Introduction
Selecting the appropriate billing and coding software is a critical decision for healthcare organizations, as it significantly influences both operational efficiency and financial performance. Given the vast array of options available, it is essential to understand the key features and integration capabilities that can enhance workflow and ensure compliance. As practices face the complexities of software selection, it is vital to consider how their choice will not only address current needs but also adapt to future challenges within the continuously evolving healthcare landscape.
Identify Key Features for Healthcare Billing and Coding Software
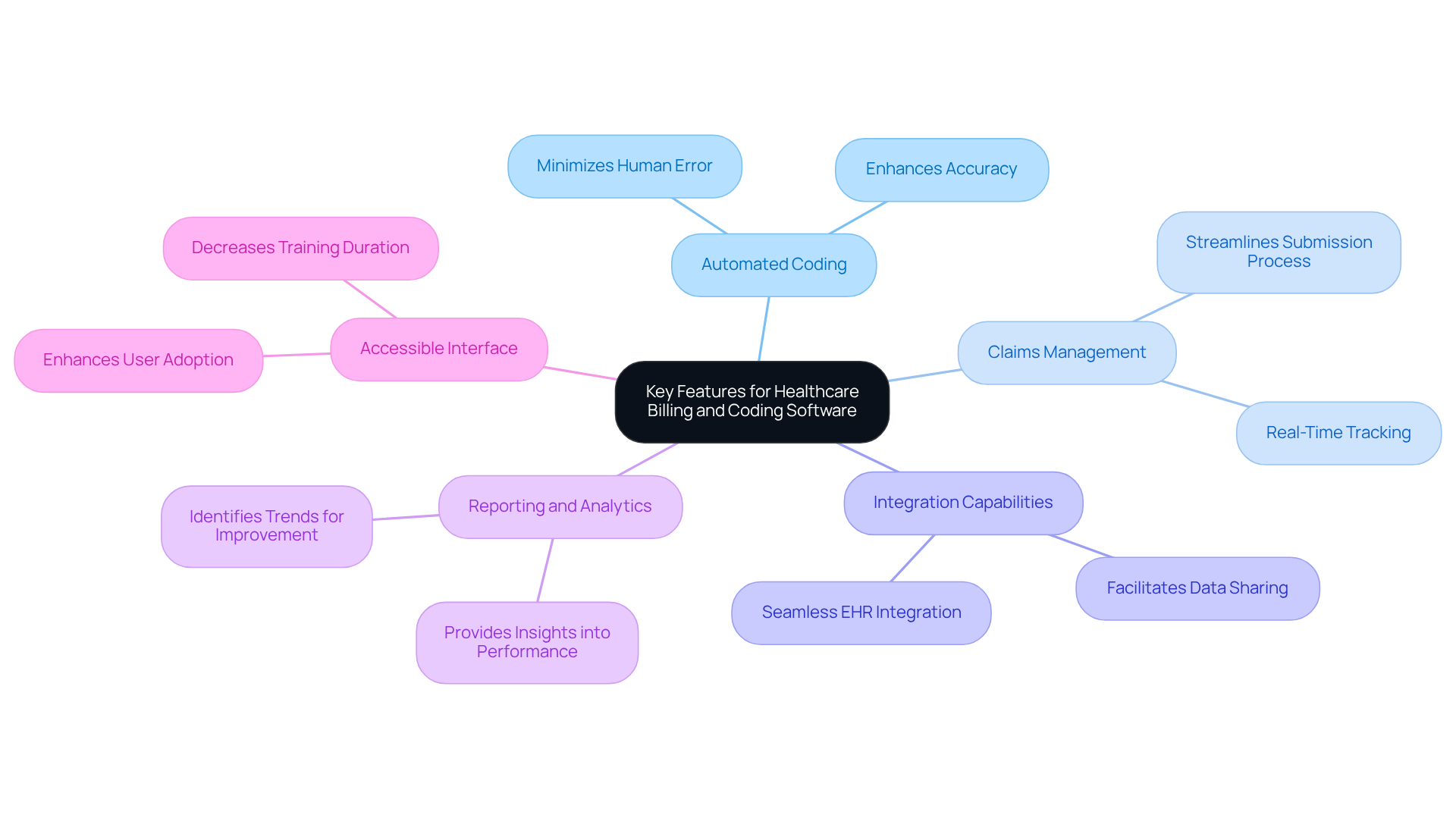
When selecting billing and coding software, it is crucial to identify key features that align with the specific needs of your practice. The following features should be prioritized:
-
Automated Coding: This feature minimizes human error by suggesting codes based on the patient’s diagnosis and treatment, thereby enhancing accuracy in billing.
-
Claims Management: Efficient claims management tools streamline the submission process and allow for real-time tracking of claims status, which is essential for timely reimbursements.
-
Integration Capabilities: It is vital to ensure that the software can integrate seamlessly with existing Electronic Health Records (EHR) systems. This capability facilitates data sharing and reduces redundancy, improving overall workflow.
-
Reporting and Analytics: Robust reporting tools provide valuable insights into billing performance, helping to identify trends and areas that require improvement, thus supporting informed decision-making.
-
Accessible Interface: A straightforward and intuitive interface significantly decreases training duration and enhances user adoption, making it easier for staff to utilize the software effectively.
By prioritizing these features, healthcare providers can select billing and coding software that not only complies with regulatory requirements but also enhances operational efficiency and accuracy.
Evaluate Usability and Integration with Existing Systems
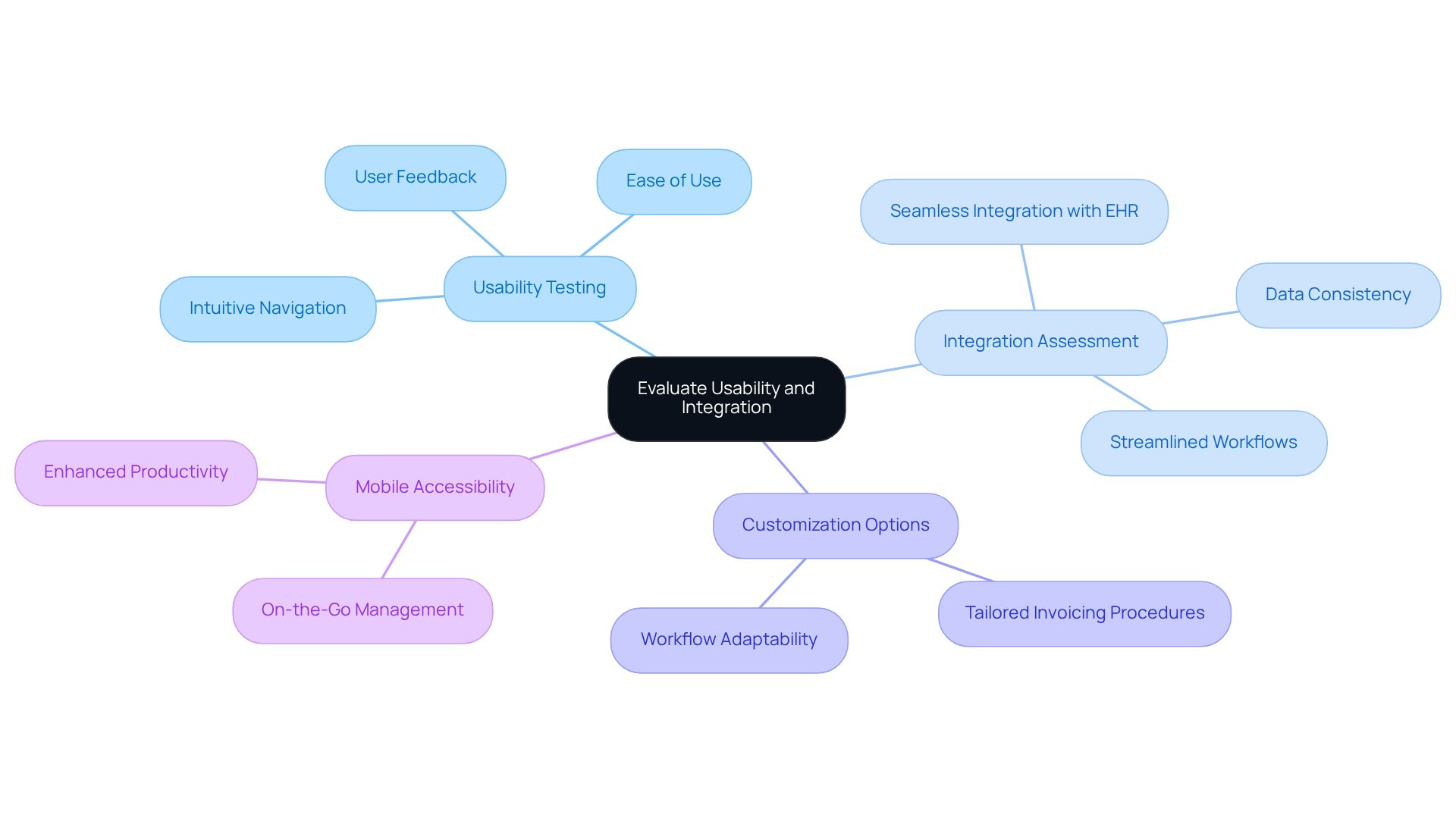
Evaluating the usability and integration capabilities of billing and coding software is essential to ensure its successful implementation.
Usability Testing: Conduct usability tests with potential users to gather feedback on the software’s interface and functionality. It is important to look for intuitive navigation and ease of use, as 88% of online consumers are less likely to return to a site after a bad experience. This can directly impact healthcare organizations’ revenue cycles.
Integration Assessment: Verify that the application can seamlessly integrate with your current EHR and practice management systems. This integration is crucial for maintaining data consistency and streamlining workflows. Practices utilizing billing and coding software along with integrated EHR-billing systems can achieve clean claim rates of 95-98% and reduce denial rates to under 5%, ultimately enhancing financial outcomes.
Customization Options: Evaluate whether the application permits customization to suit your specific invoicing procedures and workflows. Customized solutions can significantly improve operational efficiency and customer satisfaction.
Mobile Accessibility: Consider applications that provide mobile access, enabling staff to manage billing tasks on-the-go. This flexibility can enhance productivity, especially in fast-paced healthcare environments.
By concentrating on these aspects, healthcare organizations can select applications that not only fulfill their needs but also boost user satisfaction and operational efficiency, ultimately aiding in enhanced revenue cycle management. Furthermore, it is crucial to highlight that the administrative expense to redo a single rejected claim is $43-$57, and 65% of denied claims are never resubmitted, emphasizing the financial consequences of efficient system integration.
Ensure Compliance and Security Standards Are Met
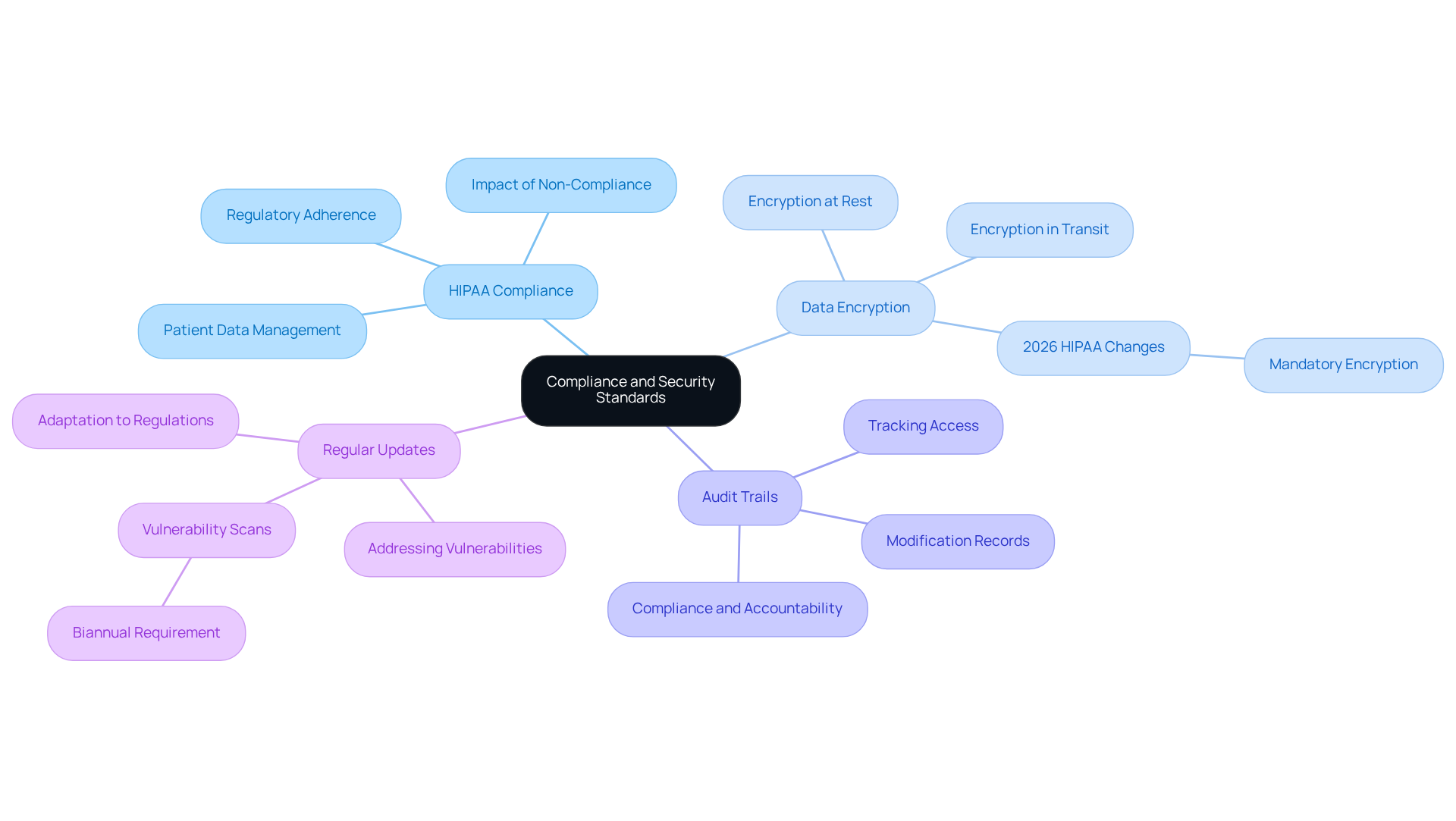
When selecting billing and coding software, ensuring compliance with all relevant security and regulation standards is crucial.
-
HIPAA Compliance: It is essential to verify that the software adheres to HIPAA regulations, which guarantees that patient data is managed securely and confidentially.
-
Data Encryption: Seek solutions that offer robust encryption for data both at rest and in transit. This is vital for protecting sensitive information from unauthorized access. Notably, the 2026 HIPAA changes mandate encryption for databases and backups.
-
Audit Trails: Ensure that the system maintains comprehensive audit trails. These are necessary for tracking access and modifications to patient data, which is critical for compliance and accountability.
-
Regular Updates: Choose applications that receive consistent updates to address security vulnerabilities and adapt to evolving regulations. Under the 2026 HIPAA changes, vulnerability scans must be conducted at least twice a year.
By prioritizing compliance and security, healthcare organizations can safeguard against potential legal issues while enhancing patient trust.
Prioritize Ongoing Support and User Training
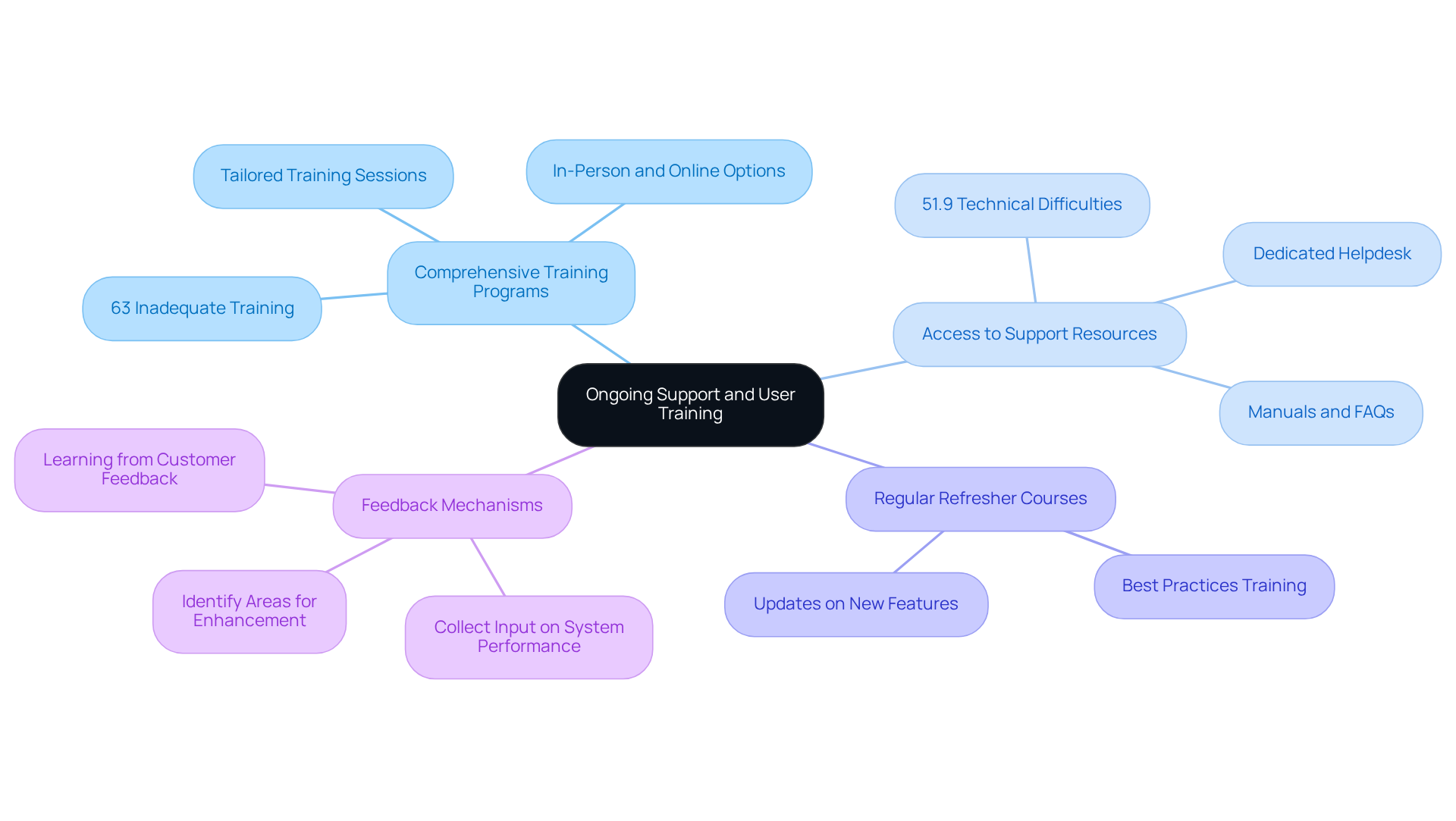
To maximize the benefits of the billing and coding software, it is essential to prioritize ongoing support and user training.
-
Comprehensive Training Programs: Implement training sessions tailored for all users to familiarize them with the software’s features and functionalities. A combination of in-person and online learning options can cater to diverse preferences, ensuring that all staff members are well-equipped to utilize the software effectively. Notably, 63% of respondents reported inadequate training in digital health technologies, underscoring the necessity for regular training initiatives.
-
Access to Support Resources: Individuals should have easy access to a variety of support materials, including manuals, FAQs, and a dedicated helpdesk for troubleshooting. This accessibility is crucial for resolving issues promptly and maintaining workflow efficiency. In fact, 51.9% of respondents cited technical difficulties and lack of support as major barriers to adopting digital health technologies, highlighting the need for robust support resources.
-
Regular Refresher Courses: Schedule regular refresher courses to keep staff updated on new features and best practices. Ongoing education can significantly improve precision and effectiveness, as it strengthens understanding and adapts to program updates.
-
Feedback Mechanisms: Establish strong feedback systems to collect input from individuals regarding system performance and identify areas for enhancement. As Bill Gates noted, “Your most unhappy customers are your greatest source of learning.” This feedback is crucial for guiding future development and assistance initiatives, ensuring that the system evolves to fulfill needs effectively.
Investing in ongoing support and training not only enhances user proficiency but also ensures that healthcare organizations can fully leverage their billing and coding software, which ultimately leads to improved operational outcomes.
Conclusion
Selecting the appropriate billing and coding software is a pivotal decision for healthcare providers, as it significantly influences operational efficiency, accuracy, and compliance. By identifying and prioritizing essential features – such as automated coding, claims management, integration capabilities, and comprehensive reporting tools – organizations can ensure they select software tailored to their specific requirements, thereby enhancing their revenue cycle management.
The article underscores the necessity of usability and integration, asserting that user-friendly software and seamless compatibility with existing systems are vital for successful implementation. Furthermore, adherence to security standards, particularly HIPAA, is crucial for safeguarding patient data and fostering trust within the healthcare community. Ongoing support and thorough training are equally important, as they enable staff to effectively utilize the software and adapt to updates, ultimately resulting in improved operational outcomes.
In conclusion, the choice of billing and coding software transcends a mere technical decision; it represents a strategic investment in the future of healthcare operations. By adhering to these best practices, organizations can not only refine their billing processes but also cultivate a culture of continuous improvement and adaptability. Emphasizing these elements will ensure that healthcare providers are well-prepared to navigate the complexities of billing and coding, ultimately benefiting both their practice and the patients they serve.
Frequently Asked Questions
What are the key features to look for in healthcare billing and coding software?
Key features to prioritize include automated coding, claims management, integration capabilities, reporting and analytics, and an accessible interface.
How does automated coding benefit healthcare billing?
Automated coding minimizes human error by suggesting codes based on the patient’s diagnosis and treatment, enhancing accuracy in billing.
Why is claims management important in billing software?
Efficient claims management tools streamline the submission process and allow for real-time tracking of claims status, which is essential for timely reimbursements.
What is the significance of integration capabilities in billing software?
Integration capabilities ensure that the software can seamlessly connect with existing Electronic Health Records (EHR) systems, facilitating data sharing and reducing redundancy.
How do reporting and analytics tools contribute to billing performance?
Robust reporting tools provide valuable insights into billing performance, helping to identify trends and areas for improvement, thus supporting informed decision-making.
Why is an accessible interface important for billing and coding software?
A straightforward and intuitive interface decreases training duration and enhances user adoption, making it easier for staff to utilize the software effectively.
How do these features impact operational efficiency and accuracy in healthcare practices?
Prioritizing these features helps healthcare providers select software that complies with regulatory requirements while enhancing operational efficiency and accuracy.
