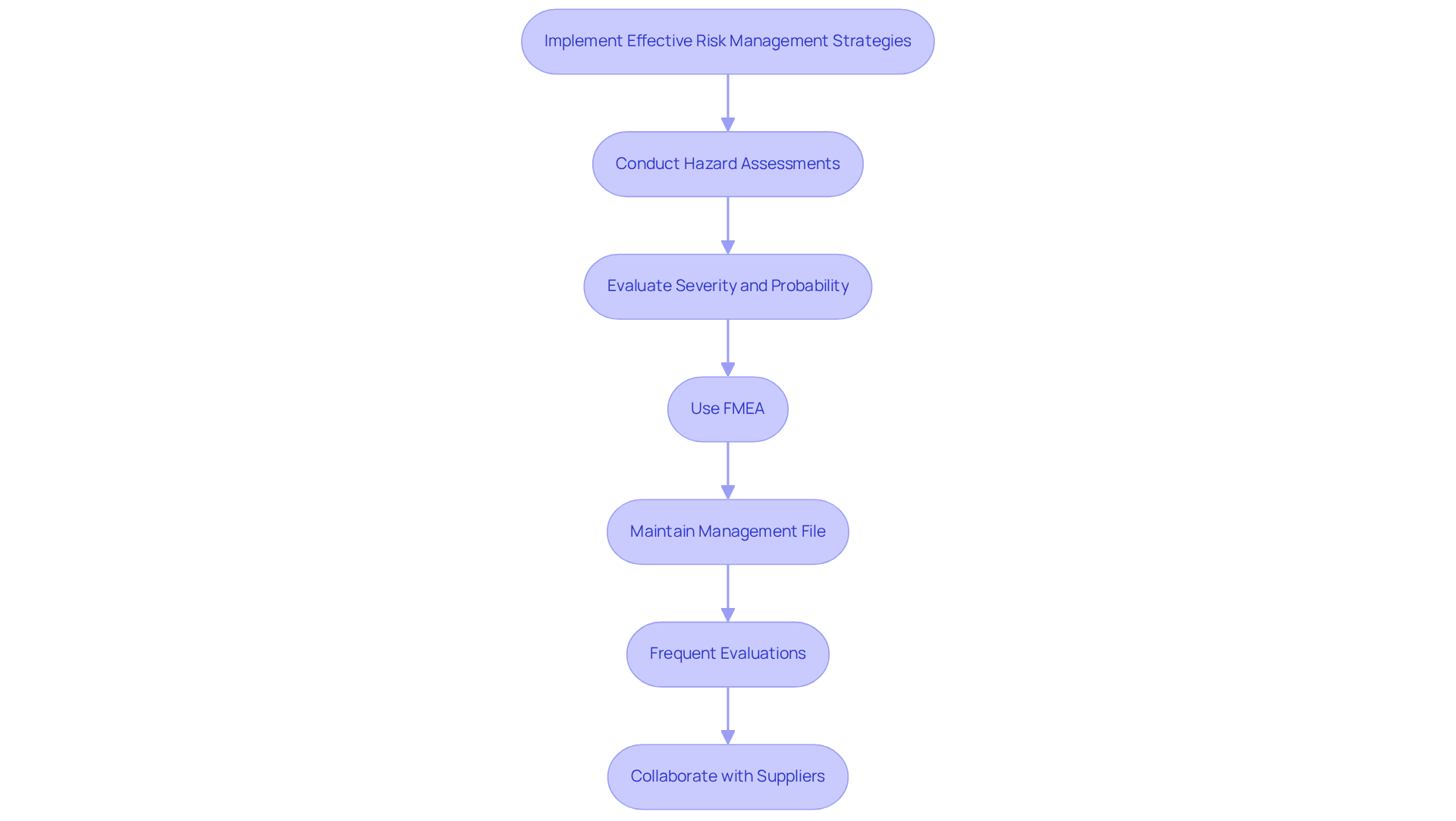
Efficient hazard management approaches are crucial for advancing medical device software engineering applications, particularly in compliance with the ISO 14971 standard. In medical device software engineering, developers must conduct thorough hazard assessments to identify potential dangers associated with their software, evaluating both the severity and probability of threats. As emphasized by Dale E. Jones, carefully evaluating and managing enterprise threats can safeguard trust, making it essential for developers to establish suitable measures for hazard reduction.
Methods such as Failure Mode and Effects Analysis (FMEA) are vital for systematically evaluating threats in medical device software engineering. These methods in medical device software engineering enable teams to pinpoint failure points and assess their effects on equipment functionality and patient safety. Additionally, maintaining a management file throughout the application creation lifecycle is essential in medical device software engineering; it ensures that all identified threats are recorded, tracked, and handled efficiently.
Frequent evaluations and revisions to the management strategy in medical device software engineering are necessary to adapt to changing information and shifts in the regulatory environment. This process strengthens the in medical device software engineering during the creation of medical products. Furthermore, collaboration with medical equipment suppliers is advised to ensure coordinated efforts in managing challenges, as highlighted in recent discussions about the decentralized accountability framework in healthcare environments.
Adopt a Structured Software Development Life Cycle (SDLC)
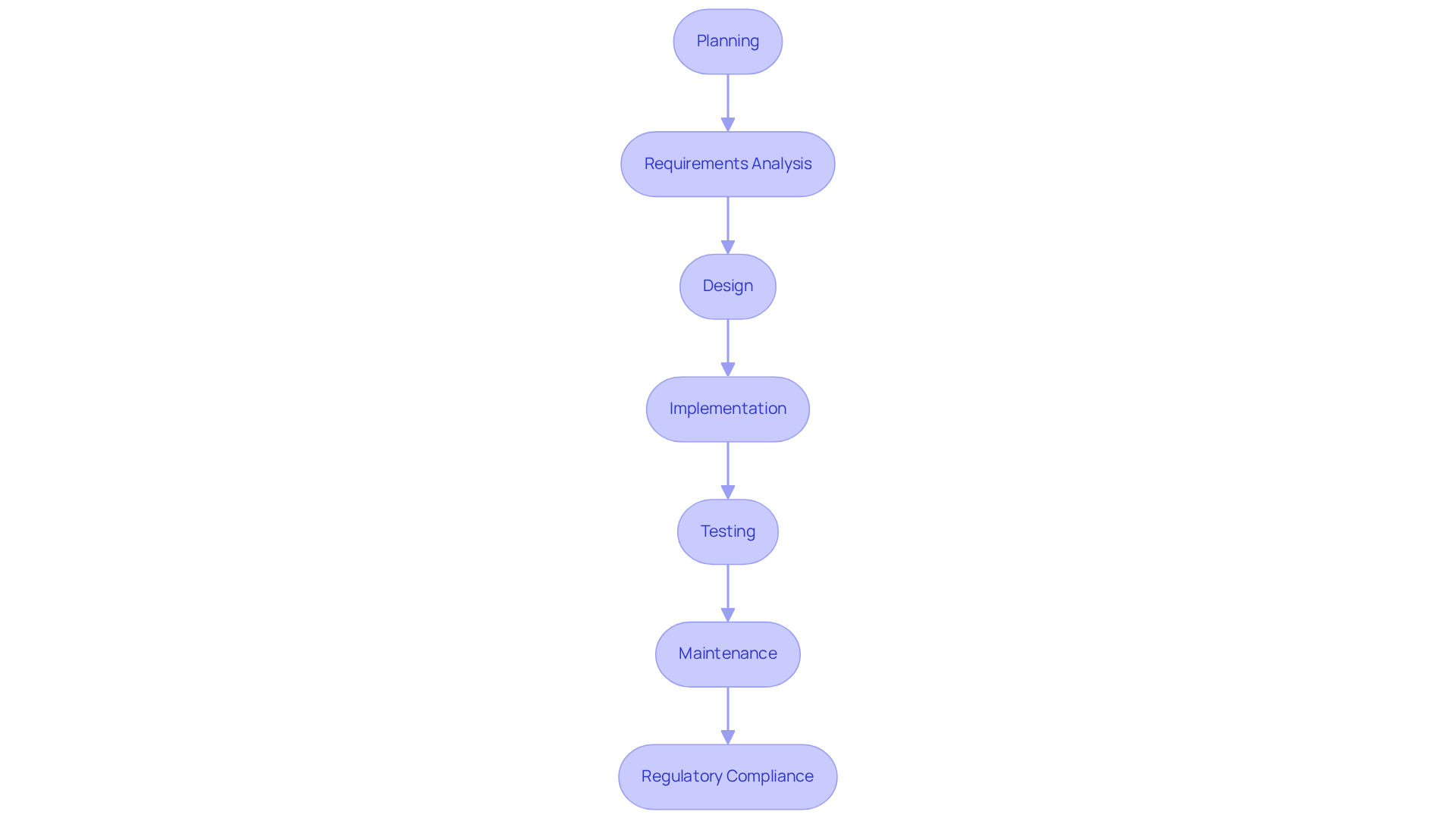
A structured Software Development Life Cycle (SDLC) is crucial for the efficient creation of programs in medical device software engineering. This SDLC encompasses all phases:
- Planning
- Requirements analysis
- Design
- Implementation
- Testing
- Maintenance
Each phase must adhere to regulatory requirements and quality standards, ensuring compliance throughout the process.
The IEC 62304 standard specifically outlines these life cycle processes, highlighting the significance of documentation and traceability at every stage. Recent updates to IEC 62304 introduce a new classification system that categorizes applications into Class A (low danger) and Classes B and C (high danger). This classification streamlines the and compliance efforts, enhancing overall safety and regulatory adherence.
Agile methodologies can be effectively integrated within this regulatory framework, allowing for iterative progress while maintaining compliance with necessary standards. By adhering to a structured SDLC, project teams can ensure that their medical device software engineering applications are not only efficient and user-centered but also compliant with all relevant regulations. This approach minimizes risks associated with non-compliance, such as market access delays and potential product recalls.
Ensure Continuous Testing and Validation
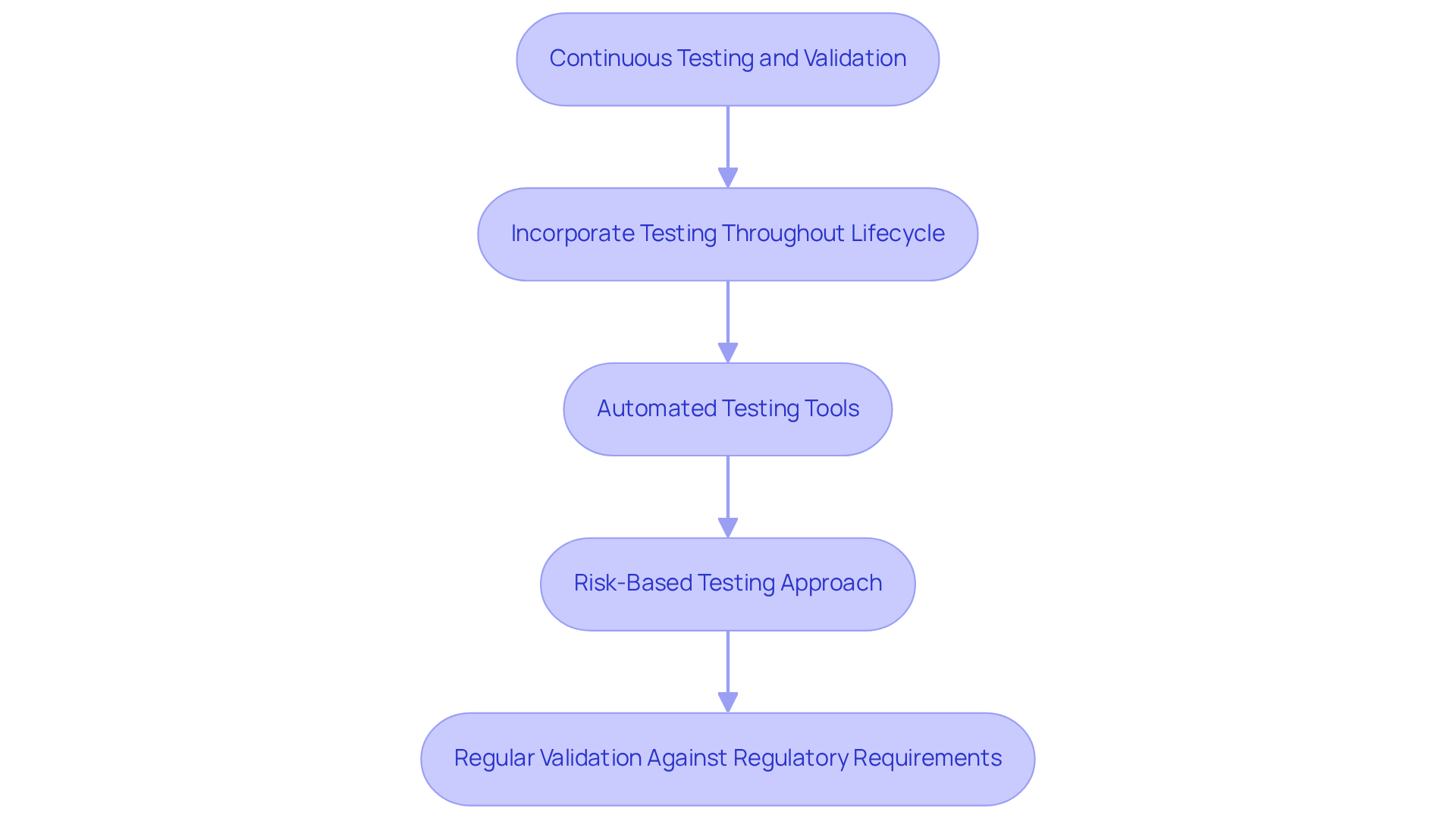
Ongoing testing and validation are essential in medical device software engineering for the development of medical device programs. In medical device software engineering, it is imperative to incorporate testing activities throughout the entire lifecycle of the program, rather than confining them to the final phases. Automated testing tools are pivotal in efficiently validating application functionality, performance, and security in medical device software engineering, thereby significantly enhancing the development process.
Adopting a risk-based testing approach is crucial, as it prioritizes testing efforts based on the severity and likelihood of identified risks. Regular validation against regulatory requirements, including those established by the FDA and ISO standards, is vital in medical device software engineering to ensure that the software remains compliant and safe for use. Additionally, comprehensive documentation of all testing activities is critical for demonstrating compliance during audits and inspections in medical device software engineering, reinforcing the integrity of the development process.
As the medical device industry evolves, the integration of automated testing tools within medical device software engineering is increasingly important. Currently, over 68% of enterprises are incorporating generative AI into their quality-engineering processes, reflecting a significant shift towards more efficient and reliable validation methods. The FDA’s updated guidance issued on January 6, 2026, further clarifies , emphasizing the necessity for transparency and independent evaluation in software recommendations.
Industry leaders have observed that leveraging automated testing tools in medical device software engineering not only streamlines the validation process but also mitigates risks associated with regulatory non-compliance. This makes such tools indispensable in today’s fast-paced development environment.
Conclusion
Navigating the complexities of medical device software engineering necessitates a comprehensive understanding of regulatory requirements and quality standards. By aligning development practices with frameworks such as FDA regulations and ISO standards, organizations can transform compliance from a daunting task into a strategic advantage. This approach not only enhances product safety and effectiveness but also fosters innovation in an increasingly competitive landscape.
Key practices include:
- Implementing effective risk management strategies
- Adopting a structured Software Development Life Cycle (SDLC)
- Ensuring continuous testing and validation
Each of these elements plays a critical role in mitigating risks associated with software development, ensuring that products meet the necessary safety and regulatory standards. The importance of thorough documentation and the integration of automated testing tools further strengthens compliance efforts, enabling teams to respond dynamically to evolving industry demands.
Ultimately, the significance of adhering to best practices in medical device software engineering cannot be overstated. As the industry continues to advance, embracing these guidelines will not only enhance compliance but also drive innovation and improve patient outcomes. Stakeholders are encouraged to prioritize these practices, ensuring that their products not only meet current regulatory expectations but also pave the way for future advancements in medical technology.
Frequently Asked Questions
What are the key regulatory requirements for medical device software engineering?
The key regulatory requirements include the FDA’s 21 CFR Part 820, which outlines the Quality System Regulation (QSR), and the upcoming transition to the Quality Management System Regulation (QMSR) effective February 2, 2026. Additionally, ISO 13485 specifies requirements for a quality management system, and adherence to ISO 14971 for managing uncertainties is crucial.
What is the Software Bill of Materials (SBOM) requirement?
The Software Bill of Materials (SBOM) requirement mandates developers to provide a detailed list of all software components used in their medical devices as part of FDA submissions. This requirement took effect in October 2023.
Why is compliance with regulatory standards important for developers?
Compliance with regulatory standards helps mitigate risks and enhances the safety and effectiveness of medical products. It also addresses the concerns that many companies have regarding the confidence in their quality management systems to support future growth.
What do industry leaders say about quality management systems?
Industry leaders emphasize the importance of aligning quality management systems with regulatory standards. They highlight that manufacturers must maintain complaint files and adhere to recordkeeping responsibilities, even if certain products are exempt from CGMP requirements.
What challenges do startups face in navigating regulatory requirements?
Startups often face challenges in navigating regulatory requirements due to a lack of expertise. It is recommended that they involve qualified clinicians to make informed decisions regarding patient safety.
How can companies integrate quality into product development?
Companies can integrate quality into every phase of product development by viewing compliance as a catalyst for innovation and differentiation rather than just a regulatory burden.
List of Sources
- Understand Regulatory Requirements and Quality Standards
- FDA Aligns U.S. Medical Device Rules with Global Standards (https://mddionline.com/regulatory-quality/medical-device-companies-must-navigate-historic-fda-rule-change)
- QMSR 2026 Explained: FDA Quality Management System Regulation & ISO 13485 Alignment Guide (https://sushvin.com/qmsr-2026-fda-quality-management-system-regulation.html)
- SAE Media Group (https://smgconferences.com/editors-corner/6630-news–fda-implements-quality-management-system-regulation-aligned-with-iso-13485)
- FDA Implements Quality Management System Regulation for Medical Devices (https://aabb.org/news-resources/news/article/2026/02/04/fda-implements-quality-management-system-regulation-for-medical-devices)
- 2025 Medical Device Industry Report | Greenlight Guru (https://greenlight.guru/state-of-medical-device)
- Implement Effective Risk Management Strategies
- 50 Risk Management Quotes: Wisdom for Smart Decision-making | ITD World (https://itdworld.com/blog/leadership/risk-management-quotes)
- Staying Ahead Of Medical Device Cyber Risk (https://forbes.com/councils/forbestechcouncil/2026/02/23/staying-ahead-of-medical-device-cyber-risk-how-visibility-collaboration-and-guidelines-help)
- Adopt a Structured Software Development Life Cycle (SDLC)
- Healthcare Software Development: Definition, Features, Building and Trends (https://kandasoft.com/blog/healthcare-software-development-trends)
- Navigating IEC 62304 Standard for Medical Software (https://cleio.com/insights/blog/navigating-iec-62304-standard-for-medical-software)
- IEC 62304 Update 2026: Key Changes & Compliance Tips (https://lfhregulatory.co.uk/iec-62304-update-2026)
- What You need to know about IEC 62304: Medical Software Lifecycle (https://securitycompass.com/blog/iec-62304-medical-software-lifecycle)
- How IEC 62304 Sparked a New Era in Medical Device Software Development (https://linkedin.com/pulse/how-iec-62304-sparked-new-era-medical-device-software-parchetalab-c6jnc)
- Ensure Continuous Testing and Validation
- Medical Device Software: Industry Statistics & Trends (https://ventionteams.com/blog/medical-device-software-statistics)
- FDA’s 2026 Guidance Expands Pathway for Low-Risk Digital Health Products—But Caution Remains Essential | Berkley Lifesciences (https://berkleyls.com/blog/fdas-2026-guidance-expands-pathway-low-risk-digital-health-products-caution-remains-essential)
- For 2026, FDA signals shifts in digital health framework | Nixon Peabody LLP (https://nixonpeabody.com/insights/alerts/2026/01/27/for-2026-fda-signals-shifts-in-digital-health-framework)
- FDA’s 2026 Expectations: Clinical Decision Support Compliance (https://about.citiprogram.org/blog/clinical-decision-support-compliance-fdas-2026-expectations)
- Continuous Testing Market Size, Share Analysis & Industry Trends Report, 2031 (https://mordorintelligence.com/industry-reports/continuous-testing-market)
